Annals of'the MBC - vol. 5 - n' 4 -
December 1992
SMALL-SIZED
FULL-THICKNESS BURNS TREATED WITH A HYDROCOLLOID DRESSING (VARIHESIVE GEL CONTROL)
Serna C., Terren J., Pous S., Hidalgo J.C., Mallent J.,
Frances J., Mirabet V.
Plastic Surgery and Burns Centre Department, La Fe
University Hospital, Valencia, Spain
SUMMARY The aim of this study was to
ascertain the effect of the hydrocolloid dressing Varihesive Gel Control on the healing of
full-thickness burns with a maximum diameter of 4 cm, in order to investigate alternatives
to treatment by split-skin autograft Or even, in some cases, direct closure of the wound.
Twenty out-patients with small full-thickness burns were treated with the hydrocolloid
dressing and were periodically checked to evaluate epithelialization. It was found that
this dressing helped complete healing in some cases and in others reduced the size of the
wound, giving the wound bed the correct properties for receiving a graft.
Introduction
Throughout the history of burn treatment different types of dressings have been used (3).
They have been made from natural or synthetic materials (with or without pharmacological
agents); there are also biological dressings and even artificial skin. The purpose
of using them is to protect the burn from outside agents which might impair the wound's
condition, to prevent pain as far as possible, to absorb the exudate, to act a barrier
against infection, to facilitate debridement of sloughs and eschars, and even to promote
epithelialization (1, 2). It has been proved that by occluding the wound a very favourable
environment is created for a new epithelium to form more quickly (6). This discovery has
brought forward a hydrocolloid dressing (Varihesive Gel Control) which has properties that
facilitate burn wound healing.
Material and methods
Material
The composition of Varihesive Gel Control is described in Table 1. It is commercially
available in three different sizes. The outer surface is impermeable to water, gases,
vapours and organisms; this characteristic permits the creation of a humid medium in the
wound (4). The constituents of the dressing form a gel when they come into contact with
the wound exudate, which facilitates its removal without damage to the newly formed
tissues. Twenty patients were selected, 12 females and 8 males. Their ages varied from 16
months to 68 years. All the burns involved were of full skin thickness, and their maximum
diameter was equal to or less than 4 cm.
Table 1 Composition of dressing
- Outer layer of polyurethane.
- Inner matrix formed by polymers, which include three
hydroactive or hydrocolloidal substances: sodium, carboxymethylcellulose, pectin and
gelatine.
The aetiology of the burns was varied
(scaldsI fire, solid contact) but no electrical burns were included, since their evolution
is erratic and different from that of other burns. In 2 patients the bums were on the
chest, in another 2 on the back, in 6 on the upper limb, in 3 on the abdomen and in 7 on
the lower limb.
Methods
All of the patients selected were treated in the Out-patients Department of the Burns
Unit, at La Fe University Hospital. The application of the Varihesive Gel Control dressing
was carried out as follows:
- cleansing of the wound with soapy water or saline;
- application of the dressing after removal of moisture from
the area;
- change of dressing every 5 days (5), checking the condition
of the wound bed, the edges and the size of the wound (measuring maximum and minimum
diameter and calculating the area as for an ellipse);
- recording any complications (infection, exudate leaks,
pain).
The trial was considered completed when in two successive
dressings the size of the burn had not changed, or when epithelialization was complete.
Results
The 20 patients were examined as out-patients and none of the courses of treatment was
discontinued for reasons other than the criteria of study completion. All of the burns
involved full skill thickness and their maximum diameter was no larger than 4 cm. 1. In
all 20 cases, Varihesive Gel Control facilitated the formation of clean granulation
tissue, which afforded an ideal bed for a split-skin graft.
 |
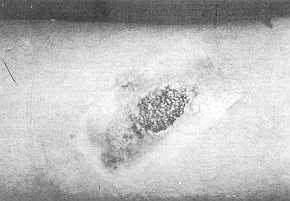 |
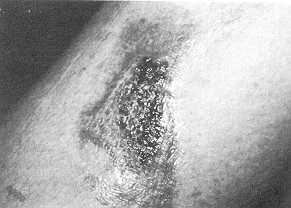
Fig. 1
35-year-old woman with scald burn on left lower limb.
1 a) Appearance of the burn on first day of trial. Size: 2.5 x 1.5
cm. |
1 b) Wound
after 15 days: size of bum markedly reduced. |
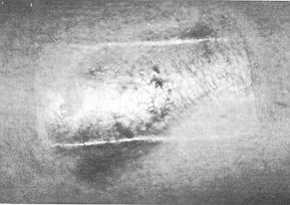 |
1 c)
After 23 days burn completely epithelialized. |
|
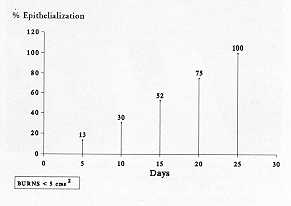 |
Table 2 Mean
epithelialization percentages |
|
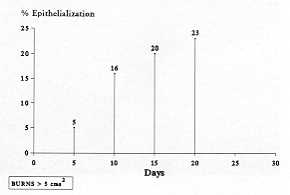 |
Table 3 Mean
epithelialization percentages |
|
2. Complete wound closure occurred in 4
cases, where the burns had a surface area less than 5-CM2. The mean healing time in these
cases was 24.5 days (Fig. la, b, c). The mean epithelialization percentage observed during
out-patient treatment is shown in Table 2.
3. In the remaining 16 cases, hypertrophic granulation tissue occurred, which impeded
complete epithelialization of the wounds, so that in the following two dressings there was
no change in size. All of these burns had a surface area larger than 5 CM2. The mean
epithelialization percentage in these 16 cases is shown in Table 3.
Within 14 to 21 days (average 17.5 days) after starting the use of Varihesive Gel Control,
this treatment was discontinued and definitive therapy was achieved, with split-skin
grafts (14 cases) or direct closure of the wound (2 cases) (Fig. 2a, b, c).
 |
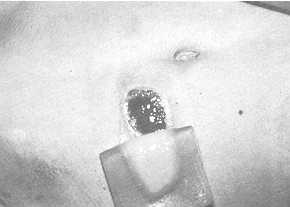 |
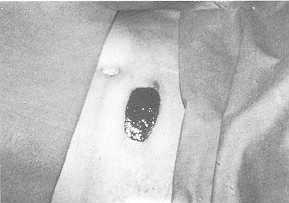
Fig. 2 12-year-old
boy with fire burn on abdomen.
2 a) Burn on first day of trial. Size: 3.5 x 2 em. |
2 b)
Appearance of the burn after 10 days. |
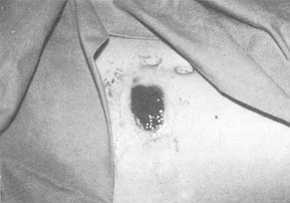 |
2 c)
After 15 days size of wound is unchanged. |
|
4. All of the patients involved in the
trial accepted the dressing, because of its comfort, large bandages not being required,
and because its removal was painless. There was no haematoma collection under the
dressing. No infection occurred. In three burns where the wound beds contained fibrin
stretches and small amounts of slough, serous exudate was found during the first
inspection, a result of the debridement effect claimed for the dressing (4).
Discussion
Our purpose was to ascertain whether the hydrocollold dressing Varihesive Gel Control can
be used in the treatment of small full-thickness burns.
It, is true, that skin autografts are..an excellent therapy; in small areas they can be
performed with a local anaesthetic, the graft takes in a few days (5-7 days), and the
healing period is short. The result is also aesthetically acceptable. However, it must be
emphasized that this means two bloody areas which have to heal (the donor site and the
receiving site), and sometimes the graft does not take.
Moreover, some of these burns can be treated by direct closure when the patient initially
consults the doctor. This requires local anaesthesia, and the result is a healing by first
intention (which is always aesthetically preferable to healing due to closure by second
intention), although not all small burns can be treated in this way.
We did not intend to show with this trial that treatment with Varihesive Gel Control is
better than the other two possibilities mentioned above: our purpose was to provide
another valid alternative which avoids surgery and is comfortable and not painful for the
patient, and which does not involve a prolonged healing period. Our result, 24.5 days on
average, is better than that of Hermans' series (5) with a mean epithelialization time of
29.5 days for this type of bum.
RESUME Cette recherche vise
a vérifier Peffet du pansement hydrocollo'fdal Variliesive Gel Control sur la
cicatrisation des brélures A toute &paisseur avec un diam&re maximum de 4 cm,
dans le but d'&tudier des alternatives au traitement moyermant l'autogreffe A
épaisseur variable ou rn~me, clans certains cas, la fermeture directe de ]a plaie. Vingt
malades en consultation externe atteints de petites brélures ~ toute épaisseur ont W
traités avec le pansement hydrocolloYdal et controllés périodiquement pour évaluer
1'épithélialisation. Les auteurs ont trouvé que le pansement Varihesive Gel Control a
contribué d la cicatrisation compl~te ou bien il a réduit la superficie de la plaie,
tout en créant les conditions les plus appropriées pour la greffe.
BIBLIOGRAPHY
- Alvarez O.M., Mertz P.M., Eaglstein W.H.: The effect of
occlusive dressings on collagen synthesis and re-epithelialization in superficial wounds.
J. Surg. Res. 35: 142-48, 1983.
- Baxter C.: Homografts and heterografts as a biological
dressing in the treatment of thermal injury. First Annual Meeting Society German Plastic
Surgeons, Munich, 1970.
- Boswick J.A. et al.: "The art and science of burn
care", 53-56. Aspen, Rockville (Maryland), 1987.
- Convatec, Squibb: Duoderm hydro-active dressings. Technical
Booklet, 1983.
- Hermans M.H.E.: Hydrocolloid dressing (Duoderm) for the
treatment of superficial and deep partial thickness burns. Scand. J. Plast. Reconstr.
Surg., 21: 283-285, 1987.
- Lawrence J.C.: The physical properties of a new
hydrocolloid dressing. An Environment for Healing Symposium, Royal Society of Medicine
Congress & Symposium, series 88: 69-76, 1985.
|







