Annals of Burns and Fire Disasters - vol. XIII -n. 2 - June 2000 MORTALITY OF THE PAEDIATRIC BURN POPULATION TREATED AT THE VIRGEN DEL ROCIO UNIVERSITY HOSPITAL, SEVILLE, SPAIN IN THE PERIOD 1968-1999Gornez-Cěa T., Franco A., Mallén J.M., Gimeno M.A., Ferndndez-Mota A., Mŕrquez T., Portela C., Lňpez I. Plastic and Reconstructive Service, Burn Unit, Virgen del Rocěo University Hospital, Seville, Spain SUMMARY. Changes in medical treatment protocols have led to a significant reduction in the mortality of the paediatric population treated at the Burn Unit of the Virgen del Rocfo University Hospital in Seville (Spain) in the last 30 yr. An analysis was made of the probability of death in two groups of patients under 9 yr with burns in:5 45 % body surface area: Group A (1451 admissions between 1968 and 1977) and Group B (312 patients admitted between January 1993 and January 1999). In Group A, approximately one-hundredth of the patients admitted with the above characteristics died, while in Group B the mortality rate was one in three hundred. The findings in these two groups of patients during the two periods are compatible with those published by other authors. Some changes in the clinical protocols might explain the improvements achieved, e.g., resuscitation therapy adapted to each individual case, with early use of colloids; strict hypercaloric and hyperproteic nutrition; early escharectomy and subsequent closing of the wound. Introduction Burns in the paediatric population are frequent. According to the Center for Disease Control in Atlanta, USA, every year more than 1000 children under 15 yr of age die in the United States in domestic fires, equivalent to almost two-thirds of deaths in children under 4 yr of age. Approximately 20% of the patients admitted to the Burn Units in our country are under 9 yr of age. In other regions, with a lower social and economic development, this phenomenon is even more frequent since the birth rate is much higher than in our country, the mean age of the population is lower, and the probability of suffering a burns accident burns increases exponentially in relation to inadequate or poorly applied fire prevention regulations. Certain specific characteristics of children make their response to a thermal accident different from that of an adult. The body proportions differ. Blood volume, for example, after adjustment for body weight, is greater in children. The loss of body fluids through the burned area isproportionally greater in the young, owing to the difference between weight and body surface, with respect to age. These and other circumstances have led many researchers to recommend that the fonnulae for fluid restoration during the shock phase should be adjusted to the paediatric patient's body surface, or that human seroalbuntin should be added early to resuscitation fluids. According to Wolf et al., lower age, larger burn size, the presence of inhalation injury, delayed intravenous access, sepsis, inotropic requirements, and ventilator dependency during the hospital course are significant predictors - among other variables - of increased mortality. The high incidence of infantile burns and the severity of sequelae in the child's subsequent development have drawn special attention to this risk group in our Burn Unit, since its inauguration in 1968. The aim of this paper is to analyse the effects that advances in burn patient treatment have had in the increased probability of survival of our paediatric patients. Material and metods The data
regarding children under 9 yr of age admitted to the Burn Unit of the Virgen del Rocěo
University Hospital, Seville, Spain between July 1968 and December 1976 (8.5 yr) (Group A)
were compared with those of children admitted between January 1993 and January 1999 (6 yr)
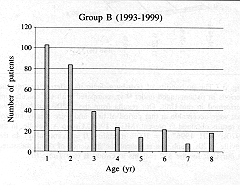
(Group B). The population served by our Burn Unit has been practically constant since its inauguration (about 7,000,000 persons) but an important reduction has been observed in the incidence of annual hospitalizations: from 175 children per yr in Group A to 50 children per yr in Group B. This could be related to the prevention campaigns that have been conducted. The burned BSA in patients in Group A ranged from I to 90%. All the patients in Group B had burns in 45% BSA (Fig. 1). In Group A, 1451 children had burns in 45% BSA, with a greater extent in 24 patients. For the sake of adequate comparison, these patients were excluded from the analysis
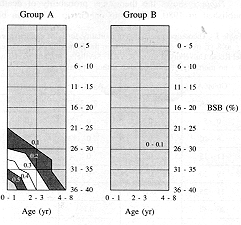
In Group A, 32 patients died during hospitalization in the Unit, fourteen of whom with burns in 45% BSA, an approximate ratio of one per hundred. Only one patient in Group B died out of the 312 patients hospitalized. This was a one-year-old boy hospitalized after a scald affecting 15% BSA in the face, neck, chest, and abdomen and requiring mechanical ventilation because of laryngeal stridor less than 12 h after admission. The child died 45 days after the accident, in the paediatric ICU of our hospital, where he had been put on mechanical ventilation to treat a distress respiratory syndrome. The cause of death was multi-system organ failure. At the moment of death the epithelialization of the burns was almost complete. Table I shows the theoretical probability of death, published in 1980, of patients in Group A. It can be observed that the probability of death was greater for younger children with more extensive burns.
Table
II shows the incidence of death observed in the 312 children in Group B. The probability
of death decreased significantly in our Unit from one out of every hundred children in
Group A to one out of every three hundred children in Group B.
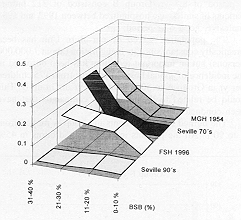
Table
III and Fig. 3 express the probability of death after burns in different centres and
periods for patients aged less than 9 yr. Our probabilities of death, adjusted for age and
burn extent in the 1970s, were similar to those published by Bull and Fishr and
significantly lower than present-day probabilities. Discussion As long ago as 1980 we stated that the treatment of burn patients had made important progress in our country because such treatment was now being given in the specially designed centres to which patients were normally referred. There were, however, certain problems: children with burns frequently arrived late at the Unit, having been sent on from other medical or surgical units that were not specialized in burns management and having received inadequate therapy. Problems were thus encountered in relation to the primary attendance and evacuation of the critically ill burn patient. These problems have now been solved by the creation in our country of a National Healthcare Service that co-ordinates specialized care and of Emergency Healthcare services that facilitate a more satisfactory emergency treatment at the location of accidents as well as the evacuation of patients with multiple trauma, in particular those suffering from burns. Mortality related to burn injuries in Spain is thus improving.Medical care protocols for burn patients, particularly in relation to the paediatric population, have also shown an outstanding improvement since the creation of this Unit in 1968. Essentially, the difference lies in the more active treatment of the patients with the intention of preventing complications and treating them early as soon as they occur: resuscitation adapted to the individual necessities of each patient, early hypercaloric and hyperproteic nutrition, excision of the burn wound, immediate temporary or definitive closure, correct application of medication, the use of a burn unit antimicrobial policy adapted to suit the particular context of the Hospital, etc. It is our logical wish to analyse whether the application of updated protocols for the assistance of burn patients has led to an improvement in our clinical results. Of the many possible methods of conducting such a study, we chose that of comparing the probability of survival, adjusted in relation to age and burn extent, in two different periods in our Burn Unit, which has been open and operative for over 30 yr - since 1968. The option for this type of analysis was partially motivated by the fact that the publication of Franco et al. in 1980 was the only study, among those performed in our Unit, that was old enough - with a 20-yr difference - to permit a reliable comparative analysis with recent data. No other similar studies exist that were, performed with other groups of patients treated at this Unit. The percentage of burned BSA and age are determinant factors in burn severity, and these two parameters are therefore frequently considered in the prognosis of patients admitted to burn units. It has also been demonstrated that besides age and burned BSA there are other decisive risk factors regarding burn severity. However, predictions based on age and the percentage of burned BSA alone have sufficient specificity to fulfil clinical and scientific goals, although the low sensitivity decreases the precision of the prediction at the moment of hospitalization if additional factors are not considered. We therefore decided that the survival curves of the paediatric population attending our Unit, in the two periods during which the care protocols were clearly different,could be used to evaluate the effectiveness of the medical treatment given. We selected the paediatric population as being a representative sample because of the high proportion of hospitalizations in relation to the total number of admissions to our Centre, and to the existence of an extensive historical control group. Unfortunately, no comparable study has been performed using the total number of patients, both paediatric and adult, seen in our Unit during the period of time in question. The present results, at least in our view, would appear to confirm the improvement in the clinical care provided in our Unit for burned paediatric patients since its creation 30 yr ago. However, these results alone do not confirm the validity, of our clinical activity and we therefore compared our results with those published by other researchers. We selected a classic reference published in 1954 by Bull and Fisher and - as a representation of burn units with currently confirmed results - findings from the Burn Unit of the United States Army Institute of Surgical Research, among the many possible units. It is evident, when comparing data of the early 1950s with those of the early 1990s, that the improvement in the clinical protocols of the burn patient care has significantly increased postburn survival, including that of paediatric patients (Fig. 3). An in-depth statistical analysis has not been possible because of the lack of comparable data between the groups analysed. We conclude that the application of updated clinical protocols to the treatment of burned children permits the achievement of results that can be homologized, with a significant decrease of mortality in our Unit compared with historical data over the thirty years studied. In our opinion, mortality curves related to age and percentage burned BSA are a simple and effective tool for the comparison of clinical results from different burn units, as long as the population analysed is as large and as homogeneous as possible. The time-course of this type of curve can be useful for the assessment of the clinical efficacy of a particular burn unit and the impact that changes in strategy have on the final outcome.
RESUME. Les modifications des protocoles du traitement médical ont porté a une réduction significative de la mortalité de la population pédiatrique traitée dans l'Unité des Brűlures de l'Hôpital Universitaire Virgen del Rocěo A Séville (Espagne) pendant les derniers 30 ans. Les Auteurs analysent la probabilité de la mort dans deux groupes de patients âgés de moins de 9 ans atteints de brűlures dans Ł 45% de la surface corporelle. Le groupe A était composd de 1451 enfants hospitalis6s entre janvier 1968 et 1977 et le groupe B de 312 enfants hospitalisés entre janvier 1993 et janvier 1999. Dans le groupe A, approximativement un patient sur 100 atteints de brűlures de l'extension en question est mort, tandis que le taux de mortalité dans le groupe B était un sur 300. Les résultats des Auteurs pendant les deux périodes analysées sont compatibles avec les résultats publiés par d'autres Auteurs.Certaines modifications dans les protocoles cliniques pourraient etrę responsables des améliorations, c'est-a-dire une thérapie réanimatoire adaptée selon les cas, avec l'emploi précoce de colloďdes, une nutrition stricte hypercalorique et hyperprotéique,l'escharectomie précoce, et la fermeture de la lésion. BIBLIOGRAPHY
|