| Annals of Burns and Fire Disasters - vol. X - n. 3 - September 1997
DERMOFUNCTIONAL
TREATMENT OF HYPERTROPHIC BURN SCARS
De Santis P., Savoia A.
Department of Plastic Surgery and Burn Unit,
Brindisi, Italy
SUMMARY. A review of the pathology of
hypertrophic bums is followed by an analysis of the results of a study of twenty
consecutive patients with hypertrophic bum scars. The patients were treated with
Synchroline, a cream compound consisting of an association of functional substances
capable of stimulating the biosynthesis of the macromolecules responsible for skin
pliability and elasticity The criteria for the selection of patients were the presence of
deep hypertrophic bum scars, an average burned surface of 20%, and the use of pressure
garment therapy. Each patient treated was matched with a control patient selected among
patients treated by other physicians working in the same Burn Unit. The patients were
matched for age group, scar site, and duration of treatment with hydrating creams and
pressure garments. All the patients were followed up monthly and the scar was assessed by
a physician in the Burn Unit who was unaware of the patients' group membership. The
following scar characteristics were assessed: appearance, consistency, presence of
nodules, coloration, and presence of ulcers. One patient underwent two hypertrophic scar
biopsies: at the beginning of treatment and after six months. Our results indicate that
hypertrophic scars in the Synchroline group were more elastic and pliable at six months
than those in the hydrating cream group. The effect of Synchroline as a precursor and
stimulator of hyaluronic acid, fibronectin and soluble collagen biosynthesis is discussed.
Introduction
Hypertrophic scars are a frequent outcome after the healing of deep
bums and represent the greatest disorder of the scarring process. The main features of
hypertrophic bum scars are the continuous production of collagen, a remodelling defect in
cell structure and the extracellular matrix, the abundant presence of infiltrated cells,
and the absence of elastic fibres. Morphologically, hypertrophic bum scars present a less
mucoid matrix, together with collagen hyaline fibres. Elastic fibres are less numerous or
absent. The fibroblasts assume the structure and properties of smooth muscles in the
contraction processes of granulation tissue. These modified fibroblasts, or
myofibroblasts, that are observable in granulation tissue after the formation of collagen
fibres are important in establishing the direction of the fibres.
In hypertrophic scars, myofibroblasts are ineffective in establishing the direction of the
collagen mass.These structural differences in the hypertrophic scar may be responsible for
differences in mechanical properties, such as increased stretch resistance. The increase
in collagen deposited in hypertrophic scars has been thought to be due to increased
synthesis or a deficit in collagen lysis .... .. Collagen synthesis is greatly increased,
while at the same time there is a decrease in the availability of active collagenase. The
enzymes involved in the transformation of protocollagen into collagen are proline
hydroxylase and lysine hydroxylase. Their activity increases considerably in granulation
and scar tissue. The increase in collagen synthesis may be due to the increased number of
actively secreting fibroblasts or to increased enzymatic activity.
Hypertrophic scars contain large amounts of type III collagen. This substance may affect
the resistance of fibres to stretch and thus be responsible for the different stretch
resistance shown by normal dermis and by bum tissue.` The hydroxylysine and hexose content
of the dermis and the scar is different. Collagen is catabolized by collagenase, a
proteolytic enzyme available in inactive form in the skin and inhibited by the alpha
globins.` It has been hypothesized that this inhibition is more marked in hypertrophic
scars. A higher concentration of chondroitin-4-sulphate (proteoglycans) has been observed
in nodular areas of hypertrophic scars.` The increased concentration of proteoglycans,
coupled with large amounts of chondroitin-4sulphate, contributes to the overdeposition of
collagen.
Hypertrophic scars display an increased amount of glycosaminoglycan-proteoglycan, and a
three-dimensional architecture compared with normal scars. The increase in
glycosaminoglycans may protect collagen from collagenase remodelling, thus allowing it to
be stored. This mechanism may also be responsible for scar hypertrophy. The amount of
dermatan sulphate is highly reduced in hypertrophic sears, especially in areas where
collagen turns spiral-shape. The quantity of glycosaminoglycans and hyaluronic acid in the
scar varies: there may be a close relationship between glycosaminoglycan-collagen and
collagenase activity, as they interact in such a way that any modification of one factor
affects all the others. Hyaluronic acid limits the conversion of extensible soluble
collagen to rigid insoluble collagen, slowing down the formation of intermolecular cross
links. The organization of collagen fibrils may be related to the quantity and type of
proteoglycans, which possibly influence the growth and remodelling of the extracellular
matrix - the links between proteoglycans and collagen are in fact stronger in hypertrophic
scars and can stabilize the plot of collagen fibrils?' The newly produced collagen is
unevenly stored in the hypertrophic scar, where it adheres through rapid intermolecular
formation of crosslinking, giving the fibrils increased resistance to stretch. A slowdown
of this process would give collagen molecules a more physiological organization. It has
been hypothesized that a temporary delay in collagen cross-link formation may facilitate
tissue remodelling and thus create softer tissue.
Synchroline is an association of functional substances capable of stimulating the
biosynthesis of the macromolecules responsible for skin elasticity and pliability. The
components of Synchroline are as follows: Asian acid from Hydrocotyle extract;
N-acetyl-D-glucosamine; proline linoleate, proline linolenate, and proline arachidonate;
and the reduced enzymatic fraction of fibronectin. The effect of Synchroline is that of
both stimulator and precursor of hyaluronic acid, fibronectin and soluble collagen
biosynthesis. Asian acid, which is responsible for Synchroline's stimulatory effect on the
amorphous and fibrous component of the dermis, acts directly on collagen biosynthesis,
improving its quality. This effect is apparently due to the increased incorporation of
fibrin in the fibroblast. Proline linoleate is the precursor of collagen present in
Synchroline and guarantees the amino acid necessary for collagen biosynthesis. The
combined action of Asian acid and proline linoleate stimulates collagen biosynthesis.
Asian acid stimulates use of the acetate in the glycosaminoglycans. N-acetyl-D-glucosamine
is a natural molecule and an active metabolite of UDP-N-acetylglucosamine, which is
essential for the formation of the monomer of hyaluronic acid after conjugation with
glycuronic acid.
 |
 |
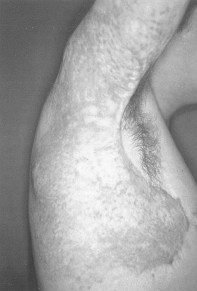
| Fig. 1 - Patient with
hypertrophic burn scar in right shoulder. Elastocompressive and topical therapy initiated
two weeks after healing. |
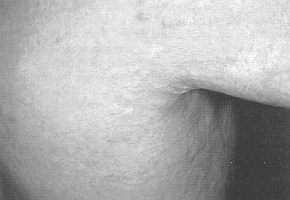
Fig. 2 - Result after
six months treatment. |
|
The combined action of Asian acid and N-acetylD-glucosamine enables
Synchroline to support production of hyaluronic acid. An increase in the biosynthesis of
fibronectin on the fibroblast walls has been observed with Asian acid. The reduced
enzymatic fraction of fibronectin available in Synchroline is characterized by the
presence of the tetrapeptide I-arginyl-glycyl-l-aspartyl-l-serine,which is the fragment of
the molecule responsible for the cell's adhesiveness. This fraction acts as a precursor of
fibronectin biosynthesis.
Materials and methods
Twenty consecutive patients were treated for six months with
Synchroline, an association of functional substances able to stimulate the biosynthesis of
the macromolecules responsible for skin elasticity and pliability.
The criteria for the selection of patients were deep hypertrophic bum scars, an average
bum surface of 20%, and the use of pressure garment therapy. Each patient was matched with
a control patient, selected among patients treated in the same Burn Unit. Each patient was
matched as regards age group, scar site, and duration of treatment with hydrating creams
or pressure garments (Tab. 1). In all, forty patients were recruited and followed
up monthly.
| |
Terproline |
Hydrating creams |
| Sex |
M |
14 |
12 |
| F |
6 |
8 |
| Age (yr) |
5-15 |
11 |
7 |
| 6-40 |
9 |
13 |
| % body surface burned |
|
22.3 |
21.1 |
| Initiation treatment |
(day 15) |
13 |
12 |
| after healing |
(day 15) |
7 |
8 |
Burn area |
|
|
|
| - thorax |
|
1 |
1 |
| - trunk |
|
6 |
6 |
| - thorax/upper limbs |
|
10 |
10 |
| - abdomen/ower limbs |
|
3 |
3 |
|
Table I - Characteristics of patients
subjected to pressure garment therapy treated |
|
A number of scar characteristics were assessed at the beginning of
treatment and after six months; assessment was performed by a specialist in the Burn Unit
who was unaware of the patients' group membership. The major points considered and
evaluation criteria were:
- scar appearance (photographs before treatment and after six months)
- scar consistency (resistance): retracting, 5 points; compact, 3 points; soft, I point
- palpation: with solid nodules, 5 points; with soft nodules, 3 points; without nodules, 1
point
- coloration: intensely hypaeremic, 5 points; moderately reddened, 3 points; similar to
surrounding skin, I point
- One patient treated with Synchroline underwent two scar biopsies: one at the beginning
of treatment and the other after six months.
Results and conclusions
The two groups of patients were comparable as regards their main
characteristics. Scar evaluation results at six months are presented in Table II.
| |
Terproline |
Hydrating
creams |
| Points |
(%) |
Points |
(%) |
| Consistency |
Before |
86 |
(4.3) |
82 |
(4.1) |
| After |
40 |
(1.3) |
51 |
(2.5) |
| Palpation |
Before |
84 |
(4.2) |
84 |
(4.2) |
| Nodules |
After |
46 |
(2.3) |
52 |
(2.6) |
| Coloration |
Before |
100 |
(5.0) |
100 |
(5.0) |
| After |
40 |
(2.0) |
60 |
(3.0) |
|
Table II - Summary of major
points considered |
|
The hypertrophic scars of the Synchroline-treated patients were more
pliable and elastic than those in the hydrating cream group. Another remarkable result was
the lack of ulcers in the crisis areas in Synchroline-treated patients. This early and
better response may be due to the effect of the association of functional substances on
the production of hyaluronic acid, fibronectin, and soluble collagen.
RESUME. Les Auteurs, après avoir considéré
la pathologie des cicatrices hypertrophiques dues aux brûlures, analysent les résultats
d'une étude de vingt patients consécutifs atteints de cicatrices hypertrophiques dues
aux brûlures. Les patients ont été traités avec Synchroline, un composé crémeux qui
consiste en une association de substances fonctionnelles capables de stimuler la
biosynthèse des macromolécules responsables de la flexibilité et l'élasticité de la
peau. Les critères pour la sélection des patients étaient la présence de cicatrices
hypertrophiques profondes dues aux brûlures, une surface brûlée moyenne de 20%, et
l'emploi de la pressothérapie. Chaque patient traité a été confronté avec un patient
témoin, sélectionné parmi les patients traités par d'autres médecins de la même
Unité de Brûlures. Les patients ont été confrontés sur la base de l'âge, le site de
la cicatrice, et la durée du traitement avec les crèmes hydratantes et la
pressothérapie. Tous les patients ont été contrôlés tous les mois quand la cicatrice
a été évaluée par un médecin de l'Unité de Brûlures qui ne connaissait pas la
division des patients en groupes. Les caractéristiques suivantes des cicatrices ont été
évaluées: aspect, consistance, présence de nodules, coloration, et la presence,
d'ulcères. Un patient a subi deux biopsies des cicatrices hypertrophiques: au
commencement du traitement et après six mois. Les résultats de l'étude indiquent que
les cicatrices dans le groupe traité avec Synchroline étaient plus élastiques et
flexibles à six mois que celles du groupe traité avec la crème hydratante. Enfin, les
Auteurs discutent l'effet de Synchroline comme précurseur et stimulateur de l'acide
hyaluronique, de la fibronectine et de la biosynthèse du collagène soluble.
BIBLIOGRAPHY
- Brody G.S.: Keloids and hypertrophic scars. Plast. Reconstr. Surg., 86:804,1990.
- Cohen I.K., Keiser N.R., Sjoerdsma A.: Collagen synthesis in human keloid and
hypertrophic scar. Surg. Forum, 22: 488, 1971.
- Cohen I.K., Diegelmann R.F.: The biology of keloid and hyper trophic scar and the
influence of corticosteroids. Clin. Plast. Surg., 4:297,1977.164
- Deitch E.A., Wheelahan T.M., Rose M.P. et al.: Hypertrophic burn scars: analysis of
variables. J. Trauma, 23: 895, 1983.
- Ehrlich H., Desmouliere A., Diegelmarm R., Cohen I.K. et al.: Morphological and
immunochemical differences between keloid and hypertrophic sear. Am. J. Pathol., 145: 105,
1994.
- Eisen A.Z., Bauer E.A., Jeffrey J.J.: Human skin collagenase. The role of serum alpha
globulins in the control of activity in vivo and in vitro. Proc. Natl. Acad.
Sci., 68: 248, 1971.
- Enzinger F.M., Weiss S.W.: Keloid. In: "Soft tissue tumors", CX Mosby Co., St.
Louis, Toronto, London, 1983.
- Gabbiani G., Ryan G.B., Majno G.: Presence of mochfied fibroblast in granulation tissue
and their possible role in wound contraction.Experientia, 27: 549, 1971.
- Grant M., Prockop D.: The biosynthesis of collagen. N. Engl. J.Med.: 286, 194, 242, 291,
1972.
- Ketchum L.D., Cohen 1. et al.: Hypertrophic scars and keloids. Plast. Reconstr. Surg.,
53: 140, 1974.
- Larson D.L., Abston S., Willis B. et al.: Contracture and sear formation in the bum
patient. Clin. Plast. Surg., 1: 653, 1974.
- Lareson D.L., Baur P., Linares H.A. et al.: Mechanisms of hypertrophic scar and
contracture formation in burns. Burns, 1: 119,1975.
- Linares H.A., Kischer C. W, Dobrkovsky M. et al.: On the origin of hypertrophic scars.
J. Trauma, 13: 70, 1973.
- Linares H.A.: Los miofibroblastos en las cicatrices hypertroficas: j causa o
consequencia? Cit. Plast. lbero Latinoamer., 5: 207, 1979.
- Linares H.A.: Measurement of collagen-proteoglycan interaction in hypertrophic scars.
Plast. Reconstr. Surg., 71: 818, 1983.
- Lynch W.S.: Wound healing. In: Epstein E., Epstein E., jr: "Skin surgery",
W.B. Saunders Co., Philadelphia, 1987.
- Magliacani G., Cavallero M., Bormioli M.: Prolina idrossilasi e acido lattico nella
cicatrice da ustione. Riv. Ital. Chit. Plast., 9: 233, 1977.
- McGrouther D.: Hypertrophic or keloid scars? Eye, 8: 200, 1994.
- Peacock E.E., jr, Madden JW.: On the use of lathyrogens in human biology. Surgery, 71:
922, 1972.
- Ryan G.B., Cliff W.J., Gabbiam G., lrl~ C. et al.: Myofibroblasts in human granulation
tissue. Hum. Pathol., 5: 55, 1974.
- Shetlar M.R., Shetlar C.L., Chien S.R: The hypertrophic location of glycosaminoglycans
within scars. Burns, 4: 14, 1978.
- Stella M., Castagnoli C., Magliacam G., Richiardi P.: Fisiopatologia della
cicatrizzazione patologica. Riv. Ital. Chit. Plast., 21: 199, j1989.
- Tanzer M.: Cross-linking of collagen. Science, 180: 561, 1973.
- Thomas D.W., Hopkinson L, Harding K.G., Shepherd J.P.: The pathogenesis of
hypertrophic-keloid scarring. Int. J. Oral Maxillofac. Surg., 23: 232, 1994.
- Younai S., Nichter L.S. et al.: Modulation of collagen synthesis by transforming growth
factor-beta in keloid and hypertrophic scar fibroblasts. Ann. Plast. Surg., 33: 148, 1994.
This paper was received on 16 May 1997.
Address correspondence to: Dr P. De Santis
Divisione di Chirurgia Plastica e Centro Ustioni
Brindisi, Italy. |
|

