| Annals qf the MBC - vol. 4 - n' 4 - December 1991
TREATMENT OF DONOR SITES OF SKIN GRAFTS OF PARTIAL THICKNESS
WITH HYDROCOLLOID DRESSINGS
Valero J., Comellas M., Alvarez A., Badran J., Vazquez
Barro A., Moledo E.
Burns Unit, Plastic Surgery Service, Juan Canalejo
Hospital, La Coruha, Spain
SUMMARY. In this paper we report
our experience with the use of a hydrocolloid dressing. The healing time that attributed
to classical treatments and comfort and handling were good. The most important drawbacks
we found were the post-operative exudate leak and the bad appearance and smell of the
wound until the site is cleaned. We believe that the dressing tested is useful in treating
the donor sites of skin grafts.
Introduction
Ever since Winter (11) showed in
laboratory animals that occlusive dressing allowed a quicker re-epithelialization rate of
wounds as opposed to drying out by exposure, and Hinman (5) confirmed this finding in
humans, numerous working groups have progressed in the field of the treatment of burns
wounds with occlusive dressings.
Material and methods
The dressing we use is of hydrocollold
type, which keeps the wound covered, is semipermeable to oxygen, a feature of
controversial importance (2), and formed with particles of sodium carboxymethylcel lu
lose, which liquefies when in contact with the wound. It also has some of the properties
attributed to the ideal dressing (3, 9, 10), such as the fact that it does not adhere to
the wound and is impermeable to bacteria, which led us to use it in the trial presented
here. The hydrocolloid dressing is marketed in Spain under the name of Comfeel Ulcus.
Comfeel Ulcus is an elastic sheet, absorbent and self-adhesive on healthy tissue, but not
on wounds. It has a layer of a semipermeable polyurethane film which controls its
permeability to oxygen and to water vapour. Like other hydrocollolds, the dressing keeps
the wound moist in order to enhance reepithelialization (1). It has a minimum thickness
contour to enhance both adhesion and adaptation to the patient's body. It is marketed in
sheets of 6 x 4 em, 10 x 10 cm, 15 x 15 cm and 20 x 20 em.
Forty patients aged from 1 to 85 years were treated with the dressing. Thirty-six of them
had suffered subdermal burns requiring skin grafts for their treatment. Four patients with
loss of skin substance of different aetiology who also required skin grafts were included
in the study. The usual preparation technique consisted of washing the donor sites with
water clorhexidine solution, rinsing with saline, painting with povidone-iodine and a
final application of isopropyl alcohol.
The grafts, about 0.3 and 0.4 mm thick, were taken with a Watson-type manual dermatome.
Deeper donor sites were not included. Once the graft was obtained cotton packs soaked in
saline were placed on the area, sometimes compressed by a temporary elastic bandage, and
were kept this way while the operation was in progress. When this was finished, the saline
packs were removed and the site and the edges of the wound were dried with dry packs. The
dressing was then applied, avoiding the dead spaces and extending it 2 to 3 cm beyond the
edges of the wound. A slightly compressive bandage was then applied on top.
The dressing was removed after 48 hours, when exudate leakage was observed, and a culture
was taken occasionally with a swab. The site was cleaned by irrigation with saline in
order to eliminate as much haematoma and debris as possible. Rubbing and scratching of the
wounds were strictly avoided. After the area had been thoroughly dried, leaving just
traces of haematoma and liquefied dressing still in the wound, a new hydrocollold was
applied.
A follow-up was made on day 6, and after that every 48 hours when necessary. Photographs
were taken during the operation, two days later if exudate leakage was observed, and six
days later in all conditions.
According to Gruber's criteria (4), the patient was considered to be cured when the wound
was pink on the surface and there were no scabs.
Results
Population treated.. the distribution and
characteristics of the 40 cases are shown in Tables I, II and III,
| Variable |
Burns |
Non Burns |
| Total number of cases |
36 |
4 |
| Number of male patients |
20 |
2 |
| Number of female patients |
16 |
2 |
|
Table I Treated
population |
|
| Parameter |
Value |
| Total protein (mean) |
6.02 gm% |
| Total protein (range) |
3.8 - 7.8 gm% |
| Haematocrit (mean) |
40% |
| Haematocrit (range) |
32 - 66.5% |
| Haemoglobin (mean) |
13.87 gm% |
| Haemoglobin (range) |
11.3 - 22.2 gm% |
|
Table II Laboratory
values in burned patients |
|
| Extent TBSA (mean) |
11.58% |
| Extent TBSA (range) |
0.5 - 50% |
|
Table III Burned
area |
|
Healing time.. The average time was
8.45 days, with a range of 6 to 20 days in burn patients and 6 to 10 days in non-burn
patients (the average healing time for patients with burns was 8.44 days and 8.5 for those
without burns).
Pain and itching.. Mild pain was
reported by patients when the dressing was removed, due to its adherence to healthy
tissue, but not to the wound, and immediately after operation. Three patients reported
some itching in the areas treated. It was not necessary to discontinue treatment for
either of these two reasons, and post-operative pain was usually controlled with
paracetamol alone or with codeine.
Infection: Cultures taken with
swabs often gave a positive result for Staphylococcus aureus, although no clinical
signs of infection were detected.
Quality oj' scars: Although the
time since the beginning of the trial is not sufficient to make a conclusive assessment,
we can say that the areas treated have so far an excellent appearance and no keloids have
appeared. In the immediate period, there was erythema in the treated areas, but this
disappeared spontaneously.
 |
 |
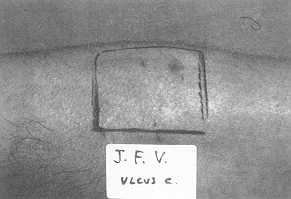
| Fig. 1a Premarked
donor area |
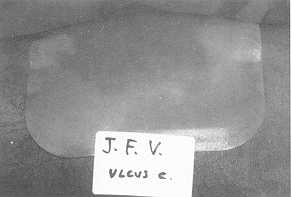
Fig. 1b Intraoperative
appearance of the dressing |
|
Comfort.. The patients were asked
to assess the comfort of the dressing between a maximum of 4 and a minimum of zero. The
average score was 3.25, with limits of 4 and 2.
Nursing staffs assessment qf use: The
nurses involved in the study assessed the dressing's convenience for use between a maximum
of 4 and a minimum of zero, and a score of 4 was given in every case. It must be
remembered that before the dressing was introduced, the donor sites were treated according
to the classical methods. The greatest problem for nurses was the appearance and smell of
exudate, and the leakage in the early post-operative period that was seen in some cases.
 |
 |
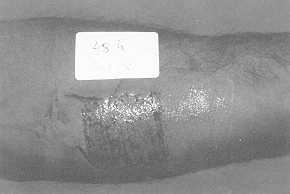
| Fig.
2 Two days later |
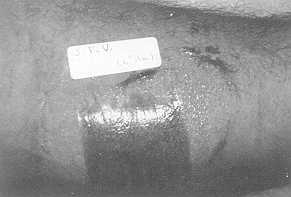
Fig. 3 Six
days later. Complete epithclialization of the donor site |
|
Discussion
The study reported here demonstrates
the positive effect of the hydrocollold dressing on the treatment of skin graft donor
sites, although the influence of factors such as the burn and concomitant illnesses has
not been established in this paper.
The healing time was significantly shorter than that attributed to classical treatments in
reports by other authors (6, 7). The discomfort attributed to the dressing was less than
with classical therapy, since it does not adhere to the wound. Patients rated the pain as
mild, and indicated that it appeared immediately after operation. At the change of
dressing, they reported some pain in the surrounding area, where the dressing adheres. In
our opinion, the patients' complaint of itching is more significant, although this did not
require treatment or suspension of treatment.
As far as the assessment of the comfort of the dressing is concerned, we think that the
cosmetic appearance of the dressing plays an important part, as does the possibility of
early mobility in the majority of cases and the fact that it facilitates personal hygiene.
The nursing staff showed their undoubted approval of the dressing, which is a clear
indication of its convenient handling.
Probably the key factor for its acceptance was the fact that less time is spent on care
with this method.
The most important drawbacks we found were:
- The exudate leak which occurs occasionally in the immediate
post-operative period, although we have seen that it does not delay healing or lead to a
premature worsening of the quality of the scar. This is a common problem with other
dressings of the same type, and we think it could be solved by making small holes in the
sheet, as recommended by Neffi et al. (8), in order to evacuate the haematomas which
appear when the dressing is first placed.
- The bad appearance and smell of wound, once the dressing is
removed; this is just temporary until the site is cleaned. In short, we believe that the
dressing tested has suflicient advantages and few drawbacks, and it can therefore be
recommended for routine use in treating skin graft donor sites.
RÉSUMÉ. Nous décrivons dans cet article
nos expériences avec l'emploi d'un pansement hydrocolloïdal. Le temps de guérison est
significativement plus bref par comparaison avec les traitements classiques; en outre le
confort et la facilité d'emploi étaient bons. Les désavantages les plus importants
étaient les pertes postopératoires d'exsudat et le mauvais aspect et l'odeur de la plaie
jusqu'à ce que le site soit nettoyé. A notre avis le pansement que nous avons testé est
utile pour le traitement des sites donneurs de greffe cutanée.
BIBLIOGRAPHY
- Alvarez O.M.: Moist enviroment for healing: matching
the dressing to the wound. Symposium on Advance Wound Care, 1988.
- Alvarez O.M., Mertz P.M., Eaglestein W.H.: The
effect of occlusive dressings on collagen synthesis and reepithelialization in superficial
wounds. J. Surg. Res., 35: 142-148, 1983.
- Brown A.S., Barot L.R.: Biologic dressings and skin
substitutes. Clin. Plast. Surg., 13: 69-74, 1986.
- Gruber R.P., Vistnes L., Pardoe R.: The effect of
commonly used antiseptics on wound healing. Plast. Reconst. Surg., 55: 472-476, 1975.
- Hinman C.D., Maibach H.: Effect of air exposure and
occlusion on experimental human skin wounds. Nature.
- Jonkman M.F., Bruin P., Permings A.J. et al.:
Polyetherurethane wound covering with high water vapour permeability compared with
conventional tulle gras on split-skin donor sites. Burns, 15: 2 11-2 16, 1989.
- Madden M.R., Finkelstein J.L., Hefton J.M. et al.:
Optimal healing of donor site wounds with hydrocolloid dressings, and environment for
healing: the role of occlusion. The Royal Society of Medicine, 88, 1985.
- Nefzi A., Kirch J.M., Baux S.: Traitement des sites
donneurs de greffe par un pansement a base de Carboxym6thylcellulose soclique. Ann. Chit.
Plast. Esth&t., 33: 102-104, 1989.
- Queen D., Evans J.H., Gaylor J.D.S. et al.:
Preclinical assessment of burn wound dressings. Burns, 12: 16 1-166, 1986.
- Tavies M.J., Thornton JW., Danet et al.: Current
status of skin substitutes. Surg. Clin. North. Am., 58: 1233-1248, 1978.
- Winters G.D.: Formation of scab and rate of
epithelialization of superficial wounds in the skin of the young domestic pig. Nature,
193: 293-294, 1962.
|



