Annals of
Burns and Fire Disasters - vol. XIII - n. 3 - September 2000
HYPERTROPHIC SCARS
AND KELOIDS: IMMUNOPHENOTYPIC FEATURES AND SILICONE SHEETS TO PREVENT RECURRENCES
Borgognoni L., Martini L., Chiarugi C., Gelli
R., Giannotti V., Reali U.M.
Plastic and Reconstructive Surgery, Santa
Maria Annunziata Hospital, University of Florence Medical School, Florence, Italy
SUMMARY. Hypertrophic scars (HS) and keloids
(K) very often result from bums and sometimes from minor injuries. It has been
hypothesized that immunological mechanisms play a role in the pathogenesis of HS and K.
However, the knowledge of the pathogenesis of these disorders is still incomplete and the
therapeutic strategies limited and often unsatisfactory. In particular, the surgical
excision of the lesion is followed by a high incidence of recurrences, especially in K. In
this study, we performed a preliminary clinical and pathological investigation in 20
selected cases of K occurring after a previous surgical excision. Our aims were to
evaluate the possible advantage of adhesive silicone sheet application after K excision in
order to prevent recurrences and to investigate immunophenotypic modifications in scar
tissue after treatment. Ten K underwent surgical excision and ten K underwent surgical
excision and silicone sheet application for 3 months. For the immunohistochemical analysis
we used the alkaline phosphatase anti-alkaline phosphatase (APAAP) technique and a large
panel of monoclonal antibodies. In the K group with surgical excision and silicone sheet
application we observed a 60% rate of complete remission, whereas only 10% of complete
remission was observed in K treated with surgical excision alone. In the latter group we
observed a high number of total recurrences. No side effects were observed after silicone
sheet application. The immunohistochetriical investigation showed a high amount of
activated immune-cell infiltrate in the excised K, consisting of CD3+, CD4+, CD45R0+,
HLA-DR+, LFA-1+ lymphocytes associated with HLA-DR+ and ICAM-1+ dendritic cells. In K
treated with surgical excision and silicone sheet application we found a clearly lower
amount of the above immune-cell infiltrate and a higher amount of CD36+ dermal dendrocytes
and CD68+ macrophages than in the excised lesion. The results of this study support the
hypothesis that in situ immune mechanisms are involved in the development of pathological
scars. The silicone sheet applications effectively reduced recurrences after K excision
and seem to induce a recovery of the balance of the remodelling processes in scar tissue.
Introduction
Hypertrophic scars (HS)
and keloids (K) are pathological scars which very often develop from burn wounds and cause
important aesthetic and functional problems. However, HS and K may also develop
spontaneously or as the consequence of a minor injury, such as ear piercing, trauma, or
acne.
Despite the numerous histological and biochemical alterations demonstrated in pathological
scars, their pathogenesis is still poorly understood, and a possible role of immunological
mechanisms has been hypothesized on the basis of various experimental evidence. It has
been found that K transplanted in nude mice undergo a rapid decrease in size.
Immunoglobulins G, A, and M are extractable from keloid tissue in significantly greater
amounts than from normal skin and eutrophic scars. Keloid fibroblasts may also be
overstimulated by specific auto-antibodies detected in the lymphocyte eluates of subjects
with K. An anomalous expression of HLA-DR antigen by fibroblasts and keratinocytes and an
increased number of epidermal CD 1 a+ Langerhans cells have also been reported in HS.
Also, in a previous study, we characterized the immunophenotypic features of the cell
infiltrate in HS and K and demonstrated the presence of an immune cell infiltrate that was
much heavier in HS and K than in eutrophic scars. These data support the hypothesis that
in situ immune mechanisms are involved in the pathogenesis of abnormal scars.
Knowledge concerning the pathogenesis of HS and K is still however incomplete and
therapeutic strategies are consequently limited and often unsatisfactory. Compression,
intralesional steroid injections, interferons, hyaluronic acid, lasers, cryotherapy,
radiotherapy, and other treatments have obtained variable results.Surgical excision is
followed by a high percentage of recurrences. At present, a widely used non-invasive
treatment for HS and K is the application of silicone sheets. However, the action
mechanisms of this therapy still have to be clarified.
In order to test the efficacy of silicone sheet application after K excision, we performed
a preliminary clinical and pathological study in 20 selected cases of K that occurred
after previous surgical treatment. Our aims were to evaluate the possible advantage of
silicone sheet application after K excision in order to prevent recurrences and to
investigate immunophenotypic modifications in scar tissue after treatment.
Materials and methods
This study regarded 20 patients with K occurring after a previous
surgical excision. Twelve patients were female (aged 14-53 yr) and eight were male (aged
17-44 yr).�
Ten K underwent a further surgical excision (five K of the ear, three K of the trunk, and
two K of the upper limb) and ten K were treated with surgical excision followed by the
application of an adhesive silicone sheet (Cica-Care, trademark of Smith & Nephew) for
three months (five K of the ear, four K of the trunk, and one K of the upper limb).
Each scar was photographed and measured before excision, at the end of treatment, and
every three months during the follow-up.
We made the following definitions: a) no recurrence - a eutrophic scar consequent to K
excision; b) partial recurrence - a recurring scar of thickness less than 50% of the
excised K; c) total recurrence a K of thickness greater than 50% of the excised K.
All the excised K underwent immune-histological examination.
Ten patients accepted biopsy three months after excision.
Skin samples were divided into two parts and processed by light microscopy and
immunochemistry.
For the histological examination, the specimens were fixed in buffered-formalin liquid for
12-24 h, routinely processed, and embedded in Paraplast Plus with a melting temperature of
+56 �C (Monoject Scientific Inc., Athy, Co. Kildare, Ireland). For each type of lesion, 4
to 6 m-thick sections were stained with haematoxylin and eosin, PASreaction, Masson's
trichrome, and Verhoeff-van Gieson stains.
The immunohistochemical investigation was performed on 6-m-thick cryostat sections
obtained from snapfrozen tissue samples embedded in OCT medium (Miles Laboratories,
Naperville, Il, USA) and stored at -80 �C until sectioned. Multiple serial sections were
cut from each block, airdried for 12-24 h, fixed in acetone for 10 min at room
temperature, airdried again, and stored at -20 �C until immunohistochemical staining. We
used the alkaline phosphatase anti-alkaline phosphatase (APAAP) method and a large panel
of monoclonal antibodies against lymphocytes and their subsets, dendritic cells,
macrophages and their precursors, activation markers, and adhesion molecules (Table 1).
For each section, five microscopic, non-consecutive fields were examined at 250
magnifications. The figures were obtained by counting the number of stained cells
overlying 100 basal cells in the epidermis and per 100 nucleated cells in the dermis.
Monoclonal
antibody |
Cluster of
differentiation |
Specificity |
Leu-14* |
CD22 |
B cells |
T3* |
CD3 |
T-cells |
UCHL-1* |
CD45RO |
T-cell subset |
T4* |
CD4 |
Helper/inducer T-cells |
OKT8* |
CD8 |
Suppressor cytotoxic T-cells |
OKT6* |
CDla |
Langerhans cells,T-zone accessory cells |
HLA-DR* |
- |
Class II molecules |
OKM5� |
CD36 |
Thombospondin
receptor (dermic dendrocytes) |
Anti-CD68* |
CD68 |
Macrophages |
MHM24* |
CDlla |
LFA-1 (a chain) |
OKMl* |
CDllb |
Monocytes, macrophages |
Leu-M5* |
CDllc |
Monocytes, macrophages |
Leu-M3* |
CD14 |
Monocytes |
MHM23* |
CD18 |
LFA-1 ((3 chain) |
CL-106* |
CD54 |
ICAM-1 |
* Dako, Glostrup, DK
� Harlan Sera-Lab Ltd, Belton Loughborough, GB |
Table I
- Monoclonal antibodies used |
|
Statistical analysis was performed using
the Fisher exact test and a p value of < 0.05 was considered statistically significant.
Results
The follow-up of the patients ranged from 6 to 18 months (mean 11.3
� 3.4 months, median 11.5 months for the surgery group; mean 11.6 � 3.5 months, median
12 monthsfor the surgery/silicone group). After treatment, biopsy was accepted by six
patients treated only by surgery (three cases with total recurrence and three cases with
partial recurrence) and four patients treated with surgery and silicone sheet application
(one case with no recurrence and three cases with partial recurrence).
In the group of patients treated only with surgical excision we observed one case with no
recurrence, three with partial recurrence and six with total recurrence.
In the group of patients treated with surgical excision and silicone sheet application we
observed six cases with no recurrence (Figs. 1 ,2), four with partial recurrence, and none
with total recurrence. The adhesive silicone sheets did not require the use of tapes and
they were all well accepted by the patients.
|
|
|
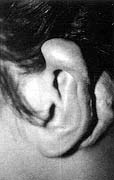
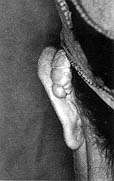
| Fig.
la - Recurrent keloid in helix. |
|
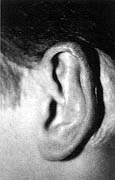
Fig.
lb - No recurrence after surgical excision of the keloid and silicone sheet
application and 15 months' follow-up. |
|
|

|
| Fig.
2a - Recurrent keloid in posterior auricle. |
|
Fig.
2b - No recurrence after surgical excision of keloid and silicone sheet
application and 10 months' follow-up. |
|
| |
No
recurrence |
Partial
recurrence |
Total
recurrence |
Surgery |
1/10 |
3/10 |
6/10 |
Surgery
+
Silicone sheet |
6/10 |
4/10 |
0/10 |
p value |
0.029 |
0.49 |
0.0054 |
Table II
- Clinical results |
|
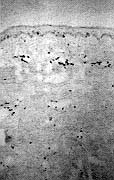
In the group of K treated only with surgical excision, the preliminary immunohistochemical
results showed totally recurring scars with immunophenotypic features similar to those of
the previously excised K described above or to partially recurring scars. These last were
characterized by CD3+, CD4+, CD45R0+, HLA-DR+, and LFA-1+ lymphocytes associated with
HLA-DR+, and ICAM-1+ dendritic cells in a lower amount than in the excised K; the number
of CD36+ dendritic cells and the number of CD68+ macrophages was lower than in the excised
lesions.
In the group of K treated with surgical excision and silicone sheet application we
observed either scars with the typical clinical and pathological features of eutrophic
scars or partially recurred scars. The latter were characterized .by an amount of CD3+,
CD4+, CD45R0+, HLA-DR+, and LFA-1+ lymphocytes associated with HLA-DR+, ICAM-l+ dendritic
cells clearly lower than in the excised K (Fig. 3)
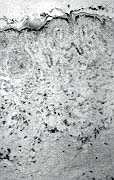
CD36+ dendritic cells were present in higher numbers than in the excised K and uniformly
distributed in the dermis (Fig. 4).
When we compared
partially recurring scars after K excision and three months' application of silicone sheet
with partially recurring scars after surgical excision of K alone, we found a lower amount
of immune-cell infiltrate and a higher number of CD36+ dendritic cells and CD68+
macrophages in the first group of scars than in the second.
Discussion
Treatment of K and HS is difficult and very often unsatisfactory.
The purpose of the present study was to evaluate the possible efficacy of the application
of silicone sheets after K excision in order to reduce recurrences and to characterize the
possible modifications in the scar tissue after treatment.�
Keloids treated with surgical excision and silicone sheet application for three months
showed a higher number of complete remissions (60%) than K treated only with surgery (10%)
(p < 0.05). Also, we did not observe any cases of total recurrence after surgical
excision of K followed by silicone sheet application, even after 18 months follow-up. In
contrast, in the group of K treated
with surgical excision, we observed 60% of cases with total recurrence. These findings are
consistent with data in the literature, which report a 45-100% recurrence after surgical
treatment of K. Compared with other postsurgical treatments to prevent recurrence of K,
silicone sheet application offers the advantage of being a noninvasive therapy. In
contrast, intralesional steroid injections often cause pain and sometimes atrophy,
hypopigmentation, teleangiectasia, and necrosis."'," Patients are often not
compliant with radiotherapy, which is mainly reserved for scars resistant to other
treatment modalities. The silicone sheets used in the present study were well accepted by
the patients, and as they were adhesive they did not require the use of tapes. No side
effects such as erythema, itching, or atrophy were observed.
Another relevant result of this study is the immunophenotypic characterization of the cell
infiltrate in the excised K and in the post-treatment scars. In a previous report, in K we
found an immune-cell infiltrate consisting of CD3+, CD4+, CD45R0+, HLA-DR+, LFA-l+
lymphocytes associated with HLA-DR+, and ICAM-1+ dendritic cells. The over-expression of
functionally meaningful molecules (MHC-Class II, LFA-1, ICAM-1) by distinct subsets of
lymphoid cells supports the hypothesis of an active involvement of the skin immune system
cells in the pathogenesis of K.
After silicone sheet application we observed a eutrophic scar or a partially recurring
scar (less than 50% thicker than previously excised K) characterized by a clearly lower
amount of immune-cell infiltrate than in the initially excised lesion. Also, after
silicone sheet application we found a higher number of CD36+ dermal dendrocytes and a
higher number of CD68+ macrophages, compared with previously excised K. The
immunophenotypic features found in scars after the application of silicone sheets were
more similar to those of eutrophic scars than to those of K.
It could be hypothesized that after the application of silicone sheets there is an
activation of down-regulatory circuits, putatively driven by CD36+ dermal dendrocytes;
with consequent production and discharge of specific cytokines possibly modulating
fibroblast and macrophage activity.
In conclusion, adjuvant silicone sheet treatment after keloid excision was effective in
reducing recurrences. The treatment was safe and no side effects were observed. After
treatment there appears to be a recovery in the balance of scar remodelling processes, as
suggested by the increased number of CD68+ macrophages and CD36+ dermal dendritic cells.
RESUME. Les cicatrices hypertrophiques et les
ch�lo�des sont un r�sultat tr�s commun des br�lures et m�me des l�sions mineures.
Il est possible que les m�canismes immunologiques jouent un r�le dans la pathog�nese
des cicatrices hypertrophiques et des ch�lo�des. Cependant la connaissance de la
pathogen�se de ces maladies est ancore incompl�te et les strat�gies th�rapeutiques
sont limit�es et souvent insuffisantes. En particulier, l'excision chirurgicale de la
l�sion est suivie par une haute fr�quence de r�cidives, particulier�ment dans les
ch�lo�des. Les Auteurs de cette �tude ont effectu� une investigation
clinicopathologique pr�liminaire dans 20 cas s�lectionn�s de ch�lo�des apr�s la
r�cidivation � la suite de l'excision chirurgicale. Le but �tait d'�valuer les
avantages �ventuels de l'application d'une lame adh�sive de silicone apr�s l'excision
des ch�lo�des afin de pr�venir les r�cidives et d'�tudier les modifications
immunoph�notypiques dans le tissu cicatriciel apr�s le traitement. Dix patients ont subi
l'excision chirurgicale et dix l'excision chirurgicale et l'application pour trois mois
d'une lame de silicone. Pour l'analyse immunohistochimique les Auteurs ont utilis� la
technique APAAP et une large s�rie d'anticorps monoclonaux. Dans le groupe des
ch�lo�des trait�es moyennant l'excision chirurgicale et l'application d'une lame de
silicone, les Auteurs ont observ� un taux de 60% de gu�rison compl�te, et un taux de
seulement 10% de gu�rison compl�te dans les cas trait�s seulement avec l'excision
chirurgicale. Ce dernier groupe a pr�sent� aussi un taux �lev� de r�cidivit�.
L'application de la lame de silicone ne pr�sentait aucun effet secondaire.
L'investigation immunohistochimique indiquait une grande quantit� d'infiltrat des
cellules immunes dans les ch�lo�des excis�es, compos� de lymphocytes CD3+, CD4+,
CD5R0+, HLA-DR+, LFA-1+ associ�s � des cellules dendritiques HLA-DR+, ICAM-1+.
Dans les ch�lo�des trait�es moyennant l'excision chirurgicale et l'application
d'une lame de silicone, les Auteurs ont observ� une quantit� nettement inf�rieure de
l'infiltrat des cellules immunes pr�cit�es et une quantit� majeure de dendrocytes
dermales CD36+ et de macrophages CD68+ par rapport aux l�sions excis�es. Les r�sultats
de cette �tude confirment l'hypoth�se que des m�canismes immuns in situ sont impliqu�s
dans de d�veloppement des cicatrices pathologiques. En outre, les applications de la lame
de silicone ont d�montr� la capacit� de r�duire les r�cidives apr�s l'excision des
ch�lo�des et semblent induire le r�tablissement de l'�quilibre des processus de
remodelage dans les tissus cicatriciels.
BIBLIOGRAPHY
- Murray J.C., Sheldon R.P.: Keloids and
excessive dermal scarring. In: "Wound Healing: Biochemical and Clinical
Aspects", Cohen I.K., Diegelmann R.F., Lindblad W.J. (eds), W.B. Saunders Co.,
Philadelphia, 500-9, 1992.
- Datubo-Brown D.D.: Keloids: A review of the
literature. Br. J. Plast. Surg., 43: 70-7, 1990.
- Rockwell BW., Cohen K.I., Ehrlich P.H.:
Keloid and hypertrophic 16. scars: A comprehensive review. Plast. Reconstr. Surg., 84:
827-37, 1989.
- Niessen F.B., Spauwen P.H.M., Schalkwijk
J., Kon M.: On the nature of hypertrophic scars and keloids: A review. Plast. Rec. Surg.,
104: 1435-48, 1999.
- Placik O.J., Lewis V.L.: Immunologic
associations of keloids. Surgery, 175: 185-93, 1992.
- Shetlar M.R., Shetlar C.L., Hendricks L.,
Kischer C.W.: The use of athymic nude mice for the study of human keloids. Proc. Soc. Exp.
19.Biol. Med., 179: 549-52, 1985.
- Kischer CW., Pindur J., Shetlar M.R.,
Shetlar C.L.: Implants of 20. hypertrophic scars and keloids into the nude (athymic)
mouse: Viability and morphology. J. Trauma, 29: 672-7, 1989.
- Cohen I.K., McCoy B.J., Mohanakumar T.,
Diegelmann R.F.: Immunoglobulin, complement, and histocompatibility antigen studies in
keloid patients. Plast. Reconstr. Surg., 63: 689-95, 1979.
- Kischer CW., Shetlar M.R., Shetlar C.L.,
Chvapil M.: Immunoglobulins in hypertrophic scars and keloids. Plast. Reconstr. Surg., 71:
821-5, 1983.
- De Limpens J., Cormane R.H.: Keloids and
hypertrophic scars: Immunological aspects. Aesthetic Plast. Surg., 6: 149-52, 1982.
- Castagnoli C., Stella M., Magliacani G.,
Teich Alasia S., Richiardi P.: Anomalous expression of HLA class II molecules on
keratinocytes and fibroblasts in hypertrophic scars consequent to thermal injury. Clin.
Exp. Immunol, 82: 350-4, 1990.
- Cracco C., Stella M., Teich Alasia S.,
Filogamo G.: Comparative study of Langerhans cells in normal and pathological human scars.
II. Hypertrophic scars. Eur. J. Histochem., 36: 53-65, 1992.
- Borgognoni L., Pimpinelli N., Martini L.,
Brandani P., Reali U.M.: Immunohistologic features of normal and pathologic scars:
Possible clues to the pathogenesis. Ent. J. Dermatol., 5: 407-12, 1995.
- Linares H.A., Larson D.L., Galstaun B.A.:
Historical notes on the use of pressure in the treatment of hypertrophic scars and
keloids. Burns, 19: 17-23, 1993.
- Ward R.S.: Pressure therapy for the control
of hypernophic scar formation after burn injury: A history and review. J. Burn Care
Rehabil., 12: 257-62, 1991.
- Tang Y.W.: Intra- and post-operative
steroid injections for keloids and hypernophic scars. Br. J. Plast. Surg., 45: 371-6,
1992.
- K�l J.: Keloids treated with topical
injections of triamcinolone acetonide (kenalog): Immediate and long-term results. Scand.
J. Plast. Surg., 11: 169-3, 1977.
- Pittet B., Rubbia-Brandt L., Desmouliere A.
et al.: Effect of gammainterferon on the clinical and biologic evolution of hypernophic
scars and Dupuytren's disease: An open pilot study. Plast. Rec. Surg., 93, 1224-35, 1994.
- Borgognoni L., Reali U.M.: Intralesional
hyaluronic acid treatment of pathological scars. Ann. Plast. Surg., 38: 308-9, 1997.
- Alster T.S.: Laser treatment of
hypertrophic scars, keloids and striae. Dermatol. Clin., 3: 419-20, 1997.
- Zouboulis C.C., Blume U., Buttner P.,
Orfanos C.E.: Outcomes of cryosurgery in keloids and hypertrophic scars: A prospective
consecutive trial of case series. Arch. Dermatol., 9: 1146-50, 1993.
- Kovalic J.J., Perez C.A.: Radiation therapy
following keloidectomy: A 20-year experience. Int. J. Radiat. Oncol. Biol. Phys., 17:
77-83, 1989.
- Nicolai J.P., Bos M.Y., Bronkhorst F.B.,
Smale C.E.: A protocol for the treatment of hypernophic scars and keloids. Aesthetic
Plast. Surg., 11: 29-35, 1987.
- Lawrence W.T.: In search of the optimal
treatment of keloids: Report of a series and a review of the literature. Ann. Plast.
Surg., 27: 164-9, 1991.
- Cosman B., Wolff M.: Correlation of keloid
recurrence with completeness of local excision. A negative report. Plast. Reconstr. Surg.,
50: 163-8, 1972.
- Berman B., Bieley H.C.: Adjunct therapies
to surgical management of keloids. Dermatol. Surg., 22: 126-32, 1996.
- Chang C.C., Kuo Y.F., Chin H.C., Lee J.L.,
Wong T.W., Jee S.H.: 32. Hydration, not silicone, modulates the effects of keratinocytes
on fibroblasts. J. Surg. Res., 59: 705-11, 1995.
- Hirshowitz B., Lindenbaum E., Har-Shai Y.,
Feitelberg L., Tendler M., Katz D.: Static-electric field induction by a silicone cushion
for the treatment of hypertrophic and keloid scars. Plast. Reconstr. Surg., 101: 1173-79,
1998.
- Cordell J.L., Folini B., Erber W.N., Stein
H., Maso D.Y.: Immunoenzymatic labelling of monoclonal antibodies using immune complexes
of alkaline phosphatase and monoclonal antialkaline phosphatase (APAAP Complex). J.
Histochem, Cytochem., 32: 219-25, 1984.
- Baadsgraad O., Fox D.A., Cooper K.D.: Human
epidermal cells from ultraviolet light-exposed skin preferentially activate autoreactive
CD4+2H4+ suppressor inducer lymphocytes and CD8+ suppressor/cytotoxic lymphocytes. J.
Immunol., 140: 1738 43, 1988.
- Baadsgrad 0., Salvo B., Mannie A., Dass B.,
Fox D.A., Cooper K.D.: In vivo ultraviolet-exposed human epidermal cells activate T
suppressor cell pathways that involve CD4+CD45RA+ suppressor inducer T cells. J. Immunol.,
145: 2854-57, 1990.
- Shen H.H., Talle M.A., Goldstein G. et al.:
Functional subsets of human monocytes contain the cells capable of inducing the autologous
mixed lymphocyte culture. J. Immunol., 130: 698-703, 1983.
- Mori M., Pimpinelli N., Romagnoli P.,
Bernacchi E., Fabbri P., Giannotti B.: Dendritic cells in cutaneous lupus erythematosus: A
clue to the pathogenesis of lesions. Histopathol., 24: 311-21, 1994.
- Maquart F.X., Gillery P., Kalias B., Borel
P.J.: Cytokines and fibrosis. Eur. J. Derm., 4: 91-7, 1994.
- Lee T.Y., Chin G.S., Kim W.J., Chau D.,
Gittes G.K., Longaker M.T.: Expression of transforming growth factor beta 1, 2 and 3
proteins in keloids. Ann. Plast. Surg., 43: 179-84, 1999.
| This paper was received on 11 March 2000. Address correspondence to: Dr Lorenzo
Borgognoni, U.O. Chirurgia Plastics,
Ospedale S.M. Annunziata, Via dell'Antella 58, 50011 Florence, Italy.
Tel./fax: +39 0552496535; e-mail: chplastfi.osma@mclink.it |
| G.
WHITAKER INTERNATIONAL BURNS PRIZE
PALERMO, ITALY
Under the patronage of the Authorities of the Sicilian Region
for 2001
By law n. 57 of June 14th 1983 the Sicilian Regional Assembly
authorized the President of the Region to grant the Giuseppe Whitaker Foundation, a
non-profit-making organization under the patronage of the Accademia dei Lincei with seat
in Palermo, an annual contribution for the establishment of the G. Whitaker International
Burns Prize aimed at recognizing the activity of the most qualified experts from all
countries in the field of burns pathology and treatment.
The amount of the prize is fixed at twenty million Italian Lire. The prize will be awarded
every year by the month of June in Palermo at the seat of the G. Whitaker Foundation.
The Adjudicating Committee is composed of the President of the Foundation, the President
of the Sicilian Region, the Representative of the Accademia dei Lincei within the G.
Whitaker Foundation, the Dean of the Faculty of Medicine and Surgery of Palermo
University, the President of the Italian Society of Plastic Surgery, three experts in the
field of prevention, pathology, therapy and functional recovery of burns, the winner of
the prize awarded in the previous year, and a legal expert nominated in agreeement with
the President of the Region as a guarantee of the respect for the scientific purpose which
the legislators intended to achieve when establishing the prize.
Anyone who considers himself/herself to be qualified to compete for the award may send by
January 31st 2001 a detailed curriculum vitae to: Michele Masellis M.D., Secretary-Member
of the Scientific Committee G. Whitaker Foundation, Via Dante 167, 90141 Palermo, Italy. |
|