Annals of
Burns and Fire Disasters - vol. XIII - n° 1 - March 2000
EFFECT OF ASPIRIN ON INTERMEDIATE BURN
SURVIVAL IN RATS
Shalom k Westreich M.
Department of Plastic Surgery, Assaf
Harofeh Medical Centre,
Tel-Aviv University, Sackler School of Medicine, Zerifin, Israel
SUMMARY. Aspirin
does not improve intermediate burn zone survival. It is possible that the active
metabolites of cyclo-oxygenase are not important in intermediate burn zone survival, but
other possibilities exist. It may be that administration post-burn does not reverse the
noxious tissue events that cause cell death, or that aspirin must be given for a longer
period of time. This suggests that aspirin is probably not beneficial in the clinical
setting for the improvement of burn wound survival and healing.
Introduction
Thermal burn injuries are
a major health care problem and any therapeutic mode that can decrease inherent morbidity
and mortality would benefit burn patients and society in general. The aim of all burn
treatment regimens is to increase survival of the intermediate burn zone, thus decreasing
morbidity, mortality, and the need for operations and hospitalization.
Complex local and systemic events are responsible for intermediate zone viability. Among
these are inflammation, ischaernia, coagulation, and oxygen free radical (OFR) formation.
These pathophysiological changes are similar to those seen in the ischaernic skin flap.
Aspirin, with its ability to neutralize the enzyme cyclo-oxygenase, has been shown to be
effective in increasing ischaemic flap survival and burn wound perfusion.` Because of the
similarities between unsuccessful flaps and intermediate zone burns, we conducted a study
to evaluate if aspirin, which increases the survival of ischaemic flaps, could also
increase intermediate zone burn survival.
Material and method
Twenty male Sprague-Dawley
rats (average weight 250 ± 20 9) were randomly divided into two experimental groups:
- aspirin treatment group (N° 10)
- control group (N° 10)
Each rat was anaesthetized
using an intraperitoneal injection of pentobarbital (40 mg/kg). The back of each rat was
shaved, and a brass comb measuring 20 x 20 x 55 min was used to inflict the bums. The comb
had four rectangular contact sectors (10 x 20 trim) cut at 5 mm intervals (Fig. 1).
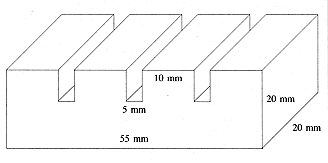 |
Fig. 1
- Brass comb with four contact sectors of 10 x 20 min set at intervals of 5 min. |
|
The comb
was equilibrated in boiling water, briefly blotted, and then placed for 30 see without
pressure on one side of the rat's back. After re-equilibration of the brass comb in
boiling water, a second identical comb burn was made on the other side. This created a
standard injury with four areas of full-thickness bum, corresponding to the four teeth of
the brass comb. Each area measured 10 x 20 mmi, and created intermediate burns' between
and around the full-thickness burn zones, the area studied in the experiment.
To simulate clinical use of the drug (i.e. post-injury), the aspirin treatment group
received intramuscular injections of 200 mg/kg of aspirin immediately after burn
infliction and 24 and 48 h later. The control group received sham injections of saline.
The total burn area was evaluated on days 1, 3, and 7 using fluorescein fluorescence (15
mg/kg). The area of the burn was copied onto a clear plastic sheet. Burn areas were
determined by cutting out the marked area of the burn and then weighing the cut-outs on an
analytical scale.
The Student t test was used to determine if there was a statistical difference between the
groups.
Results
No statistical difference
was observed between the test and control groups.
Discussion
Bums of human skin can be
divided into three distinct zones:
- coagulative zone - immediate tissue
necrosis due to the thermal injury
- intermediate zone - damaged tissue, with no
potential for survival
- erythematous zone - minor degree of thermal
injury that nearly always heals uneventfully
Since the area of burn
coagulation will invariably slough, burn treatment protocols aim at increasing survival of
the intermediate burn area. Complex events effect the viability of the intermediate burn
zone. These include inflammation, ischaernia, coagulation, and OFR formation. These
changes are commonly seen in unsuccessful cutaneous flaps. It seemed to us logical that
any therapeutic mode that could increase ischaemic flap survival would be of benefit also
to the intermediate burn zone.
The pathophysiological reactions determining random pattern flap survival, which are
similar to those seen in intermediate burn area survival, include:
- decrease in perfusion and ischaemia
- specific and nonspecific inflammatory
reaction
- OFR formation
Ischaemia - Tissue
ischaemia is a combination of systemic and local reactions. The systemic reaction causes
an increase in vascular permeability. This "third spacing" decreases effective
vascular volume and decreases perfusion. Systemic cardiac depressant factors could further
decrease cardiac output, thus decreasing perfusion of nonvital organs such as the skin.
Local reactions such as vasoconstriction, coagulation (due to low flow and tissue damage),
oedema (due to increased local vascular permeability), and vascular plugging (due to
inflammatory infiltrate) could accentuate local ischaemia.
Inflammatory reaction - The extensive damage caused by the burn stimulates the
immune system, with potentially devastating effects. Polymorphonuelears (PMN) and
macrophages could damage potentially viable tissue by OFR formation. The inflammatory
infiltrate could cause the plugging of blood vessels, causing ischaemia. Other cytokines
and echisonoid products such as thrombaxane A2 and prostaglandin F2a could
stimulate vasoconstriction and coagulation and further increase ischaemia.
OFR formation - OFRs have the ability to peroxidize cell membranes, inactivate
enzymes containing sulphydryl groups, depolymerize carbohydrates, and hydroxylate nucleic
acids.
All these reactions alone or in combination can cause cell death.
Aspirin is one of the most widely used drugs today, as an antipyretic, anti-inflammatory
and analgesic. Its anti-aggregation effect has made it an effective prophylactic drug
against atherosclerotic heart disease and cerebrovascular accident. Aspirin is an
irreversible inhibitor of the enzyme cyclo-oxygenase, which is the key enzyme in the
metabolism of arachidonic acid and its products: thrombaxane, the leukotrienes, and the
prostaglandins.
In a previous work we showed that aspirin at this high dose had a beneficial effect on
failing random pattern flaps in rats.
Aspirin has a theoretical potential to improve intermediate burn zone survival by its
ability to:
- modulate the inflammatory reaction by
decreasing the formation of thrombaxane A2, leukotriene C, and prostaglandins
by permanently blocking the enzyme cyclo-oxygenase in arachidonic acid metabolism
- increase perfusion by a direct relaxing
effect on vascular smooth muscle
- decrease reperfusion injury by increasing
initial perfusion
- reduce OFR formation by decreasing the
inflammatory reaction and a direct effect on PMNs
- release adrenocorticosteroids via an
indirect effect on the hypothalamus
- stabilize the endothelial leak
Robson showed that a dose
of 325 mg/kg aspirin can increase burn wound perfusion when given pre-bum. Although burn
viability studies using this drug have never been performed, the increased perfusion
should be reflected in increased survival of the intermediate burn area, Aspirin at the
dose used in our experimental animals (200 mg/kg) would obviously not be suitable for
clinical application, but if aspirin did benefit burn survival, other safer drugs with
similar properties could be used.
In this study, with aspirin given post-burn as in a clinical situation, the drug failed to
improve intermediate burn area survival. The reasons for this could be:
- the timing of administration - post-burn
administration of aspirin may not have the ability to reverse the noxious inflammatory,
thrombotic, and systemic effects of the burn
- dosage - the drug may not achieve effective
levels at the burn site owing to haernodynarnic compromise or local tissue events
- the length of time when the medication was
administered was shorter than that required
- other major factors affecting intermediate
burn survival that are not affected by aspirin
RESUME. L'aspirine
n'est pas capable d'améliorer la survie de la zone intermédiaire des brűlures. La
raison pourrait ętre que les métabolites actifs de la cyclo-oxygénase ne sont pas
importants pour la survie de la zone intermédiaire des brűlures, mais d'autres
possibilités existent. Il est possible que l'administration aprčs la brűlure n'est pas
capable d'inverser les évčnements nuisibles pour les tissus qui causent la mort
cellulaire, ou bien que l'aspirine doit ętre administrée pour une période de temps plus
longue. Cela indiquerait que l'aspirine probablement ne serait pas utile dans les cas
cliniques pour améliorer la survie des patients brűlés et pour leur guérison.
BIBLIOGRAPHY
Shalom A., Westreich M.: Effect of aspirin
on flap survival. European J. Plastic Surgery. Presented at 66th Annual Scientific Meeting
ASPRS.PSEF.ASMS, September 1997, San Francisco, USA (in press).
Shalom A., Westreich M.: Effect of
high-dose and low-dose aspirin in random flap survival in rats. Presented at 66th Annual
Scientific Meeting ASPRS.PSEF.ASMS, September 1997, San Francisco, USA.
Robson M.C., De Beccarc, E.J., Heggers
E.J., Loy G.L.: Increasing dermal perfusion after burning by decreasing thromboxane
production. J. Trauma, 20: 722-5, 1980.
Choi M., Rabb H., Amaout A., Ehrlich H.P.:
Preventing the infiltration of leukocytes by monoclonal antibody blocks the development of
progressive ischaerma in rat bums. PRS, 96: 117785, 1995.
Goodman & Gilman: The pharmacological
basis of therapeutics. In: Goodman, Gilman A., Rall T.W., Niews A.S., Taylor P. (eds), 8th
edition, Pergamon Press, 625-63, 1996.
Lewis H.D., jr, Davis JW., Archibald D.G.
et al.: Protective effects of aspirin against acute myocardial and death in men with
unstable angina: results of a Veterans Administration Co-operative Study. N. Engl. J.
Med., 309: 396-403, 1983.
Report of the WHO Task Force on Stroke and
Other Cerebrovascular Disorders. Stroke 1989: Recommendations on stroke prevention,
diagnosis, and therapy. Stroke, 20: 107-11, 1989.
Al-Mondhiry H., Marcus A.J., Spaet T.H.: On
the mechanism of platelet function inhibition by acetylsalicylic acid. Proc. Soc. Exp.
Biol. Med., 133: 632-6, 1970.
This paper was received on
16 October 1999.
Address correspondence to:
Dr Avshalom Shalom
Department of Plastic Surgery, Assaf Harofeh Medical Centre
Tel-Aviv University, Sackler School of Medicine
Zerifin, 70300 Israel. |
|
