Annals of Burns and Fire Disasters - vol. XIII - n. 4 - December 2000 DOES INHALATION INJURY REALLY CHANGE FLUID RESUSCITATION NEEDS? A RETROSPECTIVE ANALYSISBollero D.,* Stella M.,* Calcagni M.,* Guglielmotti E.,** Magliacani G.* *Department of Plastic Surgery and Burns Centre, Trauma Centre, Turin, Italy **Department of Anaesthesiology and Intensive Care SUMMARY.The optimization of fluid resuscitation is a key point in the treatment of severely burned patients. In order to improve our knowledge of fluid resuscitation, we performed a retrospective analysis of patients admitted to the Turin Bunts Centre, Italy, in the years 1992-96. The patients were divided into two groups: the first group was resuscitated using the Parkland formula, while the second group received 2 ml/kg/% TBSA of Ringer's lactate in the first 24 h and 0.5 ml/kg/%o TBSA of Ringer's lactate plus 0.5 ml/kg/% TBSA of 5% albumin in the subsequent 24 h. Among the 163 patients included in our study on the basis of our admission criteria, we also considered 44 burn patients with inhalation injury. The mean fluid requirement for resuscitation, in all patients, was 4.32 ml/kg/%. No statistically significant differences were observed between the groups. Only patients whose fluid administration was initially inadequate (i.e., patients admitted to our burn centre within 24 h post-burn but already lacking more than 30% of the predicted amount of fluid) received a significantly smaller amount of fluid. With regard to inhalation, inhalation injury did not in our experience alter fluid requirements during the resuscitation phase. Introduction Patients and methods A retrospective analysis was made of the 593 patients admitted to the Turin Burns Centre in the years 1992-96. Of these, 163 were included in the study on the basis of the following criteria: age < 65 yr, TBSA > 20% (without associated traumas except inhalation), admission to our burn centre within 24 h post-burn.The age range of our patients was between 13 and 65 yr, TBSA was between 20 and 98%, the Roi score" ranged from 0.01 to 0.99, and the UBS score was between 20 and 383. A diagnosis of inhalation injury was pronounced in patients presenting severe hypoxia in the first 24 h requiring intubation and ventilatory support, together with bronchoscopic evidence of heat and/or smoke injury to the airways (Table I). In this series of cases 44 patients fulfilled the criteria.
Two different resuscitation regimens were employed in the first 24 h: the Parkland formula (2 ml/kg/% TBSA in the first 8 h and 2 ml/kg/% TBSA in the following 16 h) and a formula based on Ringer's lactate plus albumin (2 ml/kg/% TBSA as lactated Ringer's in the first 8 h and 0.5 Inn/kg/% TBSA as Ringer's lactate plus 0.5 ml/kg/% TBSA as 5% albumin in the following 16 h).Patients were randomly assigned to the two groups and the total amount of fluid to be given was calculated employing the two different formulas.Resuscitation was considered successful when urine output was >1 ec/kg/h, systolic arterial pressure was > 100 mm Hg. heart rate was < 120bpm. and there was no metabolic acidosis (Table II ).
Fluid administration was adjusted in each patient as required by clinical conditions and laboratorv findings in order to give the least fluid load. The patients were subdivided on the basis of the composition of the fluid used during the resuscitation phase and associated inhalation injury. Four groups were thus obtained (Table lll):
Factors related to burn severity and outcome (age. TBSA, Roi score, and UBS score) did not differ significantly in the four groups. All patients included in the study were correctly resuscitated using the above criteria. Severe complications such as acute renal failure, haemocoa-ulative disorders. and digestive haemorrhaffes were not observed.
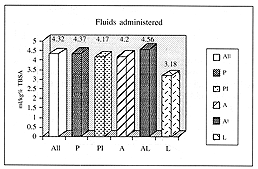
The mean amount of fluid given for correct resuscitation in the first 24 h. considering all patients, was 4.32 ml/kg/% TBSA (standard deviation [SD]. 1.20) (Fig. 1).No statistically significant differences were observed between the four different groups as regards the amount of fluid given for successful resuscitation of the patients. Patients in the first group (P) received 4.37 ml/kg/% TBSA (SD, 1.25 ), patients intubated and resuscitated by the Parkland formula (PI) received 4.17 ml/kg/clo TBSA (SD, 0.99). patients in group A received 4.20 ml/kg/% TBSA (SD, l.l4). and patients intubated and resuscitated with Ringer's lactate plus albumin (AI) were given 4.56 ml/kg/%c TBSA (SD. 1.41). It should be stressed that the indices of burn severity did not differ between the four groups. In our case records. 28 patients received a statistically significant lesser amount of fluid (L): these patients shared the common feature of having been admitted to the burns centre within 24 h post-burn but already lacking more than 30% of the predicted fluid amount. These patients received a mean quantity of 3.18 ml/kg/'7e TBSA (SD, 1.02) and were correctly resuscitated.
Conclusion Successful reanimation was achieved in all cases and no statistically significant differences were observed between the different groups. Only patients who had already been subject to insufficient fluid administration received a significantly lower amount of fluid. It has been hypothesized by some researchers" that albumin administration starting from the 8th h post-burn could reduce the total amount of fluid needed, but our study did not confirm this hypothesis. On the contrary, it is probable that in the first 24 h post-burn the composition of the resuscitation fluid, within certain limitations, makes very little difference. Our data clearly support the idea that formulas provide a reliable starting point for fluid resuscitation, but they are only an initial guide. Consequently, the volume predicted by a resuscitation formula should be modified on the basis of the individual's response to therapy. For instance, groups A and A1 had a predicted fluid volume of 3 ml/kg/% TBSA in the 24 h but they in fact received a greater amount of fluid (more than 4 ml/kg/°lo TBSA). Clinical observation and adaptation to the needs of the individual patient are therefore mandatory, and the amount of fluid should always be enough to maintain vital organ function. Regarding the choice of resuscitation parameters, we opted for the following: urine output >_ I cc/kg/h, systolic arterial pressure < 100 mm Hg, heart rate < 120 bpm, and absence of metabolic acidosis. As to the diagnosis of inhalation injury, debate is still open as to which parameters have to be correctly analysed; we adopted the condition of severe hypoxia together with bronchoscopic evidence of heat and/or smoke injury to the airways. With regard to inhalation, in our experience inhalation injury did not alter fluid requirements during the resuscitation phase. However, the subject remains controversial.We can therefore conclude that burn patients with associated inhalation injury do not need a different approach as regards fluid composition and volume: in the first 24 h careful monitoring of the evolution of the patient's clinical condition is probably more important than the application of strictly empirical formulas.
SUMMARY. L'optimisation de la reanimation liquide est fondamentale dans le traitement des grinds Mies. Pour arnéliorer leur connaissance de la reanimation liquide, les Auteurs ont effectug une analyse retrospective des patients hospitalisbs dans le Centre des Mies de Turin pendant les ann6es 1992-96. Les patients ont été divisés en deux groupes: le premier a été réanimé avec Fernploi de la formule de Parkland, tandis que les autres patients ont recu 2 tnl/kg/pourcentage de la surface totale corporelle brîtlde (STCB) de lactate de Ringer clans les premičres 24 h et 0,5 ml/kg/pourcentage STCB d'albume dans les 24 h successives. Les Auteurs ont inclus parmi les 163 patients compris dans leur etude selon les critéres d'admission aussi 44 patients brîtlés atteints de lesions d'inhalation. La quantité moyenne de liquides nécessaires pour la reanimation, tons patients compris, était de 4,32 ml/kg/pourcentage STCB. Les Auteurs n'ont observe aucune difference significative entre les différents groupes. Settlement les patients qui ont recu une administration de liquides insuffisante dčs I'origine (c'est-ŕ-dire les patients hospitalises dans le Centre des Auteurs moins de 24 h aprčs la lesion mais déjŕ en retard de plus de 30% sur la quantitb de liquides calculée) ont recu une quantite significativement inférieure de liquides. Pour ce qui concerne Finhalation, selon 1'expérience des Auteurs elle ne modifie pas la domande de liquides pendant la phase de la reanimation. BIBLIOGRAPHY indices. J. Trauma, 23: 1023-0, 1983 severely burned patients. Ann. Surg., 223: 14-25, 1996.
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||