Annals of Burns and Fire Disasters - vol. XIII - n. 3 - September 2000 THE IMPORTANCE OF EARLY PHYSICAL THERAPY TO PREVENT CONTRACTURE IN THE BURNED HANDPetronic I., Nikolic G., Markovic M., Marsavelski A., Golubovic Z., Janjic G., Cirovic D. University Children's Hospital, Belgrade, Yugoslavia SUMMARY. Keloid scars are most commonly observed after full-thickness and second-degree burns. Keloid scars are commonly localized on the limbs, face, and neck because of the exposed nature of these parts. A prospective investigation was conducted at the University Children's Hospital in Belgrade over a three-year period, during which 35 children with hand burns were treated. Early physical therapy consisted of electrokinetic therapy, corrective orthosis, and the application of elastic bandages. In the late phase, working hydrokinesia and occupation therapy were performed. After physical therapy the outcome was followed up. A significant number (67.7%) of immature scars healed, unlike mature scars, which had to be managed surgically. Treatment aimed at the aesthetic and functional improvement of the hands. It should be noted that favourable aesthetic results and a full range of movement were achieved only in cases where physical therapy was applied simultaneously with wound epithelializafion and initiated as early as possible in collaboration with the surgeon. Introduction Burns have an important place in the
pathology of children in relation to their frequency and gravity. The severity of burns in
children is also related to the fragility of the child's organism so that an area of
burned surface that does not represent severe injury in an adult may be very dangerous for
a child. Material and method During the three-year period
1996-1999, at the University Children's Hospital in Belgrade, we treated 35 children with
scars secondary to burns of the hand. After completion of the surgical treatment of the
bum, i.e. when epithelialization begins, we carefully examine the burn surface and
investigate the functional state of the surrounding joints. At the first sign of
compromised function or attraction of the surrounding healthy tissue, we initiate
physiatric therapy in an attempt to discontinue the formation of keloids and to promote
the regression of any already existing. Results The majority of burns in the 0-3 year-old group were sustained by the child pulling on an object or during play and play-learning behaviour. Contact with hot solids was in second place. Burns caused by flame were of significant importance in the older age group. This explains why the most frequent localization of scalding was the upper limbs, trunk, and face. Keloid scars were commonly localized in the limbs, face, and neck, because of the greater exposure of these parts (Table 1). We treated 35 children with scars induced by burns in the hand. Keloid scars were most commonly noted after full-thickness burns (84.21 %) and deep second-degree burns (63.93%).
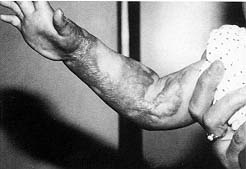
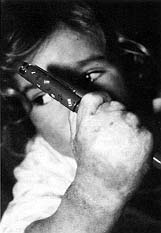
After physical therapy had been conducted a significant number of immature scars were found to have healed, contrary to mature scars, which had to be managed surgically (Figs. 1,2).
In immature keloids leading to extensive functional disorders, surgical therapy is initiated earlier in order to prevent degenerative processes around the joints. Mature (older) keloids cannot in practice be conservatively treated. In such cases surgery must be performed and followed by prolonged physical therapy (Table II).
Discussion The aim of this work is to point out that
in spite of successful treatment, the later phase of burned children's lives may be
affected owing to concomitant consequences. It should however be noted that favourable
aesthetic results and a full range of movement were achieved only in burns where physical
therapy applied simultaneously with wound epithelialization.
RESUME. Les cicatrices chéloďdales se manifestent le plus communément ŕ la suite des brűlures ŕ toute épaisseur et des brűlures de deuxičme degré. Elles sont localisées principalement sur les membres, le visage et le cou, ŕ cause de la majeure exposition de ces parties du corps. Les Auteurs ont effectué une étude prospective pendant une période de trois ans, pendant lequel 35 enfants atteints de brűlures de la main ont été traités dans l'Hôpital Universitaire des Enfants ŕ Belgrade. Les premiers soins physiques consistaient de la thérapie électrokinétique les orthoses correctives et l'application de pansements élastiques. Dans les phases successives les Auteurs ont utilisé l'hydrokinčse du travail et la thérapie occupationnelle. Aprčs la thérapie physique les patients ont été suivis et un nombre significatif (67,7%) des cicatrices immatures sont guéries, contrairement aux cicatrices matures, qu'il fallait traiter chirurgicalement. Le but du traitement était l'amélioration esthétique et fonctionnelle des mains. Il faut noter que les résultats esthétiques positifs et la capacité totale de la mobilité ont été possibles seulement dans les cas oů la thérapie physique et l'épithélialisation ont été efféctuées en męme temps et avec le moindre délai possible en collaboration avec le chirurgien. BIBLIOGRAPHY
|