Annals of
Burns and Fire Disasters - vol. XIV - n. 1 - March 2001
A COMPARATIVE STUDY OF CEREBRAL OEDEMA
WITH MAGNETIC RESONANCE IMAGING AND PATHOLOGICAL EXAMINATION IN THE EARLY STAGES OF
SEVERELY BURNED DOGS
Li Haitao,* Ying Dajun, Ding
Shiyi, Bian Xiuwu, Yang Zongcheng, Sun Jiansen
The Third Military Medical University,
Chongqing, People's Republic of China" Department of Anatomy
SUMMARY. Fifty-two
dogs were randomized into a control group, a simple burn group (SB), a burn with sodium
lactate group (BSL), and a burn with glucose solution group (BGS). The manifestations of
the dogs in the control group were compared with those in wounded groups in the early
stages (6, 12, 18, and 24 h) after severe burn (50% TBSA III degree) using magnetic
resonance imaging i;MRI) and pathological observation (gross appearance, light microscopy,
and electron microscopy). The earliest finding of brain oedema was seen 12 h after burn in
the BGS group, which exhibited brain swelling as an MRI characteristic. The decrease of
the signal intensity ratio (SIR) on TIW1 was not observed until it was above 10%. SIR on
T2W1 increased by 8.29% (p < 0.05) 24 h post-burn. It was difficult to distinguish grey
matter from white matter at the boundary line, which could not be seen later. Histological
changes of brain oedema were observed as early as 6 h post-burn, accompanied by swelling
of endothelial cells and perivascular astrocytes. Vacuolation look place in neurons 12 h
post-burn, with ischaemic necrosis of varying degree of the capillary endothelium,
neurons, and axons. 'these changes became more marked with the lapse of time. The BGS
group showed the most obvious consequences mentioned above 24 h post-burn. The results
indicated that the model of brain oedema after severe burn had features of both vasogenic
oedema and cellular toxic oedema as regards MRI and pathology.
Introduction
Cerebral oedema
is a major post-burn internal organ complication in burn victims, with a complicated
pathogenesis. The incidence is paralleled to burn severity, but up to now there have not
been many systematic reports on radiological studies of the indices of post-burn cerebral
oedema in the early stages, let alone reports of comparative radiological and pathological
studies. In this study, magnetic resonance imaging (MRI) was therefore employed to conduct
a dynamic observation of morphological changes in cerebral oedema in severely burned dogs
during the early post-burn stage, which were also compared with pathohistological changes
in order to explore the possibility and the reliability of the diagnosis of cerebral
oedema in the early stages after severe burn using MRI and to provide morphological
evidence for the management of post-burn cerebral oedema.
Materials and methods
Animals. Fifty-two
healthy dogs weighing 11.5 ± 1.5 kg were taken as the model. The animals were first
systematically anaesthetized with 3% pentobarbital sodium (30 mg/kg) and then depilated.
The dogs were randomized into a control group (no. 6) and a wounded group (no. 46). The
animals in the wounded group received a 50% TBSA III degree napalm burn injury on the
back. Depending on the different patterns of post-burn management, the wounded dogs were
subdivided into a simple burn group (SB, no. 6), a burn with sodium lactate group (BSL,
no. 20), and a burn with glucose solution group (BGS, no. 20). Dogs in the SB group
received no treatment post-burn. Dogs in the BSL group received sodium lactate solution
based on the Parkland formula at post-burn hour (PBH) 6 at a rate of half the daily amount
in the 2 h between P13H 6 and 8 and the other half in the remaining 16 h. In the BGS
group, animals were resuscitated with 5% glucose solution after P13H 6. Examination. MRI
and pathomorphological examinations were performed in the control group and at P13H 6, 12,
18, and 24 in the wounded groups, respectively.
1. MRI scanning method and image analysis
The type
of MRI employed in this study was 0.2T open style permanent magnets. A spin-echo sequence
with T1WI (TR/TE 560/30 ms) and T2WI (TR/TE 6000/114 ms) was set. The matrix of imaging
was set at 256 x 256 and the field of view at 200 mm. Nine contiguous sections with 4 mm
thick slices were harvested in each sequence. Regular regions (0.3 cm2/ROI) were selected
from both sides of the frontal lobe, the parietal lobe cortices, the basal ganglion, the
cerebellum, and the brain stem areas for image analysis. The mean signal intensity of TIWI
and T2W 1 in ROI from different layers, and the subcutaneous normal soft tissue of the
corresponding layers was measured. The ratio of the above two measurements was set as
standard signal intensity ratio (SIR).
2. Pathomorphological study
a. Gross examination. The
purpose was to observe the colour; distribution, and running patterns of cerebral vessels
and the surface forms of various cerebral tissues.
b. Light microscopy (LM) examination. The harvested brain tissue was fixed in 10% formalin
solution for one week. Samples sized 5 mm3 obtained from both sides of the frontal lobe,,
parietal lobe, cortices, cerebellum cortices, brain stem, and basal ganglion were
gradiently dehydrated with ethanol, embedded with paraffin, sliced, and then stained with
haemotoxylin-eosin.
c. Electron microscopy examination. One cubic mm brain tissue samples were harvested from
both sides of the frontal lobe and the parietal lobe cortices respectively under
anaesthesia and placed in 3% glutaraldehyde for routine fixation for 6 h. The samples were
then dehydrated gradiently with acetone, embedded, sliced, stained, and finally examined
using a transmission electron microscope (EM).
'The ANOVA
statistical analysis and Student's t test were. employed. The data were expressed
as mean ± standard deviation (y ± S).
Results
1. Comparative observation
of brain with MRI and pathomorphology
Control group.
TIWI of MRI scanning revealed a normal-size brain figure and a clear structure of the
cerebral sulci, cracks, cisterns, and ventricles. The TZW1 signal revealed a clear
boundary between grey matter and white matter. Gross and microscopic examination of brain
tissue appeared normal.
Simple burn group. MRI scanning revealed little change at PBH 6. It was shown by LM
that the capillary was slightly dilated and hyperaemic. The pericapillary gaps were
slightly broadened. The neurons exhibited dissolution of the Nissl bodies and
karyopyknosis. EM examination revealed hypertrophy of the capillary endothelia and
swelling of the end foot of the astrocyte.
TIWI in two dogs at PBH 12 indicated shallower cerebral sulci and tracks and slightly
narrower cerebral cisterns and ventricles. T2W 1 showed an obscure boundary between grey
and white matter. Observation of the brain tissue with LM indicated the above lesion
became more obvious than at PBH 6. EM examination showed swelling of the perivascular
astrocyte end foot and cracks in the mitochondrial crista. Gross examination found slight
expansion, congestion, and normal running of external cerebral vessels.
Burn with sodium lactate group. MRI scanning and pathomorphological findings at PBH
6 were similar to those in the SB group. MRI revealed relative normal brain parenchymal
figures, structure, and signals at other time points. At time points later than PBH 12,
examination with LM indicated changes of capillary endothelia and nerve cells similar to
those at PBH 6. In addition to the results observed at PBH 6 with EM, it was found that
part of the basement membrane became thicker and looser. At PBH 24, mitochondrial lysis
and disappearance were observed.
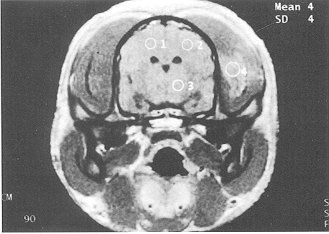
Burn with glucose solution group. The results of MRl scanning and
pathomorphological examination at PBH 6 showed no obvious difference from those in other
groups (Figs. 1, 2).
There were however gradual morphological changes in the brains of two dogs at PBH 12,
three at PBH 18, and four at PBH 24 on MRI scanning. TIWI indicated symmetrical
enlargement of the cerebral parenchyma, flattening and disappearance of cerebral sulci and
cracks, and narrowing and closing of cerebral cisterns and ventricles. T2W 1 showed a mild
diffuse increase in the signals in cerebral parenchyma and partial disappearance of the
boundary between grey and white matter in two dogs at PBH 24 (Figs. 3, 4). It was
found that cerebral endothelia exhibited collapse, defect, and enlargement of partial
interendothelial connective gaps on EM examination. Increased meninx tension, widened
gyri, and shallowed cerebral sulci were noted on gross examination at PBH 18 and 24.
When inspected by LM, the brain white matter exhibited lysis and disappearance, and the
neurons revealed karyopyknosis, etc. On EM the mitochondria of the capillary endothelia
swelled and the mitochondrial crista were fractured and deranged. Swelling of the karyon,
margination of chromatin, capillaries
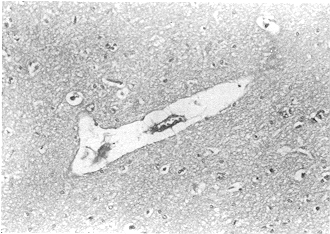
were dilating, tortuous, and hyperaemic. The neurons revealed vacuolization and they
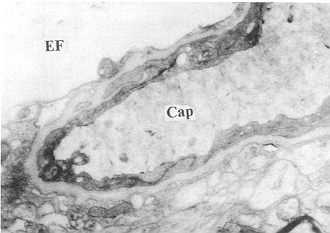
aggravated with the lapse of time on LM examination (Fig. 5). Capillary irregularity of the capillary basement
membrane, and obvious vacuolar swelling of the end foot of the astrocyte were also
observed (Fig. 6).
|
|
Fig. 1 - The cerebral sulci,
cracks, cisterns, and ventricles of the brain appeared normal at PBH 6 in glucose solution
group (Ti-weighted MRI, coronal section). |
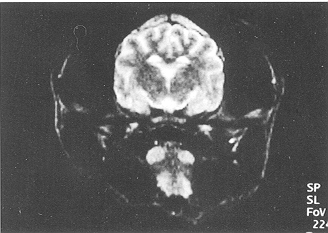
Fig. 2 - The boundary line between grey matter and white
matter appeared clearly, and there was no abnormal cerebral signal at PBH 6 in the glucose
solution group (T2-weighted MRI, coronal section). |
|
|
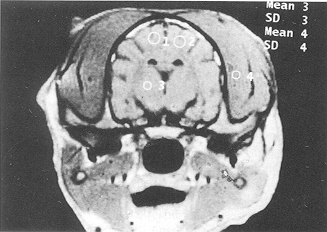
| Fig.
3 - The cerebral sulci and cracks became flat and tended to disappear; the
cerebral cisterns and ventricles were narrowed and blocked at PBH 24 in the glucose
solution group (Ti-weighted MRI, coronal section). |
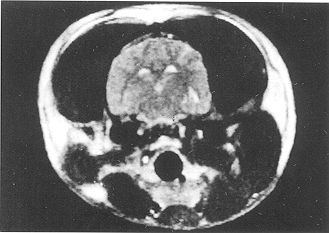
Fig. 4 -
It was difficult to distinguish grey matter from white matter at the boundary line; the
brain signal was not uniform at PBH 24 in the glucose solution group (T2-weighted MRI,
coronal section). |
 |
 |
| Fig.
5 - Evident enlargement of the perivascular gaps and a compressed capillary lumen
were found at PBH 24 in the glucose solution group (LM, HE x 400). |
Fig. 6
- Swelling of mitochondria of capillary endothelia and vacuolation of perivascular end
foot were observed at PBH 24 in the glucose solution group (TEM x 8000). |
|
TIWI SIR decreased by 5.1%, while T2WI SIR increased by 7.39% at PBH 12 in the SB group.
There was no significant change of SIR in the BSL group. However, in the BGS group, TIWI
SIR decreased by 10.39% (p < 0.05), while T2W 1 SIR increased by 8.29% (p < 0.05) at
PBH 24 (Tables I, II).
| |
SB |
BSL |
BGS |
| Control group |
1.627 ± 0.050 |
1.454 ± 0.187 |
1.636 ± 0.096 |
| 6 h |
1.621 ± 0.125 |
1.482 ± 0.113 |
1.657 ± 0.110 |
| 12 h |
1.544 ± 0.114 |
1.468 ± 0.134 |
1.543 ± 0.125 |
| 18 h |
|
1.474 ± 0.089 |
1.482 ± 0.123 |
| 24 h |
|
1.494 ± 0.113 |
1.466 ± 0.154* |
| * p <~ 0.05
versus control group |
|
Table I -
Changes of mean SIR of T1 WI (x ± S) |
|
| |
SB |
BSL |
BGS |
| Control group |
1.447 ± 0.050 |
1.394 ± 0.128 |
1.446 ± 0.161 |
| 6 h |
1.521 ± 0.125 |
1.422 ± 0.121 |
1.457 ± 0.121 |
| 12 h |
1.534±0.114 |
1.411 ±0.140 |
1.460±0.123 |
| 18 h |
|
1.427 ± 0.119 |
1.483 ± 0.115 |
| 24 h |
|
1.436 ± 0.109 |
1.566 ± 0.147* |
| * p <~ 0.05 versus
control group |
|
| Table II - Changes of mean SIR of
T2 WI (x ± S) |
|
Discussion
The
results of this study indicate that after the infusion of a 5% glucose solution based on
the Parkland formula at PBH 6 brain oedema developed in dogs with typical pathological
features and prolongable survival time, which thus provided a reliable and optimal model
of brain oedema in the early stage after severe burn for MRI study. The dogs in this group
revealed brain swelling on MRI examination at PBH 12, which was most evident at PBH 24.
The pathomorphological changes of brain oedema started at PBH 6 and aggravated with the
passing of time, and they were consistent with the MRI scanning results. However, positive
MRI findings were observed after the path omorphological changes. In this study, positive
MRI findings appeared only after PBH 12.
The pathomorphological changes of early post-bum brain oedema possessed characteristics of
both vasogenic and cellulartoxic oedema with similar features in the MRI findings.
Encephalaemia and vasogenic oedema were the main MRI findings in brain tissue before P13H
12. The brain tissue was found to be hyperaemic with increased permeability of the blood
brain barrier, widened capillaries, and perineurocytic gaps at P13H 6. Endothelial cells
and neurons revealed swelling by pathomorphological study after PBH 12. At PBH 24 we
observed attenuated capillary hyperaemia and dilatation, flattened cerebral sulci and
cracks, and increased tension of the meninges.
The results implied that cellulartoxic brain oedema dominated the middle and late period
of the formation of early post-burn brain oedema. Cellulartoxic and vasogenic oedema may
be a common cause of the morphological changes of brain tissue and it may also be the
pathological basis of the aggravation of brain oedema after PBH 12. MRI signal intensity
can be applied to make a quantitative analysis of the changes in brain oedema caused by
trauma, ischaemia and hypoxia, tumour, and cerebritis.
In our experiment, MRI signal intensity of the brain tissue in the early stage post-burn
was analysed quantitatively. The results indicated that the TjWI SIR of brain tissue was
slightly decreased before PBH 18 and manifestly decreased at PBH 24 compared with that of
the control group. T2WI SIR was slightly enhanced in 40% of all the dogs at P13H 24. There
was not so much alteration of MRI SIR at PBH 12 in the SB group, owing to the relatively
short period of observation.
Also, there was no abnormal MRI scanning at P13H 6 in the SL group, owing to the optimal
control of shock. Dynamic observation of MRI SIR in the GS group found that signal
intensity changes could not be detected before a 10% decrease in TIWI SIR, which implied
that the pathomorphological changes in brain oedema had already occurred when TjWI SIR
decrease was detected. It was observed that MRI signal intensity could to some degree
reflect the degree of diffusion of the oedematous fluid of early post-burn brain oedema,
but this was not well correlated with changes in pathomorphology and the trend of MRI
morphological changes.
The changes in MRI signal intensity were related not only to those of brain water content
but also to changes in the dynamic structure of brain tissue water and existing status,
magnetic field strength, proton density, scanning condition, etc. MRI intensity changes
may therefore play a role in reflecting the pathomorphological changes of post-burn brain
oedema, which is a special type of brain oedema.
In conclusion, MRI and pathomorphological comparative studies were employed in the
observation of an animal model (dogs) with brain oedema in the early stage after severe
burn. This may be considered to be a related procedure for the diagnosis and treatment of
post-burn brain oedema, aimed at improving the outcome of brain oedema management after
severe burn.
RESUME. Cinquante-deux chiens ont ete divises en
maniere randomisee dans un groupe t6moin, un groupe de brulures simple lBS), un groupe de
brulures traitees avec le lactate de sodium (BLS), et un groupe de br6lures traitees avec
une solution de glucose i BSG). Les manifestations des chiens dans le groupe temoin ont
ete confrontees avec celles des groupes des animaux br616s dans les premiere phases (6,
12, 18 et 24 h) apres une brnlure severe (50% de la surface corporelle totale de troisieme
degre), avec Vemploi de la resonance magnetique nucl6aire (RMN) et Fobservation
pathologique (aspect grossier, microscope simple, microscope electronique). La premiere
indication d'oedeme c6rebrale se manifestait 12 h apres la br6lure dans le groupe BSG, qui
presentait Fenflure cerebrale comme caracteristique de la RMN. La diminution du rapport de
Fintensite du signal (RIS) sur TIWI n'a pas ete observee avant d'atteindre 10%. Le RIS sur
T2WI augmentait de 8.29% (p < 0,05) a 24 h apres la
bru"lure. 11 etait difficile de distinguer entre la matiere grise et la matiere
blanche a la ligne de delimitations, qui n'etait pas
visible en suite. Les transformations histologiques de 1'oedeme c6r6brale ont ete
observees des la sixieme heure apres la bralure, accompagnees par une enflure des cellules
endovasculaires. Le phenomene de la vacuolation a ete observe dans les neurones a 12 h apres la brulure, comme aussi tme n6crose isch6mique de
degre variable de 1'endothelium capillaire, des neurones et des axones. Ces modifications
devenaient plus marquees dans le temps. Le groupe BSG pr6sentait les consequences les plus
evidentes a 24 h apres la brulure. Les resultats
indiquent que le modele employe d'oedeme cerebrale apres la brulure severe pr6sentait les
caracteristiques de Foedeme vasogenique et de Foedeme celluliaretoxiiique dans 1'examen
RMN et pathologique
BIBLIOGRAPHY
- Li Ao, Yang Zongcheng: Experimental burn surgery. Publishing House of Chongqing
University, 38, 1997.
- Allegrini P.R., Sauer D.: Application of magnetic resonance imaging to the measurement
of neurodegeneration in rat brain: MRI data correlate strongly with histology and
enzymatic analysis. Magn. Reson. Imaging, 10: 773-8, 1992
- Robson M.C., De Beccarc, E.J., Heggers E.J., Loy G.L.: Increasing dermal perfusion after
burning by decreasing thromboxane production. J. Trauma, 20: 722-5, 1980.
- Choi M., Rabb H., Amaout A., Ehrlich H.P.: Preventing the infiltration of leukocytes by
monoclonal antibody blocks the development of progressive ischaerma in rat bums. PRS, 96:
117785, 1995.
- Rother J., De Crepigny A.J., D'Arceuil H.: MR detection of cortical spreading depression
immediately after focal ischaemia in the rat. J. Cereb. Blood Flow Metab., 16: 214-20,
1996.
- Kohno K., Hoehn-Berlage M., Mies G.: Relationship between diffusion-weighted MR images,
cerebral blood flow, and energy state in experimental brain infarction. Magn. Reson.
Imaging, 13: 73-80, 1995.
- Kamman R.L., Go K.G., Berendsen H.J.: Proton-nuclear magnetic resonance relaxation time
in brain oedema. Adv. Neurol., 52: 401-5, 1990
- Lonbinous I., Volk A., Borredon J.: Spreading of vasogenic oedema and cytotoxic oedema
assessed by quantitative diffusion and T2 magnetic resonance imaging. Stroke, 28: 419-27,
1997.
This paper was received on
3 October 2000
Address correspondence to:
Dr Li Haitao,
Department of Anatomy,
The Third Military Medical University,
Chongqing,
People's Republic of China 400038. |
|





