| Annals of Burns and Fire Disasters - vol. XI - n. 3 - September
1998
HIGH-TENSION
ELECTRICAL BURNS
Faggiano G., De Donno G., Verrienti P., Savoia A.
Centro Ustioni, Ospedale Di Summa, Brindisi, Italy
SUMMARY. Electrical burns have
traditionally been considered as distinct from thermal burns. The management of
high-voltage electrical burns, in particular, poses certain therapeutic challenges for the
surgeon. We present our experiences with a series of such patients admitted to the Burn
Unit of Brindisi Hospital (Italy).
Introduction
Electrical burns occur less frequently
than flame or liquid burns, but they give rise to a series of very complex problems. They
account for 3-9% of all patients treated in burns centres. Such cases are distinguished as
highvoltage burns (over 1000 V) and low-voltage burns (less than 1000 V).
An electric current can cause two types of tissue damage, due to:
- local generation of heat owing to passing of current (main
mechanism)
- direct action (mechanism not fully understood), probable
damage to endothelial membrane
The factors determining the degree of
tissue damage are shown in Table I.
Voltage
Amperage
Resistance
Contact time
Pathway of current
Type of current |
|
| Table 1 - Factors causing tissue damage |
|
Voltage (V) is the electromotor force
generated by a power, while amperage (A) is the intensity of the electric current per unit
of time; they are related by the formulae A = V/J and J = IRT. The joule (J) is the heat
produced by the current (1) when it meets a resistance (R) during its passage per time
unit (T); the resistance depends on the quantity of water in the tissues, water being a
good conductor.
The most resistant tissues are bone, followed by fat, tendon, skin, muscle, vessels and
nerves (Tables II, III).
Bone
Fat
Tendon
Skin
Muscle
Vessel
Nerve |
|
Wet skin
= 1,000 ohm/cm2
Dry skin
= 10,000 ohm/cm2
Calloused palm skin = 1,000,000 ohm/cm2 |
|
| Table II - Resistance to passage of current |
Table
III - Skin resistance |
|
In high-voltage burns the entry point of
the current is the area of contact with the electric source; the exit point is often an
area of damp skin such as the sweaty areas of the axilla, the sole of the foot, the elbow
and the hands.
The severity of the burn is directly proportional to the duration of the contact, although
even extremely short exposure to high-voltage current can cause massive tissue damage.
The pathway of the current is unpredictable but usually follows the vessels, as these
offer least resistance.
The passage of current from one hand to the other is extremely dangerous because in this
case it passes through the thorax, with an elevated rise of cardiac fibrillation.
Material and methods
A retrospective analysis was carried out
with regard to four patients suffering from high-voltage electrical burns admitted to our
burns centre in Brindisi, Italy, over a oneyear period (Table IV).
Patient
reference |
% TBSA |
Number of
debridements |
Cardiac
symptoms |
Fasciotomy |
Hospital
stay (days) |
M.C. |
5 |
1 |
No |
No |
35 |
L.T.R. |
25 |
- |
- |
No
(deceased) |
4 |
M. M. |
12 |
2 |
No |
Yes |
50 |
S.M. |
10 |
2 |
No |
No |
60 |
|
| Table IV - Patients admitted |
|
All the patients were male; the mean
voltage was 15,000 V; the patients were admitted to the burns centre within 3 h of the
accident; the current entry point was the lower limbs (two cases), the right thigh (one
case), and the right buttock (one case).
The mean burned body surface area was 12%; no patient required cardiovascular
resuscitation; all four patients received infusion therapy (Baxter formula); one patient
was subjected to fasciotomy of the upper limb, with topical treatment involving use of
silver sulphadiazine and salicylic vaseline; and several surgical debridement procedures
were performed, with skin graft coverage. One patient, suffering from advanced AIDS, died
on day 4; the other three patients were discharged after about 50 days.
Discussion
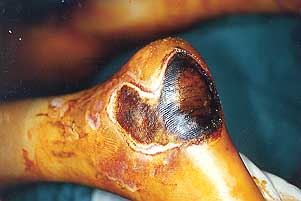
In high-voltage burns the body surface
involved is often relatively limited, but all the burns are deep, unlike those caused by
electric tlash (Figs. 1a, 1b, 2a, 2b).
 |
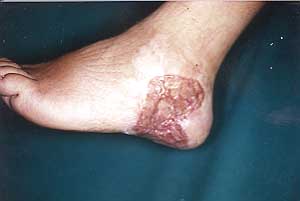 |
Fig. la
- Electrical burn. |
Fig. 2a
- Electrical burn. |
 |
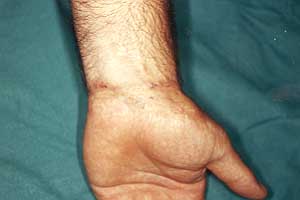 |
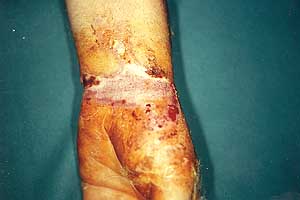
Fig. lb
- Electrical burn. |
Fig. 2b
- Electrical burn. |
|
The skin at the entry point often appears
mummified and depressed, with a clear outline due to the rapid evaporation of water. The
skin adjacent to the exit point is often ulcerated, with the formation of outwardly
oriented craters that conceal deep and severe muscular lesions.
The deep tissues are damaged by the direct action of the heat produced, by progressive
devascularization secondary to thrombosis, or by the inevitable infections. In typical
cases the muscle is dark in colour, noncontractile, not bleeding: the hand looks as if it
has been boiled.
Sometimes a compartment syndrome develops because of massive perilesional oedema, with an
increase in cutaneous tension that may exceed 30 mm Hg and a consequent loss of tissue
perfusion. In such situations fasciotomy becomes imperative. This is performed along the
major axis of the limb, as in escharotomy. The underlying muscle is then inspected, and
debridement is thus facilitated. Early debridement of the muscle and necrotic tissue, and
if necessary the amputation of nonviable extremities, reduce the risk of infection and the
possibility of renal damage due to massive myoglobinuria.
Tissue cleaning may have to be repeated several times; definitive coverage is performed
when there is no more devitalized tissue. In our patients coverage was effected on about
day 20 using full-thickness autologous skin grafts.
Cardiac complications in this type of patient range from reversible asystoles to systemic
hypertension, hypovolaemic shock, and the rupture of aneurysms of large vessels.
Death is often due to acute kidney failure with massive myoglobinuria, to DIC
(disseminated intravasal coagulation), or to direct damage caused by the electric current.
The central nervous system may be involved either directly or subsequently; the literature
contains cases of coma of varying gravity, hemiplagia, aphasia and epilepsy.
Peripheral neuropathies are very frequent as a result of direct damage by the current to
the nerve myelin or because of vascular thromboses; these consequences cause irreversible
and very incapacitating damage.
The bone structure is also frequently involved in highvoltage electric burns as a result
of violent muscular spasms that cause fractures as a result of direct destruction of the
bone by heat or devascularization. Hydroclectrolytic hydrating treatment is based on the
same principles as those followed in classic flame burns, with the use of Ringer's lactate
or hypertonic solutions, except that the quantity of fluid necessary to obtain
satisfactory renal and tissue perfusion is approximately double the normal amount, and
particular attention has to be paid to the presence of myoglobinuria, which requires a
considerable wash-out in order to prevent the precipitation of pigments in the renal
tubules.
If this risk is present, an infusion of mannitol maintains a more effective diuresis.
There is a high risk of Staphylococcus aureus and Pseudomonas aeruginosa infection
in these patients. flowever, wide-range antibiotic prophylaxis is not recommended. Topical
therapy with silver sulphadiazine will reduce the bacterial charge.
Conclusions
Our experience in the field of electric
burns confirms the absolute priority of appropriate infusion therapy in the first hours
post-burn, special care with regard to the current entry point, and early surgical
treatment with subsequent skin coverage by means of free grafts or local and distant
flaps.
RESUME. Il est tradition de
considérer les brûlures électriques comme un problème distinct de celui posé par les
brûlures thermiques. La gestion des brûlures électriques causées par la haute tension
pose des problèmes thérapeutiques particuliers pour le chirurgien. Les Auteurs
presentent leurs expériences avec des patients de ce type traités dans l'Unité de
Brindisi (Italie).
BIBLIOGRAPHY
- Baxter C.R.: Present concepts in the management of major
electrical injury. Surg. Clin. North Am., 50: 1401, 1970.
- Skoog T.: Electrical injuries. J. Trauma, 10: 816, 1970.
- Daniel R.K., Ballard P.A., Heroux P. et al.: High-voltage
electrical injury: acute pathophysiology. J. Hand Surg., 13A: 44, 1988
- Cabanes J.: Prevention des brGlures 6lectriques. Ann.
Medit. Burns Club, 4: 38-41, 1991.
- Luce A.E., Gottlieb J.: "True" high-tension
electrical injuries. Am. Plast. Surg., 84: 321, 1984.
- Zelt R.G., Daniel R., Ballard P. et al.: High-voltage
electrical injury: chronic wound evolution. Plast. Reconstr. Surg., 82: 1027, 1988.
- Lee R.C., Gottlieb J., Krizak T.: Pathophysiology and
clinical manifestations of tissue injury in electrical trauma. Adv. Plast. Reconstr.
Surg., 8: 1, 1992.
- Luce E.A.: Electrical injury. In: McCartey, "Plastic
Surgery", Saunders, Philadelphia, vol. 1, chap. 24.
- Logan M.A.: Electrical burned caused by fishing rod contact
with overhead electric cables. Burns, 19: 535, 1993.
| This paper was received on 25 March
1998. Address correspondence to:
Dr G. Faggiano
Centro Ustioni, Ospedale Di Summa
Brindisi, Italy. |
|



