Annals of
Burns and Fire Disasters - vol. XIII - n. 3 - September 2000
THE METHOD OF
MICROGRAFTING IN THE TREATMENT OF LARGE AREA FULL-THICKNESS BURNS
Hadjiiski O.
Burns and Plastic Surgery Centre,
Pirogov Emergency Medical Institute, Sofia, Bulgaria
SUMMARY. A method is proposed for the treatment of large
area full-thickness burns (over 40% total body surface area). The preparation of small
grafts, called microstamps, is described together with the method of their application to
the wound surfaces. The various advantages of the method are defined: use of a small area
autograft (some sq. cm), possibility of a large coefficient of distribution up to 1:9,
possibility of combination with other methods, use of small donor sites from which it is
not possible to take full skin grafts, and good final results.
Introduction
A basic method in the
operative treatment of large bums is the use of small skin amografts to cover large wound
areas. This is performed using various methods of enlargement of the graft area. A number
of methods have been elaborated for the perforation and enlargement of such grafts. In
1968 Hermans was the first to try to cover a wound with a skin graft of smaller area than
the wound. The aim was to cover as much as possible of the wound area (depending on the
coefficient of perforation) with skin grafts that were as small as possible. The method
became increasingly popular over the years. Various devices are used for perforation of
the skin autografts - Tanner dermatome, Zimmer dermatome, Bioplast dermatome,perforation
of the donor site, and modified and handmade devices.
In 1958 Meek presented the Humeca dermatome for the preparation of small skin autografts
of several sq. cm, a technique he called "micrografting". Kreis and Vloemans
developed the method clinically at the Red Cross Hospital, Beverwijk, Holland. Today
micrografting is used in various centres all over Europe. In Bulgaria the method has been
adopted only at the SIEM Pirogov Centre. We apply the method in burns of more than 40%
TBSA.
Working experience
We cut the skin autografts
using a special Humeca dermatome which ensures that the stamps are of equal size and that
the distance between them is accurately defined. The skin grafts are cut in pieces
measuring 4.2 x 4.2 sq. cm and placed on a special cork base. A separate small part can
also be added on top of this until the whole area of the cork base is filled. An electric
mechanism with 13 knives is used to cut the graft; the distance between the cuts is 3 mm.
After the first insertion of the graft under the knives it is rotated 90° and inserted
under them again.
Small marks of 3 x 3 mm are thus made. After cutting, the micromarks are sprayed with a
special glue (Leucospray) and glued to a gauze. Depending on the indications we use a
distribution coefficient of 1:4, 1:6, or 1:9. After adhesion of the marks to the gauze,
the gauze, which is crimped, is extended on all sides, and the extension previously set by
the gauze net is achieved. We place the previously prepared micromarks on the wound
surface. The aluminium foil is removed from the back of the gauze and the wound is dressed
as usual.
After five days the dressings are removed and the gauze is spread over with silver
sulphadiazine. The day after the gauze is soft, it is removed from the wound surface. The
grafts are cleaned and future steps are considered. In patients subjected to early
surgical necrectomy, the wound surface and the grafts are covered with a skin allograft
perforated 1:1.5 (sandwich method). Epithelialization of the marks begins under the skin
allograft. The dressings are changed in two or three days. If the marks are put over a
granulating wound surface they can be covered with a skin allo- or xenograft. If there is
a lack of such grafts the wound can be covered with ointment dressings. These are
exchanged every other day. As in the Chinese marks method (which we also use),
epithelialization begins from the mark edge up to full epithelialization of the wound.
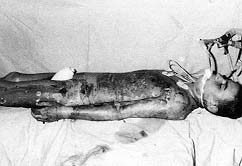
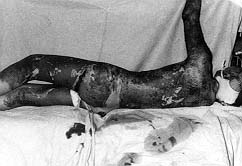
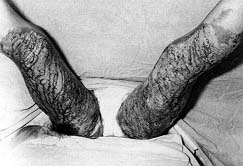
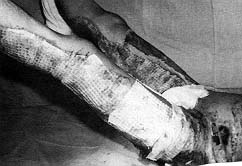
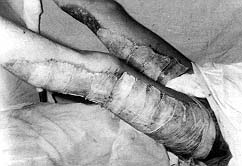
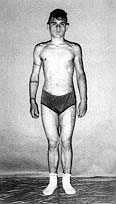
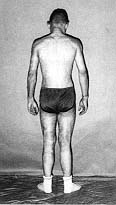
The figures below illustrate the case of 16-yr-old patient surgically treated using this
method. The patient was burned in 65% TBSA in the back, chest, arms, and legs. He was in
thermal shock and had inhaled smoke. The agent was flame. The patient was transferred to
our centre 14 h after the accident. On days 3, 5, and 7 we performed early surgical
excision of necrotic tissue in the legs, chest, and belly in 32% TBSA, leaving 14%
disseminated necrotic tissues. The wound surfaces were covered with micrografts in five
surgical steps every third to fifth day. The total donor site area was 14%. The donor
sites were large because of the need to change some of the marks in subsequent surgical
stages. During treatment the patient developed generalized bacterial infection, which was
appropriately treated. On day 79 he was discharged in good health (Figs. 1-8). The area of
the skin autografts performed in this patient was less than 2% TBSA and the blood loss
from the donor sites was no more than 300-400 ml. In the third operation on a separate
site we left the gauze until day 7-9. We do this only when the grafting is good and there
is no local infection or exudation. After removing the gauze we observe initial
epithelialization between the marks. It is important to bear in mind that in certain
conditions removal of the gauze can be postponed until later than the time normally
proposed. The advantage of this is that the sterile milieu is left undisturbed, some of
the marks remain stable, and the allograft is not necessarily used to cover the wound
surfaces.
Discussion
In extensive burns
covering more than 30% T13SA, whole autografts can be used only in 18% of surgically
treated patients and donor sites are limited.' If donor sites are used, the treatment
continues for several months, with numerous operations - a period during which the patient
may develop a severe catabolic syndrome, organ insufficiency, and generalized infection,
which can be fatal. The micromark method is a development and an improvement in the
methodology of the treatment of extensive burns, thanks to a different combination of
small autografts. Shvets8 and Kreis9 recommend the method for the treatment of burns in
45-75% TBSA and indicate a perforation of the graft over 1:4. Kreis2 observed over 90%
healing of the marks in 16 patients with extensive burns. On day 6 post-surgery Zermani
observed 93% healing in micromarks and 80% in perforated mesh autografts. We use the
method in burns of over 40% TBSA." We followed the Chinese method until 1996 but our
manual preparation of the application of the marks was not sufficiently accurate."
With the micromark method, the distribution achieved corresponds exactly to that planned,
whereas with the mesh graft technique the coefficient is smaller (20-45%), depending on
the kind of perforation .Z~"'3 The method can be used together with other mesh graft
techniques. The microtechnique combined with allograft ensures better results, especially
if removal of the necrotic tissues is performed early. This technique obviates the
application of tissue cultures.
We believe, like many other researchers, that the micromark method presents the following
advantages:
Conclusion
The Meek micrografting
method is suitable in the treatment of burns in over 40% TBSA. Its application saves the
lives of patients in whom other operative methods do not have positive results. The method
is recommended when for various reasons other methods are impossible (tissue cultures).
The late results of the micromark method are good.
RESUME. L'Auteur
présente une méthode pour le traitement de brűlures de grande étendue (> 40% de la
surface corporelle). Il décrit la préparation de ce qu'il définit les microtimbres,
comme aussi la méthode d'application sur les brűlures. Cette méthode offre une série
d'avantages: l'emploi d'autogreffes de dimensions limitées (quelques cm2),
possibilité d'un coefficient de distribution élevé jusqu'ŕ 1:9, possibilité
d'association ŕ d'autres méthodes, emploi de sites donneurs que l'on ne peut pas
utiliser pour des greffes cutanées ŕ toute épaisseur, et bons résultats finals du
traitement.
BIBLIOGRAPHY
Kreis R., Hoekstra M.J.,
Mackie D.P. Vloemans A.F.P.M., Hermans R.P.: Historical appraisal of the use of skin
allografts in the treatment of extensive full-skin thickness burns at the Red Cross
Hospital Burns Centre, Beverwijk, The Netherlands. Burns, 18 (Suppl. 2): S19-S22, 1992.
Kreis R., Mackie D.P., Hermans R.P.:
Expansion technique for skin grafts: Comparison between mesh and Meek island/sandwich
grafts. Burns, 20: 39-42, 1994.
Echinard Ch., Latarjet J.: "Les
Brűlures", Masson, Paris, Milan,349, 1993.
Verlende P.N., Zoltie N.: How to get large
meshed split-skin grafts.Burns, 15: 55-6, 1989.
Herbert K.: A simple method of preparing
split-thickness skin grafts for meshing. Plast. Reconstr. Surg., 86: 357-8, 1990.
Vartak A.: New economical skin graft
expansion wheel. Burns, 8:157-8, 1992.
Archer S.B., Henke A., Greenhalgh D.G.: The
use of sheet autografts to cover extensive burns in patients. J. Burn Care Rehabil., 19:
33-8, 1998.
Shvets V.N., Malakhov S.F., Egorov B.B. et
al.: Ability of microamotransplants to re-epithelialize deep and extensive skin injuries.
Burns, 17: 243-9, 1991.
Kreis R., Mackie D.P., Vloemans A.F.P.M.,
Hermans R.P.,Hoekstra M.J.: Widely expanded postage stamp skin grafts using a modified
Meek technique in combination with an allograft overlay. Burns, 19: 142-5, 1993.
Zermani R.G., Zarabini A., Trivisonno A.:
Micrografting in the treatment of severely burned patients. Burns, 23: 604-7, 1997.
Hadjiiski O.: Prehospital care and hospital
treatment in patients during mass burns disasters. Ph.D. thesis, Sofia, 1999.
Hadjiiski O.: Chinese method for surgical
treatment in big and deep burns. J. Emergency Medicine, Sofia, 2: 22-24, 1993.
Peeters R., Hubens A.: The mesh skin graft
- true expansion rate. Burns, 14: 239-40, 1988.
Raff T., Hartmann B., Wagner H., Germann
G.: Experience with the modified Meek technique. Acta Chir. Plast., 38: 142-6, 1996.
Fang C.H.,Yu G., Fan Y.F. et al.: A
preliminary report on transplantation of microskin autografts overlaid with sheet
allograft in the treatment of large bums. J. Burn Care Rehabil., 9: 629, 1988.
| This paper was received on
17 January 2000.Address
correspondence to: Prof. Ognian Hadjiiski MD, Bums and Plastic Surgery Centre, Pirogov
Emergency Medical Institute, Blvd. Macedonia 21, 1606 Sofia, Bulgaria. Tel./fax: 359 2
546108; e-mail: burns_hadj@hotmail.com |
|