Annals of Burns and Fire Disasters - vol. XIV - n° 1 - March 2001 EVALUATION OF "MICROMAT" DRESSING (VISCOSE POLYMER VEHICLE FOR CHLORHEXIDINE) IN PARTIAL-THICKNESS BURNS AND SKIN GRAFT DONOR SITES Bhattacharya S., Ahuja R.B., Topaz M., Tripathi C.D. Department of Burns and Plastic Surgery, Plastic Surgery Unit, Lok Nayak Hospital & Associated Maulana Azad Medical College, New Delhi, IndiaPlastic Surgery Unit, Hillel Yaffe Medical Center, Hadera, Israel Department of Pharmacology, Lok Nayak Hospital & Associated Maulana Azad Medical College SUMMARY. In this study, "Micromat"® 0.5% (a chlorhexidine-impregnated viscose polymer dressing) was evaluated for treatment of partial-thickness burns and split skin graft donor sites with a dual objective: one, to compare the dressing with traditional methods, and two, to study viscose polymer as a vehicle for delivering chlorhexidine. Only fresh cases of partial-thickness burn injury between 10-25% total body surface area (TBSA) in patients over 12 years of age were included in the study. All consecutive split skin graft donor sites harvested with a Watson's modified Humby's knife were included for the other part of the trial. Thirty patients with partial-thickness burns and 30 split thickness skin graft donor sites were evaluated. In nine patients with 20% TBSA deep dermal injury, mirror-image areas of burns were available for comparison. In these, one side was dressed with 1 % silver sulphadiazine cream, which acted as a control. Burn dressings were changed after 72 h, or as warranted by the state of the wound and the patient's general condition. Additionally, in six patients with 20% TBSA burns, chlorhexidine estimation was performed in blood. In split skin graft donor sites, the proximal half was dressed with Micromat 0.5% and the distal half with ordinary paraffin gauze (Fairlie, Johnson & Johnson). The dressings were allowed to separate by showering after 10-11 days. We observed no difference in the healing rate or pattern between Micromat treated wounds and controls. Amongst the burn patients there was no conversion of partial-thickness injury to full-thickness in either group. Many burn wounds treated with Micromat were found to be dry at the time of dressing change. Also, there were no complications like wound sepsis or septicaemia requiring substitution of the local antimicrobial agent or a need for systemic antibiotic in any of the patients. Chlorhexidine could not be detected in the blood sample of any patient. Thus, for partialrhickness burn injury in up to 25% TBSA, treatment with Micromat compares favourably with 1% silver sulphadiazine cream, and For treatment of skin graft donor sites the results of Micromat and ordinary paraffin gauze are comparable, and the former has the added advantage of delivering an effective antibacterial agent. It was also observed that viscose polymer was an effective vehicle for delivering chlorhexidine. Micromat dressing was easy to handle and relatively non-adherent, and had a capacity to absorb the discharge. Introduction Partial-thickness
burns and split skin graft donor sites heal by epithelialization from surviving
pilosebaceous units. Their healing demands a proper environment for survival of these
epidermal units. Dressings are required during this period to provide physical protection,
contain exudate, diminish pain, avoid infection, and enhance the healing process, if
possible, by providing a moist environment. Thus, partial-thickness burns and skin graft
donor sites provide a good model for the evaluation of newer dressing materials.
Material and method The study consists of
two parts: Micromat 0.5% dressing was evaluated in partial-thickness burns and a
comparison with 1 % silver sulphadiazine was attempted wherever mirror-image areas of burn
were available. Micromat 0.5% dressing was also compared with paraffin gauze dressings
(Fairlie, Johnson & Johnson ) in split skin graft donor sites. Protocol criteria
included only fresh cases of partialthic:kness burn injury between 10 and 25% TBSA in
patients who were over 12 years of age. Even though it was not specified by protocol, all
patients had a significant percentage of deep dermal injury as admission logistics
excluded others. All consecutive split skin graft donor sites harvested with a Watson's
modified Humby's knife were included for the other part of the trial. Micromat dressing is
made of knitted viscose polymer impregnated with chlorhexidine gluconate in a
concentration ranging from 0.5 to 2%. It is a hydrophilic and nonadherent sheet. The agent
is activated by coming in contact with an aqueous environment, such as body fluid,
medication, saline, distilled water, etc. The viscose polymer vehicle has good absorption
qualities and can imbibe fluid equivalent to its weight. It does not adhere to the wound
bed, making removal painless and atraumatic. Chlorhexidine has broad-spectrum
antibacterialactivity against both gram-positive and gram-negative bacteria. It is
impregnated on the viscose polymer in a sustained release formulation which obviates
frequent changes of dressing. The dressing can thus be retained for 72 h unless excessive
exudate or patient condition warrants an earlier change. Micromat is available in various
sheet sizes: 10 x 10 cm, 10 x 15 cm, and 10 x 20 cm. It is packed singly in sterile
sachets. After application the dressing is moistened by saline irrigation and covered with
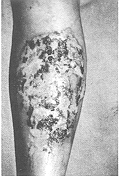
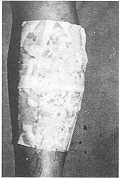
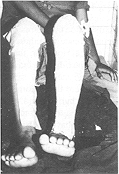
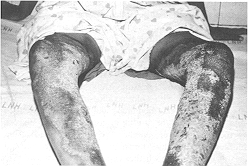
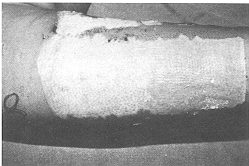
gamgee pads and bandaged much like an ordinary paraffin gauze. This group consisted of 30 patients allocated by the selection criteria. Burns > 25% TBSA were excluded from this study as, presumably, chlorhexidine alone would not have been sufficient to combat development of wound sepsis in such patients. Patients with inhalation injury and other associated injuries and those with metabolic or systemic disease were also excluded. All patients in this group had a significant component of deep dermal injury, since patients with superficial burns, even of this magnitude, do not get admitted for want of sufficient beds. Patients requiring intravenous resuscitation were given fluid according to the Parkland formula (3 ml/kg/%a TBSA burn). All patients were dressed within 4-5 h of sustaining burns. In nine patients mirror-image areas of identical depth were available for comparison to act as controls. The control areas were treated with 1% silver sulphadiazine cream. The trial areas were dressed with Micromat having 0.5% chlorhexidine. Dressings were changed every 72 h in the trial area unless an earlier inspection was warranted by wound condition. Control areas were generally dressed daily or maximum after 48 h. Preliminary photographs and wound descriptions were recorded and pre-dressing wound swabs sent for culture/sensitivity tests. The progress of healing was observed and a photographic record maintained (Figs. 1, 2).
Pus swabs were sent for culture and sensitivity tests at each dressing change. Additionally, in six randomly selected patients with burn injury of more than 20% TBSA we estimated chlorhexidine levels in blood. Five millilitres of blood were collected from a peripheral vein at 2, 4, and 6 h intervals after the second application of Micromat 0.5%. Serum was separated and stored at -20 °C until analyses were performed. Estimation of chlorhexidine gluconate was carried out by a modified method as described in British Pharmacopeia'2 by HPLC. In this procedure a stainless steel column (20 cm x 4 mm) packed with stationary phase C (IOum) (Nucleosil ODS) was used. The mobile phase of 0.01 m sodium octane sulphonate in a mixture of 73 volumes of methanol, 27 volumes of water, and glacial acetic acid was prepared and a flow rate of 1.5 ml/min was maintained. A detection wavelength of 254 nm was used. The method showed sensitivity of 0.05-0.1 ug/ml. Study of skin graft donor sites This group included
30 patients who consecutively underwent skin grafting for various reasons, excluding
postburn raw areas. Only thin- to medium-thickness skin grafts were harvested using a
Watson's modified Humby's knife. In 20 patients the graft was harvested by the first
author and in 10 patients by the third author. On all donor sites the proximal half of the
wound was dressed with Micromat (0.5%) and the distal half with paraffin gauze (Fairlie,
Johnson & Johnson). This was done with the idea of providing near perfect similarity
of wound area and depth for comparison. The dressings were overlain with gamgee pads and
bandaged. The inner dressings were left to separate spontaneously by showering on day
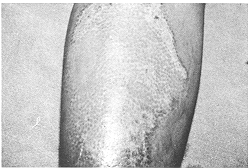
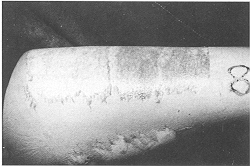
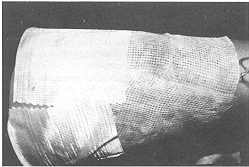
10/11 and a photographic record was maintained (Fig. 3).
Results The patients were assessed for rate and quality of healing, evidence of infection, and pain during change of dressings. The patients were asked to assess pain or discomfort at dressing change as none, mild, moderate, or severe, because the visual analogue method for pain assessment" has proved to be impractical." All patients were followed up till complete healing. The efficacy of viscose polymer as a vehicle for delivering chlorhexidine was also assessed.Partial-thickness burn group The
antimicrobial agent (chlorhexidine gluconate 0.5%) was evaluated in patients with burns in
up to 25% TBSA for the incidence of wound sepsis and septicaemia and for the need to
substitute the local agent or add systemic antibiotic. In six patients with 20% TBSA deep
dermal burns, chlorhexidine gluconate levels were also estimated in blood. The vehicle
(viscose polymer) was assessed in terms of ability to absorb exudate, ease of dressing
change, and required frequency of dressings. There was no evidence of wound sepsis in any
burned area in the trial group or the controls. No patient developed septicaemia, and no
patient therefore needed substitution of the local antimicrobial agent or administration
of systemic antibiotics. Split skin graft donor site group Although it is difficult to quantify pain objectively, especially when the areas compared are contiguous, all patients reported mild and comparable discomfort during dressing removal in both Micromat and paraffin-gauze-treated donor areas, on post-operative day 10 or 11 day, when the dressings were allowed to separate by showering. In all patients both the areas had completely epithelialized, with the same quality of neo-epithelium, at the time of removal of the dressing (Fig. 3).
Micromat, a
chlorhexidine-impregnated viscose dressing, was introduced to us as a new, inexpensive
dressing material for managing partial-thickness skin injury. We decided to evaluate its
place in the dressing armamentarium. Thus, there were two objectives: one, to compare the.
new dressing with traditional, time-tested methods for managing partial thickness skin
injury, and two, to study viscose polymer as a vehicle for delivering chlorhexidine. Split
skin graft donor sites provide an injured area akin to partial-thickness burn. By analogy
the dressing material for both kind of wounds could be similar, with less need of topical
antibacterial agents for donor sites since the donor site wound, in terms of percentage
TBSA, is generally limited. For such donor sites, in Great Britain" and elsewhere,
the most widely used dressing has traditionally been tulle gras overlaid with gamgee and
crepe bandage.
RESUME. Dans cette etude, les Auteurs ont evalue le "Micromat"® 0.5% (un pansement polymere visqueux impregne de chlorhexidine) dans le traitement des brulures d'epaisseur partielle et des sites donneurs de greffe de la peau d'epaisseur variable. Les deux buts de 1'etude etaient de confronter le pansement avec les methodes traditionelles et d'evaluer le polymere visqueux corome vehicule pour livrer la chlorhexidine. Seulement les cas nouveaux de bralures d'epaisseur partielle de 10-25% de la surface corporelle dans des patients ages au moins de 12 ans ont ete inclus dans 1'etude. Les Auteurs presentent leurs methodes et leurs resultats et concluent que pour les types de brnlures pris en consideration le traitement avec le Micromat soutient bien la comparison avec la creme sulphadiazine argentee, et aussi dans le traitement des sites donneurs de greffe de la peau les resultats obtenus avec le Micromat et la gaze commune paraffine sont comparables; le Micromat offre Favantage supplementaire de livrer un agent efficace antibacterien. Les Auteurs ont en outre observe que le polym6re visqueux est un vehicule efficace pour livrer la chlorhexidine. Le partsement Micromat est facile a utiliser et relativement non-adhesif et il possede la capacite d'absorber la suppuration. BIBLIOGRAPHY
|
||||||||||||||||||||||||||||