Annals of Burns and Fire Disasters - vol. XIV - n. 1 - March 2001 EXPERIENCE WITH EARLY TANGENTIAL EXCISION IN THE MANAGEMENT OF DEEP DERMAL BURNS ON THE DORSUM OF THE HAND Fadaak H.A. Division of Plastic Surgery, King Fahd Hospital of the University, AI-Khobar, Saudi Arabia SUMMARY.Thermal injury of the hand deserves special consideration because it affects not only the patients' functional capability but also their long-term rehabilitative potential. The aim of treatment in dorsal hand injury is to restore wound coverage and movement within 14 days of injury, in order to avert sequelae. Early tangential excision and skin grafting coverage on deep dermal burns on the dorsum are predictably successful in restoring function in both the short and the long term. Since 1990 the author has practised this method for treating the burned hand. A total of 27 hands in 19 patients were available for treatment. The age of the patients ranged between 6 and 45 yr, with a male preponderance. Tangential excision and grafting were carried out during the second week post-burn in the majority of patients, mainly because of the severity of burn in terms of body surface area, which necessitated prolonged stabilization. There was partial graft loss in five hands, while none developed infection. All the patients were followed up for at least six, months, and at the end of one year eight hands were available for review. The grafted hands showed excellent recovery of early function and nearly normal appearance and feel; the patients had good compliance with physiotherapy and an early return to work. Introduction Early tangential excision in burn management is now an established practice.` It has opened up better prospects for burn victims in terms of improved survival rates and good cosmetic results. The burned hand represents a special area, where the approach for ideal management is controversial. It remains a challenge to the treating surgeon if both the cosmetic result and full hand function, coupled with an early return to work, are to be achieved. A precise estimate of burn depth, which at times can be difficult, is essential for planning the most appropriate management of the burned hand.' Superficial burns, which heal within two weeks, are nearly always treated conservatively, while full-thickness burns require surgical intervention at the most appropriate time. Controversy remains as regards deep dermal burns and burns of indeterminate depth, particularly in the dorsum of the hand. It has been suggested that hand function is well preserved when burns of uncertain depth are treated expectantly.' Regarding this particular group of deep dermal burn the literature is uncertain as to the ideal approach. The conservative approach, as well as early excision, have both been tried in such cases but the results have not helped to formulate a definite policy. The modality of treatment adopted remains mostly a matter of personal preference. A thermal burn affects the hand through two mechanisms: 1. impaired circulation; and 2. infection. Immediate excision has been claimed to be the best therapeutic measure as far as compromised circulation is concerned. The purpose of this paper is to describe eight years of the author's personal experience in treating deep dermal burns of the dorsum of 27 hands by early tangential excision and immediate split-thickness skin grafting. Patients and methods Between 1990
and 1997, deep dermal burns of the dorsum of 27 hands in 19 patients were seen in this
hospital in Saudi Arabia. Early tangential excision and grafting, performed by the author,
were the preferred method of treatment in all of the patients. In eight patients both
hands were involved. Males (14) outnumbered females (5) and the age varied between 6 and
45 yr. The most extensive associated total body surface area (TBSA) burn was 65%. All
nineteen patients underwent tangential excision of burned tissue and skin grafting. Seven
hands were grafted within the first week, while the remaining 20 were treated in the
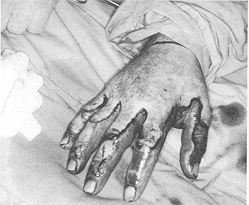
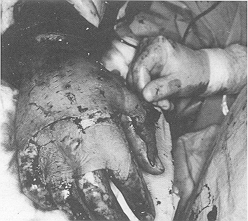
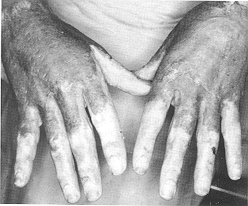
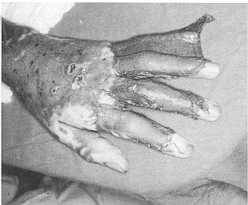
second week post-burn. The procedure was always performed under endotracheal general
anaesthesia, using a tourniquet (Fig. 1). Repetitive slices of necrotic burned tissue were
carefully removed from the dorsum of the hand until viable tissue was reached, when minute
but vigorous bleeding points were seen, which when swabbed revealed a glistening, almost
porcelain-white bed, denoting viability and readiness to accept graft. Before the
tourniquet was released the hand was wrapped in warm saline-soaked sponge dressing, and
pressure was applied for at least ten minutes to stop the bleeding. In the meanwhile the
skin graft was harvested from the thigh. The temporary pressure dressing was released, the
recipient area was irrigated free of clots, and complete haemostasis was ensured before
the sheet graft was applied. The graft was perforated at a number of sites and fixed to
the dorsum with staples. The hand was dressed in a functional position with paraffin
gauze, and a voluminous dressing was applied. The dressing was removed on day 5
post-operation and the graft was inspected for take. Physiotherapy and functional exercise
were initiated only 3-5 days later, after the initial postoperative dressing.
Results In three hands there was
only partial take of the graft because of inadequate excision of the necrotic tissue. A
haematoma collecting beneath the graft accounted for another two incomplete takes. Thus a
total of five hands had an incomplete graft take. There was no infection in the grafted or
donor area. No significant scar contracture preventing functional use of the hand was seen
in this series. In one patient with partial graft take, a hypertrophic scar was observed
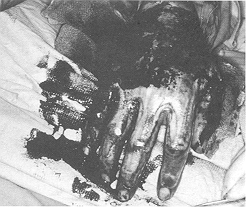
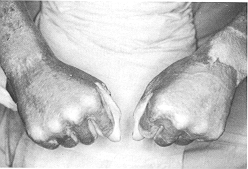
that necessitated excision and re-grafting. Interdigital web space correction by M-plasty
only, without any need of skin graft, was required in four patients late in the follow-up
(Fig. 2).
All the
cases were seen during follow-up six months post-operatively, while only eight
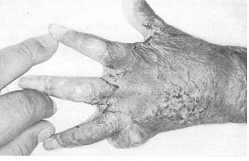
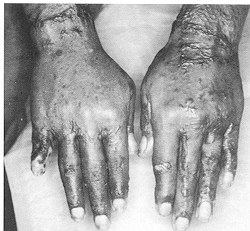
hands were seen and were available for follow-up at the end of one year. The graft was
observed to be soft and supple, and graft elasticity was good. The subcutaneous tissue was
pliable and the hand looked and felt nearly normal (Fig. 3). No tourniquet paralysis was
encountered.
Discussion A total number of 835
cases of burns were seen during a 15-year period in the Burns Unit of our hospital. The
results of treatment were recently analysed, and it was gratifying to note a mortality
rate of only 5.9% 5 Early tangential excision and grafting were liberally practised in our
burn unit wherever indicated, and this contributed to a shorter hospital stay and a lower
mortality rate. While this method of treatment is now well established worldwide in burn
units for body burns, its use in hand burns remains controversial. Burke et al."'
showed that early excision and grafting in hand burn injuries in children shortened
hospitalization and reduced morbidity. There was also an apparent superiority in the
quality of the functional outcome of burned hands so treated. Conversely, Salisbury' and
Labandter,9 in studies comparing excisional therapy with non-operative treatment in
severely burned hands, found no difference in outcome between the two modalities of
treatment when only long-term functional outcome was considered.The principle of early
excision and grafting combined with adequate early physiotherapy and the use of pressure
garments gives favourable results in the treatment of burned hands.'�" The practice
of managing burned hands of deep dermal or indeterminate type in this unit has been in
accordance with the preferences of the treating consultant. Most times these cases were treated conservatively,
especially when the condition of the patient was critical owing to extensive burns. During
this conservative management, delayed unstable healing, blister eruption, and fissuring
were noticed, mainly on the fingers, which delayed rehabilitation and also caused patient
discomfort. When early excision was performed the outcome was different: the results were
better and more acceptable to the patients, healing time was shorter, and there was no
blistering or fissuring on graft-covered areas. The skin graft was applied as a sheet in
all cases, which eliminated the irregularities of mesh graft and gave better cosmetic
results. Early excision of the burn eschar before wound contamination may be a factor in
the prevention of infection, delayed wound healing, and scar formation with its
incapacitating sequelae and non-aesthetic appearance. Levine et al. 12 found that early tangential excision of the
hand in patients with 40% TBSA burns or less had significantly better hand function and
recovery than patients sustaining burns in more than 40% TBSA, and recommended early
tangential excision with skin grafting for deep dermal burns of the hands in all patients
with small to moderate thermal cutaneous injury. However, they cautioned that patients
with life-threatening thermal injuries should be selected for this procedure only after
careful evaluation. Five of the 19 patients in this cohort had more than 40% TBSA burns,
the maximum being 65%. In these five patients the surgical procedure was delayed to the
second week post-burn. These patients' compliance with physiotherapy was unfortunately not
up to the desired level. Also, two patients in this group suffered partial graft loss
owing to haematoma under the graft. The group is however too small to draw any conclusion
regarding timing of excision.
Tangential
excision should always be carried out under a tourniquet. Reluctance to use this
technique, for fear of the difficulty of judging the depth of excision, is not a valid
argument since one can always see the punctuate bleeding spots when viable tissue has been
reached." At the same time the colour of the wound base is clearly visible, providing
further evidence when the excision has reached the desired depth. A Laser Doppler
flowmeter to measure cutaneous microcirculation, in order to provide an immediate result
for early determination of burn depth, has been shown to be an effective and accurate
method of determining burn wound depth." Its availability should encourage surgeons
to adopt tangential excision and grafting as a preferred method of treatment. Acknowledgement. The author would like to thank Prof. Dilip Mitra for his useful editorial suggestions and advice.
RESUME.Les lesions therrniques de la main mdritent une attention particuli6re non settlement parce qu'elles reduisent la capacite fonctionnelle du patient mais aussi a cause des problemes pour ce qui conceme les possibilitds de redducation a long terme. Le traitement des ldsions dorsales de la main se propose d'obtenir la couverture des lesions et la mobilite entre 14 jours apres 1'accident, pour eviter les sequelles. Depuis 1990 1'Auteur utilise la methode qu'il decrit pour traiter les mains brnlees (27 mains dans 19 patients). L'age des patients variait entre 6 et 45 ans, avec une majorite de patients males. L'excision tangentielle et la greffe ont ete effectudes pendant la deuxieme semaine apres la brulure dans la plupart des patients, principalement a cause de la severite de la brulure (surface corporelle totale), qui ndcessitait une stabilisation prolongee. Cinq mains ont subi une perte partielle de la greffe. Aucun cas d'infection n'a ete observe. Tous les patients ont ete suivis pour au moins six mois, et apres un an il dtait possible de rdexaminer huit mains. Les mains greffdes montraient une excellente reprise de la fonction precoce, un aspect et une sensation au contact presque normal, avec un bon rapport vis-a-vis de la physiotherapie et un retour precoce au travail. BIBLIOGRAPHY
|
|||||||||||||||||||||||