| Annals of Burns and Fire Disasters - vol. IX - n. 1 - March 1996
SERUM CYTOKINES FOLLOWING THERMAL INJURY
Shehab El-Din S.A.,(1) Aref S.,(2) Salama O.S.,(2) Shouman
O.M.(1)
Plastic, Reconstructive and Burn Unit(1) and Haematology
Unit(2), Mansoura University Hospitals, Faculty of Medicine, Mansoura, Egypt
SUMMARY. Serum levels of
interleukin- 16 (IL- 1ß), interleukin-6 (IL-6) and tumour necrosis factor-a (TNF-a) were assayed in 31 bum
patients and 12 controls. A study was made of the correlation between cytokine levels and
time post-burn, burn area, and mortality. The early IL-1ß, IL-6 and TNF-a systemic responses following
thermal injury decreased with time post-burn but did not reach control levels. With
increased burn area a significant elevation of IL-6 and TNF-a, but not of IL-1ß, was
detected in the systemic circulation. All non-surviving burn patients had detectable
levels of IL-1ß, IL-6 and TNF-oc; these were significantly higher than those of surviving
patients. The results suggest that IL-1ß, IL-6 and TNF-a may play a role in the pathogenesis of septic shock or
multiple organ failure and are therefore to be considered bad clinical omens.
Introduction
Infection is the primary or major
contributory cause in 75% of deaths from thermal injury. Thermal injury induces a
dose-related suppression of the immune response which correlates significantly with the
survival of the patient? Cytokines modulate a number of immunological functions following
thermal injury and may influence the resistance of burn patients to infection.
Interleukin-I (IL-1) displays multiple biological activities of which activation of
T-lymphocytes is one of the first. IL-1 serves to increase the adherence of neutrophils
and lymphocytes to the endothelial cells. This is due to an increase in adhesion molecules
on both the neutrophils and the endothelial cells. IL-1 also has the ability to induce
fever. In addition to elevating serum copper and depressing serum zinc and iron
concentrations, IL-I also causes the synthesis of hepatic acute phase proteins and induces
production of interleukin-6 (IL-6).11 IL-1 causes neutrophilia by inducing colony
stimulating factors, and it has been implicated in the pathogenesis of various diseases;
septic shock and sepsis syndrome, rheumatoid arthritis, inflammatory bowel
disease, and leukaemia.
Several biological activities have been ascribed to IL6. It is thought to play a
protective role in inflammation. This is done by stimulating the host defence mechanisms
to limit the injury (synthesis of hepatic acute-phase proteins) and to augment the
clearance of pathogens (increased immumoglobulin production by the induction of maturation
of B-cells to plasma cells). IL-6 possesses the additional property of inhibiting TNF
production in vitro and in vivo and of decreasiing acute inflammation. IL-6
induces the formation of multipotential hernatopoictic colonies. The injection of
recombinant IL-6 can cause fever.
Tumour necrosis factor (TNF) performs numerous biological activities, many of which
overlap with those of IL- 1. It can induce the synthesis of other cytokines, including
IL-6 and IL-8 Endothelial cells may be altered by TNF to assume a procoagulant profile 26
and increase adherence for inflammatory cells. TNF plays a role in transplantations, lysis
of tumour cells 21 cachexiall and septic shock. It also suppresses lipoprotein lipase
activity and stimulates lipolysis.
The aim of this study was to evaluate serum cytokine concentrations (IL-Iß, IL-6 and TNF-a) in patients with thermal injury and
their relationship with clinical outcome.
Patients and methods
The patients
Over an eight-month period (October 1994 - May 1995) 31 burn patients (14 male and 17
female; mean age 26.3 years; mean burn size 44.2% TBSA) were evaluated in a prospective
randomized fashion for serum IL-1ß, IL-6 and TNF. The patients, normotensive and
haemodynamically stable after uneventful resuscitation, were divided into three groups
according to the percentage TBSA burned: Group 1 (0-25%), Group 11 (26.50%) and Group III
(51-100%). There were 19 survivors and 12 non-survivors. The characteristics of the
patients are shown in Table I.
| |
No. |
Sex |
Mean age
(yr) |
Mean burn
size
(% TBSA) |
| M |
F |
| Whole group |
31 |
14 |
17 |
26.3±12
(range: 9-63) |
44.2±23.0
(range: 10-95) |
| Group 1 |
9 |
5 |
4 |
23.2 ± 11.3
(range: 9-37) |
21.1 ± 5.5
(range: 10-25) |
| Group II |
15 |
8 |
7 |
27.7 ± 13.9
(range: 9-63) |
42.0+7.7
(range: 30-50) |
| Group III |
7 |
1 |
6 |
28.4 ± 9.5
(range:18-45) |
78.6 ± 17.5
(range:60-95) |
| Survivors |
19 |
12 |
7 |
24.2 ± 8.7
(range: 9-40) |
31.3 ± 11.3
(range: 10-50) |
| Non-Survivors |
12 |
2 |
10 |
29.6 ± 15.8
(range: 9-63) |
64.6 ± 22.0
(range: 25-95) |
|
Table I -
Patient population |
|
Collection and processing of specimens
Peripheral blood samples (5 cc) were collected from each patient on admission, in the
second and third weeks post-bum and after complete healing, either spontaneously or after
surgical excision and skin grafting. The blood was drawn between 5.00 and 6.00 a.m. into
blood collection tubes. The specimens were centrifuged at 750 g for 20 minutes, and the
serum was removed and stored in aliquots at -70 °C until assay. Serum IL-1ß
concentrations were measured in 81 samples from all 31 patients. Serum IL-6 concentrations
were measured in 75 samples from the 31 patients. Serum TFN-a concentrations were measured in 83 samples from 31 patients.
Twelve serum samples from 12 healthy laboratory persons were used as controls.
Assay procedure
The cytokines were detected by enzyme-linked immunosorbent assay (ELISA). The IL-1ß, IL-6
and TFN-a ELISA kits were
obtained from Medgenix Diagnostics SA, B-6220 Fleurus, Belgium.
* Principle of the test
Medgenix IL-1ß, IL-6 or TFN-a is an enzyme-amplified sensitivity immunoassay (EASIA) performed
on a microtitre plate. It is based on the oligoclonal system in which several monoclonal
antibodies (Mabs) directed against distinct epitopes of IL-1ß, IL-6 or TFN-a are used. The use of several distinct
Mabs avoids hyperspecificity and allows highly sensitive assays with extended standard
range and short incubation time. The assay is performed directly on serum, plasma or
culture media samples, without any treatment or extraction. Mabs I - the capture
antibodies - are attached to the lower and inner surface of the plastic well. Standards or
samples are added to the well. After incubation, washing removes the occasional excess of
antigen. Mabs 2-HRP (horseradish peroxidase) labelled antibody is added. After an
incubation period, to allow the formation of a sandwich, and washing, the microtitre plate
is washed to remove unbound enzyme-labelled antibodies. Th~ revelation solution
tetramethylbenzidine (TMB) - (H2 2) is added and incubated. The reaction is stopped with
H2SO4 and the microtitre plate is read at the appropriate wavelength. ermined coloriich is
proportiorations. A standard curve is plotted and the cytokine concentrations in the
samples are determined by interpolati~n from the standard curve.
Statistical Design
Data were collected, tabulated and statistically analysed
using chi-square for comparison of frequency of occurrence and Z-test for comparison
percentages. The difference is considered significant if P <0.05.
Results
Serum cytokines following thermal
injury at presentation
Of the serum samples taken from b admission, 89.7%, 64.5% and 32.1% con amounts
resnectivelv of IL-Iß IL-6 and burn patients on ained detectable TNF-a. The percentage of samples with
detectable amounts of IL-1ß and IL-6 was significantly higher in the burn patients than
in controls (P <0.001 and <0.01 respectively) (Table II).
| |
Controls |
Bum patients |
P |
| IL-1ß |
25.0% (3/12) |
89.7% (26/25) |
<0.001 |
| IL-6 |
25.0% (3/12) |
64.5 % (20/3 l) |
<0.01 |
| TNF-a |
16.7% (2/12) |
32.1% (9/28) |
>0.05 |
|
| Table II - Percentage of detectable
serum cytckines measured by ELISA in burn patients on admission and in 12 healthy
laboratory persons (controls) (actual numbers in parentheses) |
|
Serum cytokines and time post-burn
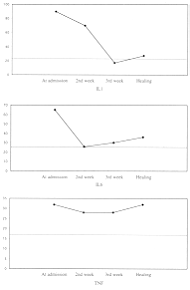
Fig. 1 shows the percentage of patient samples containing detectable amounts of
cytokines irl the first three weeks post-burn. Patient serum samples c ntained detectable
levels of IL-1ß, decreasing from 89.7ck d ri h fi week post-burn to 68.2% during the sec
18.2% during the third week. This was stat cant (P <0.001). IL-6 was detectable in
64.5% serum samples during the first week post-b to 26.7 % during the second week and
risir g the third week. This was statistically signifi TNF in patient samples during the
first, u ng c e rst ond week and istically signifi4.5% of patient urn, decreasing to 30%
during cant (P <0.05). week post-burn was 32.1%, decreasing to 27.8% during both the
second and the third weeks. This was statistically non-significant (P >0.05).
|
Fig. 1
- Seturn cytokines in burn patients and time post-burn (weeks). |
|
Serum cytokines and burn size
The relationship between cytokine
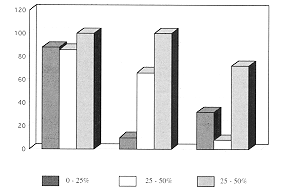
levels and the percentage of TBSA burned was examined (Table III). Fig. 2 shows
that the percentage of patients with positive IL-6 and TNF-a levels increased with increasing burn size (P <0.001 and
<0.05 respectively). There was no apparent relationship between bum size and positive
IL-113 patient samples.
| |
Group I
(0-25%) |
Group II
(26-50%) |
Group III
(51-100%) |
P |
| IL-1B |
87.5%(7/8) |
85.7% (12/14) |
100% (17/17) |
>0.05 |
| IL-6 |
11.1%(1/9) |
66.7% (10/15) |
100% (7/7) |
<0.001 |
| TNF-a |
33.3% (3/9) |
8.3%(1/12) |
71.42% (5/7) |
<0.05 |
|
Table III -
Percentages of detectable serum cytokines measured by ELISA in surviving and non-surviving
burn patients grouped by bum size on admission (actual numbers in parentheses) |
|
|
Fig. 2 -
Scrum cytokines in burn patients and TBSA burn. Cytokine values were grouped by burn size
as displayed. Bars represent percentage of sample with detectable levels of cytokines. |
|
Serum cytokines and mortality
Table IV shows'that 83.3%, 36.8% and
17.6% of serum samples from the 191~surviving burn patients contained detectable amounts
respectively of IL-1ß, IL-6 and TNF-a. Serum samples from the 12 non-surviving burn patients contained
detectable amounts of IL-18 (100%), IL-6 (91.7%) and TNF-a (54.5%), which were significantly higher than in the surviving
burn patients (P <0.05, <0.01 and <0.05 respectively).
|
Survivors |
Non-survivors |
P |
| IL-1ß |
83.3% (15/18) |
100% (11/11) |
<0,05 |
| IL-6 |
36.8% (7/19) |
91.7% (11/12) |
<0.01 |
| TNF-a |
17.6% (3/17) |
54.5% (5/11) |
<0.05 |
|
| Table IV - Percentages
of detectable serum cytokines measured by ELISA in surviving and non-surviving burn
patients on admission (actual numbers in parentheses) |
|
Serum cytokines and healing
The relationship between cytokine
levels on admission and after complete healing of the burn patients, either spontaneously
or after surgical excision and skin autografting, was examined (Table V). Percentages
of detectable serum IL-1ß levels show a highly significant decrease from admission to
healing, while the percentage of detectable IL-6 and TNF-a levels shows a non-significant decrease.
|
Admission |
Healing |
P |
| IL-1ß |
29.6% (26/29) |
23.3% (5119) |
<0.001 |
| IL-6 |
64.5% (20/31) |
47.4% (7/19) |
>0.05 |
| TNF-a |
32.1% (9/28) |
31.6% (6/19) |
>0,05 |
|
| Table V - Comparison between percentages of
detectable serum cytokines measured by ELISA on admission and after complete healing |
|
Discussion
Interleukin-Iß, interleukin-6 and
tumour necrosis factor-a
are proinflammatory cytokines. Their role in thermal injury has been the objective of
considerable researchl.Drost et al. reported that serum ILA activity is increased in
burned rats compared with controls. Drost et al . showed increased plasma IL-1ß and IL-6
concentrations following thermal injury, while TNF-a was increased only in a subpopulation of patients .3 Our study
found that acute thermal injury initiates an early IL-1ß, IL-6 and TNF-a systemic response. This may account,
at least in part, for some of the physiological responses characteristically seen after
injury, e.g. fever without infection, muscle wasting associated with negative nitrogen
balance, and an acute phase response accompanied by attendant elevations in certain serum
proteins and decreases in albumin and transferrin.
In this study, serum IL-1ß and IL-6 decreased in relation to time post-bum but did not
reach the control level. This may coincide with the decrease in hypermetabolism, the
return to normal hormone levels and the positive nitrogen balance occurring after the
third week post-bum.
The initial elevation of cytokines observed in this study is consistent with the findings
of Rodriguez et al., who reported that acute thermal injury initiates an early systemic,
lung and skin response involving TNF, ILß and IL-8, which are generated locally and do
not originate from the systemic cytokine pool. Kupper et al.11 also reported that the
human bum wound is a primary source of IL-1 activity. On the basis of these findings, we
would suggest that the initial elevation of cytokines in bum cases is of both systemic and
local origin and that other events besides burn severity induce their production.
This study found a statistically significant positive correlation between bum size and the
levels of both serum IL-6 and TNF-u.. IL-1ß did not show this correlation. This is in
contrast with the results of Drost et al.,1 who observed a relation between increasing
burn size and increased levels of IL-1ß levels, but not of IL-6 or TNF-a. Our findings are consistent with
those of Schluter et al.,11 who reported an increased IL-6 production as a potential
mediator of lethal sepsis after major thermal trauma. Marano et al." reported no
correlation between TNF-(x and burn size.
However, in our study, we found a statistically significant correlation between mortality
and serum cytokine IL-1ß, IL-6 and TNF-a. The highest incidence of mortality was in group 111 (100%), which
presented a high percentage of TBSA burn, a high percentage of third-degree burn,
inhalation injury, and a high incidence of septic episodes. Rodriguez et al.11 reported no
association between mortality or local organ infection and TNF, IL-6 and IL-8. Hack et
al.11 and Drost et al. found a relationship between IL-6 and mortality. Marano et al.11
reported a relationship between TNF-a and mortality. Several other reports correlated mortality with
TNF, IL-6 and IL-8 systemic production. In the light of our study, we can postulate that
serum cytokines play a role in multiple organ failure and septic shock. We therefore
conclude that cytokine elevation may be a bad clinical omen.
RESUME. Après
avoir essayé les niveaux sériques d'interleukine- 1 B (IL-1ß), d'interleukine-6 (IL-6)
et du facteur de nécrose tumorale-a (TNF-a) dans 31 patients brûlés et 12 témoins, les auteurs ont
corrélé les niveaux des cytokines avec le temps post-brûlure, l'extension de la
brûlure, et la mortalité. A la suite des lésions thermales les réponses systémiques
précoces de l'IL-1ß, IL-6 et TNF-a diminuaient en fonction du temps mais n'arrivaient pas aux niveaux
des témoins. Avec une extension augmentée de la brûlure, des niveaux élevés l'IL-6 et
de TNF-a, mais non
d'IL-1ß, ont été observés dans la circulation systémique. Tous les patients non
survécus présentaient des niveaux appréciables d'IL-1ß, d'IL-6 et de TNF-oc qui
étaient supérieurs aux valeurs observées dans les patients survécus. Les auteurs
concluent que l'IL- 1ß, l'IL-6 et le TNF-a peuvent jouer un rôle dans la pathogenèse du choc septique ou de
l'insuffisance organique multiple et qu'il faut donc les considérer des présages
cliniques néfastes.
BIBLIOGRAPHY
- Polk H.C.: Consensus summary on infection. J. Trauma, 19:
894, 5.1979.
- Munster A.M.: Immunologic alterations following injury.
Adv. Orthopaed. Surg.: 328, 1985.
- Drost A.C., Burleson D.G., Cioffi W.G. et al.: Plasma
cytokines following thermal injury and their relationship with patient mortality, burn
size, and time postburD. J. Trauma, 35: 335-9, 1993.
- Houssiau. F.A., Coolie P.G., Van SnickJ.: Distinct roles
ofIL-I and IL-6 in human T-cell activation. J. Immunol., 143: 2520, 1989.
- Schleimer R.P., Rutledge B.K.: Cultured human vascular
endothelial cells acquire adhesiveness for neutrophils after stimulation with
interleukin-1, endotoxin, and tumor-promoting phorol diesters. J. Immumol., 136: 649-54,
1986.
- Cavender D.E., Haskard D.O., Joseph B. et al.:
Interleukin-1 increases the binding of human B and T lymphocytes to endothelial cell
monolayers. J. Immunol., 136: 203-7, 1986.
- Pohlman T.H.. Harlan J.M.: Human endothelial cell response
to lipopolysaccharide, interleukin-1, and tumor necrosis factor is regulated by protein
synthesis. Cell. Immumol., 119: 41-52, 1989.
- Dinarello C.A.: Interleukin-1. Rev. Infect. Dis., 6: 51,
1984.
- Kampschmidt R.F., Upchurch, H.F.: Effect of leukocyte
endogenous mediator on plasma fibrinogen and haptoglobin. Proc. Soc. Exp. B iol. Med.,
146: 904, 1974.
- Baumann H., Richards C., Gauldie J.: Interaction among
hepatocyte-stimulating factors, interleukin-1, and glucocorticoids for regulation of acute
phase plasma proteins in human hepatoma (Hep G2) cells. J. Immunol., 139: 4122-8, 1987.
- Van Damme J., Opdenakker G., Simpson R.J. et al.:
Identification of the human 26-KD protein, interferon beta-2 (TFN-beta 2), as a Bcell
hybridoma/plasmacytoma growth factor induced by interleukin1 and tumor necrosis factor. J.
Exp. Med., 165: 914-9, 1987.
- Vogel S.N., Douches S.D., Kaufman E.N. et al.: Induction of
colony stimulating factor in vivo by recombinant interleukin-I alpha and
recombinant tumor necrosis factor alpha-1. J. Immunol., 138: 21438, 1987.
- Bone R.C.: Let's agree on terminology: Definitions of
sepsis. Crit.Care Med., 19: 973-6, 1991.
- Lefebvre V., Peeters-Joris C., Vaes G.: Modulation by
interleukin-1 and tumor necrosis factor alpha of production of collagenase, tissue
inhibitor of metalloprotemases and collagen types in differentiated and dedifferentiated
articular chondrocytes. Biochim. Biophys. Acta, 1052: 366-78, 1990.
- Cominelli F., Nast C.C., Duchini A. et al.: Recombinant
interleukinI receptor antagonist blocks the proinflammatory activity of endogenous
interleukin-1 in rabbit immune colitis. Gastroenterology, 103: 65-71, 1992.
- Rambaldi A., Torcia M., Bettom S. et al.: Modulation of
cell proliferation and cytokine production in acute myeloblastic leukemia by interleukin-1
receptor antagonist and lack of its expression by leukemic cells. Blood, 78: 3248-53,
1991.
- Richards C., Gauldie J., Baumann H.: Cytokine control of
acute phase protein expression. Ent. Cytokine Netw., 2: 89-98, 1991.
- Hirano T., Yasukawa K., Harada H. et al.: Complementary DNA
for a novel human interleukin (BSF-2) that induces B lymphocytes to produce
immunoglobulin. Nature, 324: 73-6, 1986.
- Aderka D., Le J.M., Vileek J.: IL-6 inhibits
lipopolysaccharide induced tumor necrosis factor production in cultured human monocytes,
U937 cells, and in mice. J. Immunol., 143: 3517-23, 1989.
- Ulrich T.R., Yin S., Guo K. et al.: Intratracheal injection
of endotoxin and cytokines. 11. Interleukin-6 and transforming growth factor beta inhibit
acute inflammation. Am. J. Pathol., 138: 1097-101, 1991.
- Rennick D., Jackson J., Yang G. et al.: Interleukin-6
interacts with interleukin-4 and other hematopoietic growth factors to selectively enhance
the growth of megakaryocytic, erythroid, myeloid and multipotential progenitor cells.
Blood, 73: 1828-35, 1989.
- Helle M., Brakenhoff J.P., De Groot E.R. et al.:
Interleukin-6 is involved in interleukin-I induced activities. Eur. J. Immunol., 18:
957-9, 1988.
- Le J., Vilcek J.: Tumor necrosis factor and interleukin-1:
Cytokines with multiple overlapping biological activities. Lab. Invest., 56: 234-48, 1987.
- Kohase M., Henriksen-De Stefano D., May L.T. et al.:
Induction of beta-2 interferon by tumor necrosis factor: A homeostatic mechanism in the
control of cell proliferation. Cell, 45: 659-66, 1986.
- Strieter R.M., Kunkel S.L., Showell H.J. et al.:
Endothelial cell geneexpression of a neutrophil chernotactic factor by TNF-alpha, LPS, and
IL-I beta. Science, 243: 1467-9, 1989.
- Nawroth P.P., Stern D.M.: Modulation of endothelial cell
hemostatic properties by tumor necrosis factor. J. Exp. Med., 163: 740-5, 1986.
- Pohlman T.H., Stanness K.A., Beatty P.G. et al.: An
endothelial cell surface factor induced in vitro by lipopolysaccharide, interleukin-I and
tumor necrosis factor-alpha increases neutrophil adherence by a CDw 18-independent
mechanism. J. Immunol., 136: 4548-53, 1986.
- Lin H., Chensue S.W., Strieter R.M. et al.: Antibodies
against tumor necrosis factor prolong cardiac allograft survival in the rat. J. Heart Lung
Transplant, 11: 330-5, 1992.
- Carswell E.A., Old L.J., Kassel R.L. et al.: An
endotoxin-induced serum factor that causes necrosis of tumors. Proc. Natl. Acad. Sci. USA,
72: 3666-70, 1975.
- Tracey K.J., Morgello S., Koplin B. et al.: Metabolic
effects of cachectin/turnor necrosis factor are modified by site of production.
Cachectin/turnor necrosis factor-secreting tumor in skeletal muscle induces chronic
cachexia, while implantation in brain induces predominantly acute anorexia. J. Clin.
Invest., 86: 2014-24, 1990.
- Cannon J.G., Tompkins R.G., Gelfand J.A. et al.:
Circulating interleukin-I and tumor necrosis factor in septic shock and experimental
endotoxin fever. J. Infect. Dis., 161: 79, 1990.
- Kawakami M., Murase T., Ogawa H. et al.: Human recombinant
TNF suppresses lipoprotein lipase activity and stimulates lipolysis in 3T3-L1 cells. J.
Biochern. (Tokyo), 101: 331-8, 1987.
- Rodriguez J.L., Miller C.G., Garner W.L. et al.:
Correlation of the local and systemic cytokine response with clinical outcome following
thermal injury. J. Trauma, 34: 684-95, 1993.
- Drost A.C., Larsen B., Aulick H.L.: Interleukin-1 (IL-1)
activity in the serum of burned rats. FASEB J., 3: A319, 1989.
- Kupper T.S., Deitch E.A., Baker C.C. et al.: The human burn
wound as a primary source of interleukin-I activity. Surgery, 100: 409, 1986.
- Schluter B., Kong B., Bergmann U. et al.: Interleukin-6 - A
potential mediator of lethal sepsis after major thermal trauma: Evidence for increased
IL-6 production by peripheral blood mononuclear cells. J. Trauma, 31: 1663, 1991.
- Marano M.A., Fong Y., Moldawer L.L. et al.: Serum
cachectin/tumor necrosis factor in critically ill patients with burns correlates with
infection and mortality. Surg. Gynecol. Obstet., 170: 32,1990.
- Hack C.E., De Groot E.R., Felt-Bersma R.J. et al.:
Increased plasma levels of interleukin-6 in sepsis. Blood, 74: 1704, 1989.
- Guo Y., Dickerson C., Chrest F.J. et al.: Increased levels
of circulating interleukin-6 in sepsis. Blood, 74: 1074, 1989.
- Friedland J.S., Suputtamongkol Y., Remick D.G. et al.:
Prolonged elevation of interleukin-8 and interleukin-6 concentrations in plasma and of
leukocyte interleukin-8 mRNA levels during septicernic and localized Pseudomonas
pseudomallei infection. Infect. Immunol., 60:2402,1992.
| This paper was received on 22
December 1995. Address correspondence
to: Dr S. A. Sheltab El-Din
Plastic, Reconstructive and Burn Unit
Mansoura University Hospitals, Faculty of Medicine
Mansoura, Egypt. |
|

