Annals of
Burns and Fire Disasters - vol. XII - n° 4 - December 1999
ABDOMINAL WALL RECONSTRUCTION IN AN ELECTRICAL BURN WITH A MYOCUTANEOUS
TENSOR FASCIAE LATAE ISLAND FLAP. CASE REPORT
Cavadas P.C.
La Fe University Hospital, Valencia, Spain
SUMMARY. High-voltage
electrical injuries often cause full-thickness defects in the abdominal wall, which are
difficult to reconstruct. A case is reported of periumbilical reconstruction using a
tensor fasciae latae (TFL) myocutaneous flap in an 8-yr-old boy who had sustained severe
electrical injuries. The operative procedure is described, in which a right TFL
myocutancous island flap was used. The treatment described led to satisfactory results.
General considerations
Reconstruction of
full-thickness defects in the abdominal wall is a difficult problem that is sometimes
encountered in the treatment of high-voltage electrical injuries. In the acute situation
of explosive exit wounds in the abdomen, with traumatic evisceration, it has been
recommended that skin grafting should be performed in the granulating peritoneal surface,
although reconstruction of a competent abdominal wall will later prove necessary.
Local cutaneous or fasciocutaneous flaps can be based medially on anterior midline
perforators, laterally on intercostal perforators, cranially on superficial superior
epigastric vessels, and caudally on superficial inferior epigastric vessels. Bogart et al.
reported on the use of a bilateral groin flap to repair a large defect after desmoid
tumour resection. Little et al. described a sensate upper quadrant flap based on
intercostal bundles.
Farr described a thoracic myofascial flap for upper abdomen reconstruction. In 1934
Wargensteen first reported on the use of the tensor fasciae latae (TFL) myofascial flap
for wide infrared umbilical defects. Wargensteen also stated that even in patients with
very long femurs, the TFL is not long enough to reconstruct subcostal defects. Watson
described the extended TFL up to the knee joint for the reconstruction of supraumbilical
defects. The external oblique muscle flap was used by Hershey and Butcher for
supraumbilical abdominal defects.
Boswick et al. described the extended latissimus dorsi flap and Houston et al. reported on
its use in reconstruction of large incisional hernia. In 1977 Mathes and Boswick, using a
previous work of Brown et al., described the use of a superiorly based rectus abdominis
myocutaneous flap for upper abdominal defects. The inferiorly based rectus abdominis flap
has been widely used for upper abdomen reconstruction. Taylor et al. described the
extended rectus abdominis myocutaneous flap for abdominal wall reconstruction. Cormack and
Quaba reported on the use of a bilobed extended rectus abdominis flap for massive
abdominal reconstruction.
A clinical case is reported of periumbilical reconstruction with a TFL flap.
Case report
An 8-yr-old male had
sustained a high-voltage electrical injury one yr before presentation, with left
above-knee amputation, severe hand injuries, and a 13 x 9 em perisupraumbilical hernia.
The hernia resulted from the exit wound, which was skingrafted directly over the
peritoneum. There was heavy scarring in the upper abdomen.
The reconstruction of the hernia was performed with a right TFL myocutaneous island flap,
after excision of the abdominal skin graft (Figs. 1-3).
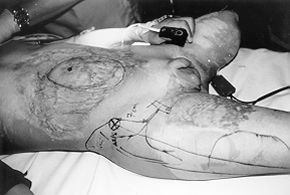 |
Fig. 1
- Skin markings for the procedure, depicting the, defect, the tensor fasciae latae muscle,
the skin island, and the lateral circumflex femoral vessels. |
|
|
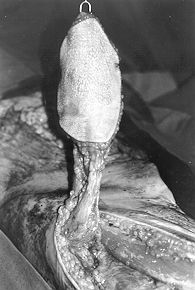
Fig.
2 - Full-thickness defect and flap ready to be transposed. The lateral circumflex
femoral vessels can be seen in the base of the flap. |
|
The
supporting structure of the reconstruction was made up of vascularized fascia lata from
the flap. The flap was completely elevated, disinserting the muscle from the anterior
superior iliac spine.
Approximately one-quarter of the distal skin island was lost, although the fascia remained
vital and accepted a skin graft after partial debridement. The final result was
satisfactory in terms of the recovery of abdominal wall competence (Fig. 4).
 |
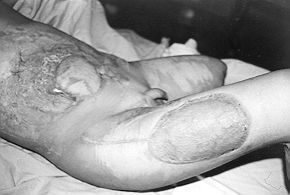 |
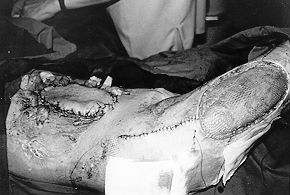
Fig. 3 - Immediate post-operative result. The donor
tensor fasciae latae area was skingrafted. |
Fig. 4 - Late post-operative result. The distal part was
debrided and skin was grafted over the viable fascia. |
|
Discussion and
conclusion
Upper abdominal wall
defects can be a difficult problem when both recti abdominis muscles are lost. In general
the most widely accepted choices for this situation are either a laterosuperiorly based
external oblique muscle flap or a TFL flap. In the case reported here, an external oblique
muscle flap was ruled out because of heavy scarring in the upper abdomen, with probable
injury of the muscle, and a TFL flap was therefore preferred. Although Watson has stated
that the TFL flap, when extended up to the knee joint, permits reconstruction of the upper
abdomen, opinions vary as regards the safety of this extension. In the case reported here,
the distal. end of the flap was 4 cm above the knee joint. The distal skin (not fascia)
necrosis could have been due to excessive tension, and could have been prevented by
extending the flap ventrally instead of caudally. The end result was satisfactory.
RESUME.
Les lésions causées par la haute tension peuvent provoquer des défauts ŕ toute
epaisseur de la paroi abdominale difficiles ŕ reconstruire.'L'Auteur décrit un cas de
reconstruction périombilicale avec l'emploi d'un lambeau myocutané du tensor fasciae
latae (TFL), dans un enfant âgé de 8 ans qui avait subi de graves brűlures
électriques. L'Auteut décrit la procédure chirurgicale, effectuée avec l'emploi d'un
lambeau droit en îlot myocutané du TFL. Le traitement a donné des résultats
satisfaisants.
BIBLIOGRAPHY
Shaw
W.W., Aston SJ., Zide B.M.: Reconstruction of the trunk. In: McCarthy J.G., "Plastic
Surgery", W.B. Saunders Company, Philadelphia, vol. 6, 3763-74, 1990.
Bogart J.N., Rowe D.S., Parsons R.W.: Immediate abdominal
wall reconstruction with bilateral groin flaps after resection of a large desmoid tumor.
Plast. Reconstr. Surg., 58: 716-9, 1976.
Little J.W., Fontan D.J., McCullough D.T.: The
upper-quadrant flap. Plast. Reconstr. Surg., 68: 175-80, 1981.
Farr R.E.: Closure of large hernial defect in the upper
abdomen. Surg. Gynecol. Obstet., 34: 264-7, 1922.
Wangensteen O.H.: Large
defects of the abdominal wall employing the iliotibial tract of fascia lata as a pedicled
flap. Surg. Gynecol. Obstet., 59: 766-9, 1934.
Wangensteen O.H.: Repair of large abdominal defects by
pedicled fascial flaps. Surg. Gynecol. Obstet., 82: 144-50, 1946.
Watson J.S.: Reconstruction
of the anterior abdominal wall above the umbilicus using a tensor fasciae latae
myocutaneous island flap. Br. J. Plast. Surg., 36: 334-6, 1983.
Hershey F.B., Butcher H.P.: Repair of defects after partial
resection of the abdominal wall. Am. J. Surg., 107: 586-91, 1964.
Boswick J., Nahai F., Wallace J.G., Vasconez L.O.: Sixty
latissimus dorsi flaps. Plast. Reconstr. Surg., 63: 31-6, 1979.
Houston G.C., Drew G.S., Vasquez B., Given K.S.: The
extended latissimus dorsi flap in repair of anterior abdominal wall
defects. Plast. Reconstr. Surg., 81: 917-20, 1988.
Brown R.G., Vasconez L.O., Jurkiewicz M.: Transverse
abdominal flaps and the deep epigastric arcade. Plast. Reconsur. Surg., 55: 41620, 1975.
Mathes S.J., Boswick J.: A rectus abdominis myocutaneous
flap in repair of anterior abdominal wall defects. Br. J. Plast. Surg., 30: 282-9, 1977.
Taylor G.I., Corlett R.I.,
Boyd J.B.: The extended deep inferior epigastric flap. A clinical technique. Plast.
Reconstr. Surg., 72: 75 1 - 61, 1983.
Taylor G.I., Corlett R.J.,
Boyd J.B.: The versatile deep inferior epigastric (inferior rectus abdorninis) flap. Br.
J. Plast. Surg., 37: 330-50, 1984.
Cormack G.C., Quaba A.A.:
Bilobe modification of the deep inferior epigastric artery flap for abdominal wall defect
reconstruction. Br. J. Plast. Surg. 44: 541-3, 1991.
This paper was received on
3 November 1999.
Address correspondence to:
Pedro C. Cavadas, M.D., Ph.D.
Paseo Facultades I C-10
46021 Valencia, Spain. |
G. WHITAKER
INTERNATIONAL BURNS PRIZE
PALERMO, ITALY
Under the patronage of the Authorities of the Sicilian Region for 2000
By law n. 57 of June 14th
1983 the Sicilian Regional Assembly authorized the President of the Region to grant the
Giuseppe Whitaker Foundation, a non-profit-making organization under the patronage of the
Accademia dei Lincei with seat in Palermo, an annual contribution for the establishment of
the G. Whitaker International Burns Prize aimed at recognizing the activity of the most
qualified experts from all countries in the field of burns pathology and treatment.
The amount of the prize is fixed at twenty million Italian Lire. The prize will be awarded
every year by the month of June in Palermo at the seat of the G. Whitaker Foundation.
The Adjudicating Committee is composed of the President of the Foundation, the President
of the Sicilian Region, the Representative of the Accademia dei Lincei within the G.
Whitaker Foundation, the Dean of the Faculty of Medicine and Surgery of Palermo
University, the President of the Italian Society of Plastic Surgery, three experts in the
field of prevention, pathology, therapy and functional recovery of burns, the winner of
the prize awarded in the previous year, and a legal expert nominated in agreeement with
the President of the Region as a guarantee of the respect for the scientific purpose which
the legislators intended to achieve when establishing the prize.
Anyone who considers himself/herself to be qualified to compete for the award may send by
January 31st 2000 a detailed curriculum vitae to: Michele Masellis M.D., Secretary-Member
of the Scientific Committee G. Whitaker Foundation, Via Dante 167, 90141 Palermo, Italy. |
|



