Annals of
Burns and Fire Disasters - vol. XIII - n. 4 - December 2000
EVALUATION OF THE VALIDITY OF THE HAIFA FORMULA FOR FLUID RESUSCITATION IN
BURN PATIENTS AT THE RAMBAM MEDICAL CENTRE
Ullmann Y., Kremer R., Ramon Y.,
Berger J., Ullmann A., Peled I.J.
Plastic and Reconstructive Surgery
Department and Burn Unit, Rambam Medical Centre, and Technion Faculty of Medicine, Haifa,
Israel
SUMMARY. In
order to evaluate the validity of the Haifa formula for the fluid resuscitation of burn
victims, we retrospectively evaluated the files of 72 burn patients treated in the burn
unit of the Rambam Medical Centre (Israel) during the years 1990-95. According to this
formula, the estimated quantity of fluid to be given in the first 24 h is: plasma - 1.5 cc
x kg x percentage burned TBSA and Ringer's lactate - 1 cc x kg x percentage burned TBSA.
Half of this is given in the first 8 h and the other half in the successive 16 h. The
fluid estimation for the next 24 h is half the amount estimated for the first day. We
included patients over 15 yr old with burns of 20-80%o TBSA, without smoke inhalation. We
divided the patients into three subgroups on the basis of the extent of the burned area -
subgroup 1: 20-34% TBSA; subgroup 2: 35-49% TBSA; subgroup 3: above 50%o TBSA. We found a
good correlation between the volume of plasma recommended by the formula and the amount
actually given. We found a substantial difference between the quantity of Ringer's lactate
recommended by the formula and the quantity actually given to patients with less than 50%
TBSA, during the first day. Since the hourly urine output per kg was relatively high (1.66
cc/kg/h), we concluded that haemodynamic instability was not the cause of the deviation.
Respiratory complications were recorded in 12.5% of our patients and sepsis in 60%; the
mortality rate was 5.5%. These data are consistent with those found in the literature,
although about 25% less fluid was given to our patients than that recommended by the
Parkland formula. Complications attributed to fluid overload, such as ileus and
compartment syndromes, were not recorded. It was possible to initiate early enteral
feeding in all the patients.
Introduction
It is now well established that fluid
management is fundamental in the treatment of burn patients during the immediate
post-trauma period. The quality of this treatment is prognostic for the outcome.
The opinions of physicians involved in the treatment of the burn trauma vary as to the
best solution and to the correct amount to be used. Many scientific papers deal with the
issue.
A burn causes the accumulation of fluid in the burned area but also in tissues not
directly involved, owing to the release of vasoactive substances from the damaged tissues.
Burns covering more than 20% TBSA may cause hypovolaemic shock if not treated properly.
Tissue oedema develops quickly during the first 6-8 h and continues gradually during the
next 18-24 h post-burn.
Infectious mediators released from activated platelets, macrophages, and leukocytes in the
burned area cause higher permeability of the blood vessels and high capillary flow.Z There
is a leakage of intravascular components into extravascular spaces, leading to a decrease
in intravascular volume. The prominent mediator during this phase is histamine, released
from the mast cells, which acts mainly on receptors located on the venules.
Prostaglandins, the derivates of arachidonic acid, cause vasodilatation of the arterioles,
thus increasing flow to the injured tissues and raising hydrostatic pressure, which
further contributes to the leakage.
The mediators released in extensive burns may cause multiple organ failure, and ultimately
death.
The purpose of fluid resuscitation is to prevent burn shock by giving adequate fluid,
without overloading the vascular system or causing excessive oedema. The Parkland formula
is the one most widely in the treatment of burn patients. The supporters of the Parkland
formula believe that using Ringer's lactate alone is as good as using more expensive
solutions. The disadvantage of this formula is the enormous amount of fluid given,
resulting in extensive oedema in all the organs.
In order to restrict oedema Monafo` suggested using a solution containing 250 mEq Na, 150
mEq lactate, and 100 mEq Cl. The amount needed is monitored on the basis of urine output.
The rationale of this method of management is that by raising intravascular osmolarity
less fluid is required. Demling proved this thesis in an animal model.' Huang failed to
reach the same conclusion and observed higher rates of renal failure and mortality in
animals treated with the hypertonic solution.
It is an established fact that plasma proteins play an important role in building up
oncotic pressure in the blood vessels, thus contributing to maintaining fluid
intravascularly. This physical principle is the basis of formulations containing colloids
in addition to crystalloids - this combination is used by the formulations of Evans and of
Brooke (the latter also includes dextrose 5%).
Goodwin and others claim that if colloids are given early during the resuscitation period
they may cause accumulation of fluid in the interstitium of the lungs.
Demling recommended using fresh frozen plasma (FFP') in accordance with the following
formula: 0.5-1 x % TBSA x body weight (kg), with colloids starting only 8 h post-burn.
Slater recommended using FFP: 75 ml x body weight (kg) during the first 24 h, with the
addition of 2 1 Ringer's lactate. Plasma is added according to the amount of urine.
The Haifa formula
We have been using this formula since
1990. It is a modification of the Slaterformula, adjusted to include the extent of the
burn. The amount of fluid given during the first 24 h is as follows: plasma (cc) - 1.5 x %
TBSA x body weight (kg); Ringer's lactate (cc) - 1 x % TBSA x body weight (kg). Half the
estimated amount is given in the first 8 h and the other half in the next 16 h. In the
subsequent 24 h, we give half the amount estimated for the first day. The sufficiency of
the fluid is judged mainly on the basis of urine output, since we try to avoid any more
invasive monitoring, unless it becomes necessary. Less than 0.5 cc urine per h per kg body
weight is an indication for the addition of Ringer's lactate to the previously estimated
fluid. Restriction of the fluid is possible due to the use of colloids, which help to keep
the fluid in the vessels.
Limiting the total fluid given is believed to reduce the rate of complications caused by
fluid leakage, with a lower rate of oedematous lungs and better myocardial function.
Oedema of the central nervous system may cause nausea and disturb consciousness. An
oedematous gastrointestinal tract tends to cause ileus and disturbance of intestinal
absorption, thus preventing early feeding, which is critical in the treatment of the burn
patient.
The purpose of the present paper was to check the validity of the Haifa formula, in terms
of the adequacy of the estimated fluid, and to find out if there were any exceptions to
the formula and the possible causes. We also checked some parameters regarding final
outcome to see if we were staying within the standard limits of good care.
Materials and methods
A retrospective study was carried out
based on the files of 100 burn victims treated in the Rambam Medical Centre Burn Unit in
Israel in the years 1990-95. Patients with second- and third-degree burns in 20-80% TBSA
and aged 15 yr and over were included in the study. Twentyeight files were excluded
because they lacked part of the information needed for the study.
The data collected included fluid amounts, patients' weight, % TBSA burned, early and late
complications, urine output, and hospitalization time.
The statistical analysis included the Student T test, the Leven test, and the Pearson
test.
Results
The experimental group included 72
patients, 46 men (65%) and 26 women (35%). The mean age of the men was 26 yr and that of
the women 33 yr.
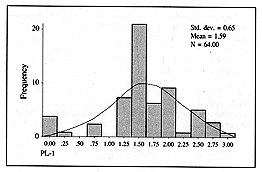
We defined as PL-1 the quantity of plasma given in the first 24 h: PL-1 = plasma (ml) in
first 24 h / kg x % TBSA. According to our formula the expected PL-1 was 1.5, but we found
that the mean value of plasma actually given in the first 24 h was 1.59, with a p value of
0.272 (not significant) (Fig. 1).
We defined as RL-1 the quantity of Ringer's lactate given in the first 24 h: RL-1 =
Ringer's lactate (ml) in first 24 h / kg x % TBSA. According to the formula, the expected
value was 1, but the value of the mean amount of Ringer's solution actually given to the
patients was significantly different: 1.78 (p < 0.0001) (Fig. 2).
 |
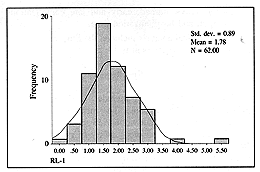 |
Fig. 1
- The distribution of the PL-1 value. |
Fig.
2 - Distribution of the RL-1 value |
|
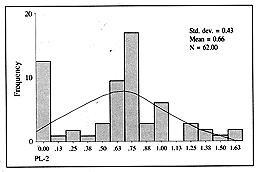
PL-2 means the plasma given
in the successive 24 h: PL-2 = plasma (ml) in successive 24 h / kg x % TBSA. The expected
value was 0.75, and the value calculated for the amount given was not significantly
different: 0.66 (p = 0.105) (Fig. 3).
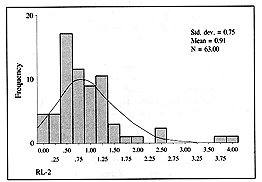
RL-2 refers to the amount of Ringer's lactate given in the subsequent 24 h: RL-2 =
Ringer's lactate (ml) in the subsequent 24 h / kg x % TBSA. The expected value was 0.5,
but the calculated value was significantly different: 0.91 (p < 0.0001) (Fig. 4).
 |
 |
| Fig. 3 -
Distribution of the PL-- value. |
Fig. 4
- Distribution of the RL-2 value. |
|
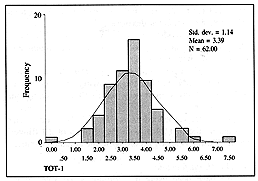
TOT-1 was defined as
follows: TOT-1 = Ringer's lactate (ml) + plasma (ml) in first 24 h / kg x % TBSA. The
expected value was 2.5 but the calculated value for the fluid actually given during the
first day was significantly different: 3.39 (p < 0.001) (Fig. 5).
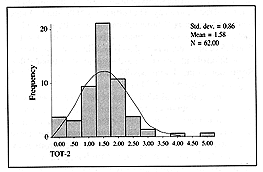
TOT-2 value was defined as follows: TOT-2 = Ringer's lactate (ml) + plasma (ml) in the
subsequent 24 h / kg x % TBSA. The expected value was 1.25, while the mean amount
actually given was 1.58, with a p value of 0.86 (Fig. 6).
 |
 |
| Fig. 5
- Distribution of the TOT-7 value. |
Fig. 6 -
Distribution of the TOT-2 value. |
|
The amount of fluid actually given on the
second day was thus not significantly different from that expected, although more Ringer's
lactata was given.
In order to obtain more information about our use of the formula vs a divided our patients
into three subgroups on the basis of their burned TBSA:
- subgroup 1: 34 patients with bums estimated to be 20-34%
- subgroup 2: 19 patients with 35-49% burns
- subgroup 3: 11 patients with 50-80% burns
Table I shows the results in relation to
the three subgroups. The results after the division into the three subgroups show that on
the first day the amount of plasma given was not significantly different from that
expected on the basis of the formula. However. the amount of Ringer's solution liven in
two subgroups (20-3-1~'c and 35-49%) was significantly higher than that recommended by the
formula. as also the total fluid given. In the third subgroup, the deviation from the
formula was not significant in the three values investigated.
|
PL-1 |
RL-1 |
TOT-1 |
| Mean |
1.7 |
1.87 |
3.57 |
| S.D. |
0.64 |
1 |
1.38 |
| No. |
34 |
34 |
34 |
| T test (p value) |
0.08 |
0 |
0 |
| Subgroup 2
(TBSA 34-49%) |
|
PL-1 |
RL-1 |
TOT-1 |
| Mean |
1.4 |
1.9 |
3.38 |
| S.D. |
0.72 |
0.67 |
0.78 |
| No. |
19 |
19 |
19 |
| T test (p value) |
0.55 |
0 |
0.0001 |
| Subgroup 3
(TBSA 50% and more) |
|
PL-1 |
RL-1 |
TOT-1 |
| Mean |
1.6 |
1.29 |
2.9 |
| S.D. |
0.47 |
0.55 |
0.86 |
| No. |
11 |
11 |
11 |
| T test (p value) |
0.49 |
0.11 |
0.15 |
|
| Table I -
Distribution of results on day 1. in relation to the subgroups. Expected values were: PL-1
= 1.5, RL-1 = 1, TOT-1 = 2.5 |
|
Table II demonstrates
the results for the second day the only significant differences were in RL-2 in the second
subgroup. and we can thus conclude that on the second day the quantity of fluid actually
given corresponded well to the recommendation of the formula.
| Subgroup
I (TBSA 20-34%) |
| |
PL-2 |
RL-2
|
TOT-2 |
| Mean |
0.63 |
1 |
1.67 |
| S.D. |
O.d7 |
0.97
|
1.1 |
| N0. |
34 |
34 |
34 |
| T test (p
value ) |
0.15 |
0.005
|
0.052 |
| Subgroup
2 ITBSA 35-49%) |
| |
PL-2 |
RL-2 |
TOT-2 |
| Mean |
0.69 |
0.86 |
1.56 |
| S.D. |
0.-14 |
0.39 |
6.5
3 |
| No. |
19 |
19 |
19 |
| T test (p
value ) |
0.56 |
0.0008 |
0.84 |
| Subgroup
3 iTBSA 50% and more) |
| |
PL-2 |
RL-2 |
TOT-2 |
| Mean |
0.6-1 |
0.71 |
1.35 |
| S.D. |
0.31 |
0.49 |
0.58 |
| No. |
11 |
11 |
11 |
| T test (p
value) |
0.37 |
0.19 |
0.58 |
|
| Table 1I - Distribution on
day 2, according to the subgroups: PL-1= 1.5, RL-1 = 1, TOT-1 = 2.5 |
|
Urine output. The
urine value (U) was defined as follows: U = urine (ml) / kg x h. The mean value in our
study was 1.67. indicating that the mean urine output was three times higher than that
recommended, which is 0.5 ml per h per kg body- w eight. There was no difference in the U
value between the three (p = 0.690. as shown in Table III..
| |
Mean value
(h/kg) |
S.D. |
| Subgroup
1 |
1.85 |
0.9 |
| Subgroup
2 |
1.62 |
0.78 |
| Subgroup 3 |
1.-16 |
0.66 |
|
| Table III - Distribution of
L' value. The difference between the subgroups was not significant (p = 0.69) |
|
Hospitalization time. The
results show that the mean hospitalization time was 36.6 days (subgroup 1, 31.5 days;
subgroup ?, -16.5 days: subffroup 3. 36 days). There was no correlation between
hospitalization time and TBSA burn.
Sepsis. In this study 58.75'c of the patients developed sepsis. whether haematogenic or
due to the burn wound. The mean TBSA burned in septic patients was 41/0, while the mean
TBSA burned in patients without sepsis was 27%. Applying the T test to the results
produced a significant correlation between TBSA burn and the occurrence of sepsis (p >
0.0001): there was also a high correlation between hospitalization time and sepsis (p >
0.001).
Pubnonary complications. ARDS and/or pneumonia occurred in nine patients (1?.5%). who
needed intubation and mechanical ventilation. This was too small a group for statistical
evaluation.
Discussion
The treatment of burns is a real medical
challenge. It starts with evaluation of the patient and continueswith fluid and sometimes
respiratory resuscitation. local treatment, surgery, antibacterial treatment, and
rehabilitation, all of which require the collaboration of a multidisciplinary team.
In recent years there has been a great improvement in the outcome of burn patients,
reflected in a higher survival rate, better and faster rehabil�tation, and fewer early
and late complications. This improvement is the result, of a better understanding of the
various supportive treatments.
The present studs was designed to elamine only the aspect of fluid resuscitation in our
burn unit. we wanted to learn how closely w e actually followed our fluid formula and to
consider the possible influence of this management on the complication rates, as well as
some aspects of the outcome.
Since 1990 we have been using the Haifa formula, in which we integrate plasma and Ringer's
lactate for the fluid resuscitation of burn patients during the first 48 h post-burn.
The Haifa formula is defined as follows: plasma (ml) = 1.5 x %o TBSA x body weight
(kg); Ringer's lactate (ml) = 1 x % TBSA x body weight (kg). Half the estimated amount is
given in the first 8 h and the other half in the following 16 h.
Generally speaking, the use of a formula helps physicians to estimate the fluid needed by
patients on the basis of their TBSA burned and weight. But this is just an indication,
which has to be adjusted in relation to the patients' needs, as estimated by careful
monitoring.
A good formula is one that needs fewer adjustments when tested over a substantial period
of time. This is the aspect which this retrospective study is intended to clarify.
Validation of the formula will give staff a reliable tool they can use.
We omitted from the study patients with smoke inhalation, patients whose treatment was not
initiated in our hospital, children, and patients with inadequate data in their files. We
investigated the validity in the whole group and in subgroups established on the basis of
TBSA.
In this study the plasma component was well validated. This means that the deviation from
the amounts recommended on the first day, as standardized by the PL-1 value, was not
statistically significant (p > 0.05). This was found both generally and in each of the
subgroups investigated. Deviations at the edges of the graft were attributed to the
re-evaluation of TBSA that is always performed the morning after the day of admission.
Plasma was stopped on day 2 in 12 patients because of a change in their TBSA estimate.
In the Ringer's lactate component we found a notable deviation from the formula on the
first day. This is the adjustable component of our formula, where Ringer's lactate is
given according to the patient's condition. The RL-1 value was found to be higher than
that recommended in the first two subgroups but surprisingly not in the third group, which
included the more extensive burns (TBSA of 50% and more).
We tried to find out if the deviation from the formula in the Ringer's lactate component
on the first day could be attributed to haernodynamic instability. One of the most
reliable monitors of the haemodynamic situation is urine output. The U value (urine output
per h per kg body weight) was found to be higher than what is believed to be an adequate
value, i.e. 0.5 cc. The mean value in our study was 1.66 cc, with no significant
difference between the subgroups. One possible explanation is that U, which is a mean
value, does not reflect the values of the whole day, so that it is possible that during
the day there were some hours with low urine output which induced a young physician on
duty to add Ringer's lactate.
The total fluid given to the patients in the first 24 h was also significantly higher (p
> 0.05) than that recommended by the formula. This was however due to the Ringer's
lactate component only. The mean TOT-1 in our study was 3.4 cc, compared with the formula,
which is 2.5 cc, and with the Parkland formula, which is 4 cc. Also here the deviation was
significant only in subgroups 1 and 2, and nonsignificant in subgroup 3 (p = 0.13).
The main goal in adapting a formula is to keep the patients well hydrated and in good
haemodynamic condition by maintaining the amount of fluids as low as possible and to avoid
the complications caused by other formulations that use more fluids.
In our study we found that our patients were treated with less fluid than that suggested
by the Parkland formula but also that the crystalloid component in the two subgroups with
TBSA 20-49% was unjustifiably higher than that prescribed by the formula.
During the second day the deviation from the formula was not significant in terms of total
fluid given, although more Ringer's lactate was given and less plasma, mainly because of a
reduction in the estimate of the burn area, followed by suspension of the plasma component
after reevaluation on the second day.
We learned from this study that during the first day after admission our resident
physicians should react more cautiously before administering more fluid to these patients.
In this study we also tried to check other aspects concerning the quality of our treatment
in comparison with others in the literature, even though these data are not a direct
consequence of the fluid regimen.
Mortality. Four deaths were recorded (5.5%0) in the 72 files checked for this study. It
should be recalled that the study included only burns with a TBSA over 20%o and a mean
TBSA of 36.6%0.
In his study, Frye summarized the treatment of 1585 burned patients over a 7-yr period
(1988-95) and found a mortality rate of 4.5%.'- Peck reported that among 196 patients with
mean TBSA 7.2%o the mortality rate was 7.7%0.'3 In these two studies the resuscitation
formula was not reported. Our mortality rate was comparable to these two studies, although
the mean TBSA in our work was higher. It is reasonable to attribute some of the success to
treatment during the critical period.
Infection rate. Extensively burned
patients have the tendency to develop infections that need systemic antibiotic treatment.
Among the causes are impairment of the external defence mechanism, lowering of the immune
system, long hospitalization, and invasive monitoring."
Our policy is to try to avoid using unnecessary invasive monitoring. Among our patients,
59.7% needed antibiotic treatment, i.e. patients presenting burn wound sepsis positive
blood cultures and septic shock. Peck also reported that 60% of his patients needed
antibiotic treatment, although the mean TBSA of his patients was lower.
Sepsis is influenced by multiple factors, and there is no direct influence of the
resuscitation formula on the incidence of the sepsis. There was no recorded viral
(hepatitis or HIV) infections among our patients. In fact, during the last 20 years that
we have been using other formulations that include plasma, there has been no case of viral
infection among our burn patients. This can be attributed to the perfect screening of
donated blood in our country.
Pulmonary complications. Burn
patients are at high risk for the development of pulmonary infections and ARDS. The
tendency for pulmonary complications is higher among patients who have suffered smoke
inhalation. Respiratory failure is connected with a higher rate of multiorgan failure and
a mortality rate of 27-50%.'S Most of the cases in this study did not present smoke
inhalation, and respiratory failure developed in only nine patients (12.5%). In Peck's
study, 12% of the patients needed mechanical ventilation, owing to pneumonia or ARDS.
Goodwin' reported that a combination of colloid and crystalloid solutions permitted
haemodynamic stabilization with smaller amounts of fluid. However, he also noted that more
pulmonary fluid collection was found in the lungs of such patients on day 7 post-burn,
compared with patients treated only with crystalloids.
The influence of the combination of these two solutions on the incidence of ARDS, in
comparison with the use of crystalloids alone, has not yet been investigated. We can
however speculate that smaller amounts of fluid with high osmotic pressure may keep the
lungs "drier" and lead to a lower complication rate.
Although we gave our patients colloids 4 to 5 h after the burn, in contrast to some other
methods, the pulmonary
complication rate was not higher than others reported in the literature.
Hospitalization time. The
hospitalization time of burn patients is a rough parameter of the severity of their
illness and the success of treatment. The mean hospitalization time in this study was 36.5
days. We found a significant difference in mean hospitalization times between patients who
had sepsis and patients who did not (p > 0.0001).
We have shown that hospitalization time was closely related to the occurrence of sepsis,
but as there is no connection between sepsis and fluid management we could find no link
between fluid management and hospitalization time.
Conclusion
Our review of 72 files of our burn
patients validates the Haifa formula with regard to its plasma component, while the
validity of the crystalloid component was proved only in patients with a burned TBSA of
more than 50%.
The addition of crystalloids beyond the required amount can be mainly attributed to an
overliberal addition of Ringer's solution in patients with a TBSA of less than 50%.
Restriction of fluids by about 25%, compared with the Parkland formula, did not cause
higher complication rates. However, we saved our patients from complications attributed to
the overloading of fluids, such as compartment syndromes, ileus, and bowel syndrome. We
were able to feed patients enterally from the first day, and we thus saved them from
complications due to late feeding.
The mean urine output was three times higher than the minimum expected.
The debate concerning the ideal formula for burn patients is not over yet, but the
potential harmful effects of the fluid overload caused by formulas using only crystalloids
should be considered." And in the light of the most recent debates on the use of
albumin in critically ill patients," the use of plasma seems to be reasonable.
RESUME. Pour �valuer la validit� de la "formule de Haifa"
clans la reanimation des patients br�l�s les Auteurs ont �tudi� les dossiers cliniques
de 72 patients trait�s clans 1'Unit� de Brnlures du Centre Medical Rambam en Israel
pendant les ann�es 199095. La quantit� de ftuides administr�e pendant les premi�res 24
h est la suivante: plasma = 1,5 cc x kg x % surface corporelle br�l�e totale (SCBT);
Ringer = I cc x kg %o SCBT. La moiti� est administr�e clans les premi�res 8 h et Fautre
moiti� pendant les 16 h successives. La quantit� estim�e pour les 24 h successives est
la moiti� de la quantit� pour le premier jour. Les Auteurs ont inclus clans 1'�tude les
patients �g�s de plus de 15 ans atteints de brfilures de 20-80% SCBT, sans inhalation de
fum�e. Les patients ont �t� divis�s en trois sous-groupes sur la base de Faire br6l�:
sous-groupe 1, 20-34%n SCBT; sous-groupe 2, 35-49%o SCBT; sousgroupe 3: plus de 50%o SCBT.
Les Auteurs ont trouv6 une bonne correlation entre le volume de plasma recommand� par la
formule et la quantit� effectivement administr�e. Its ont trouv� une difference
considerable entre la quantit� de Ringer recommandee par la formule et la quantit�
effectivement administr�e aux patients atteints de br�lures clans moins de 50%o SCBT,
pendant les premi�res 24 h. Puisque la production horaire d'urine �tait relativement
�lev�e (1,66 cc/kg/h), les Auteurs ont conclu clue la cause de cette deviation n'�tait
pas Finstabilit� h�modynamique. Its ont observe un taux de complications respiratoires
de 12,5% clans les patients atteints de sepsis de 60%. Le taux de mortalit� �tait 5,5%.
Ces r�sultats sont compatibles avec ceux de la litt�rature, bien clue les patients aient
requ 350c moins de fluide par rapport � la quantit� recommand�e par la formule de
Parkland. Les Auteurs n'ont pas obsers � de cas de surcharge liquide. comme par
example 1'il�us, ni de syndromes de compartiment. Il a �t� possible de commencer
1'alimentation ent�rale pr�coce dans tons les patients.
BIBLIOGRAPHY
Monafo bI.: Initial management of burns. \. Eng. J. NIed..
335:1581-5, 1996.
Pitt R.M., Parker J.C., Juhovich G.S.. Taylor A.E.. Curreri
P.y~'.: Analysis of altered capillary pressure and permeability after thermal injury. J.
Sure. Res.. 43: 693-702. 1987.
Glenn DAN'.: Burn shock resuscitation. World J. Surg.. 16:
16-23.1992.
Leape L.: Tissue changes in burned and unburned skins of
Rhesus 1-1 monkeys. J. Trauma. 10: 188-92. 1970.
Cavajal H.F., Broubard B.H.. Linares H.A.: Effect of
antihistamineantiserotonin and ganglionic blocking agents upon increased capillary
permeability follo" ina burn edema. J. Trauma. 15: 96975. 1975.
Monafo W.W.: Treatment of burn shock by intravenous and
oral administration of hypertonic lactated saline solution. J. Trauma. 10:575,1970
Demling R.H.: Burn edema paft II: Complications.
prevention. and treatment. J. Burn Care Rehabil.. 3: 199,1982.
Huang P.P.: Hyperbaric sodium resuscitation is associated
with renal failure and death. Ann. Surg., 231: 5-13-7 (discussion 554-7). 1995
Goodwin CAN'.: Randomized trial of efficacy of crystalloid
and colloid resuscitation on hemodvnamic response and lung water following thermal injury.
Ann. Surg.. 197: 5?0-31. 1983.
Demling R.H.: "Fluid resuscitation in the art and
science of burn care". Aspen Publishers Inc., 189-302. 1987.
Du G., Slater H., Golfard JAL Influences of different
resuscitation regimens on acute early weight gain in extensively burned patients. Burns.
17: 14'-50, 1991.
Frye K.E.. Jzenberg S.D., Williams OLD.. Luterman A.:
Simulated biologic intelligence used to predict length of stay and survival of burns. J.
Burn Care Rehabil.. 17: 510-6. 1996.
Peck M.D.. hlontelle L.. Word C.G.: Comparison of length of
hospital stay to mortality rate in a regional burn center. J. Burn Care Rehabil.. 17:
39-1-1. 1996.
Vurtz R.. Uara Jovic ifL. Dacumos E.. Javanovic B..
Hanumadass DL: Nosocomial infections in a burn intensive care unit. J. Burn Care Rehabil..
181-4. 1995.
Hollingsed T.C.. Saffle S.R.. Bonon R.G.. Craft "-.B.,
Morris S.E.: Etiologic consequences of respiratow failure in thermally injured patients.
Am. J. Sura.. 166: 592-7. 1993.
Bert J.. Gvenge C.. Bowen B. et al.: Fluid resuscitation
following a burn injury: Implications of a mathematical model of microvascular exchange.
Burns, '_'3: 93-105, 1997.
Cole R.P.: The UK albumin debate. Burns. 25: 565-8. 1999.
This paper was received
on 3 March 2000.
Address correspondence to:
Yehuda Ullmann 1f.D.,
Plastic and Reconstructive Surgery Department and Burn Unit. Rambam
Medical Centre. and Technion Faculty of Medicine.
Haifa. Israel. |
|





